Reduced vision, blurring or loss of vision (blindness) is the primary concern for a person with any eye problem as well as for the doctor. One should know the possible causes affecting vision, when to take timely action and seek immediate consultation from the eye specialist.
The structure and parts of the eye along with the causes of vision loss are summarized in the figure below.
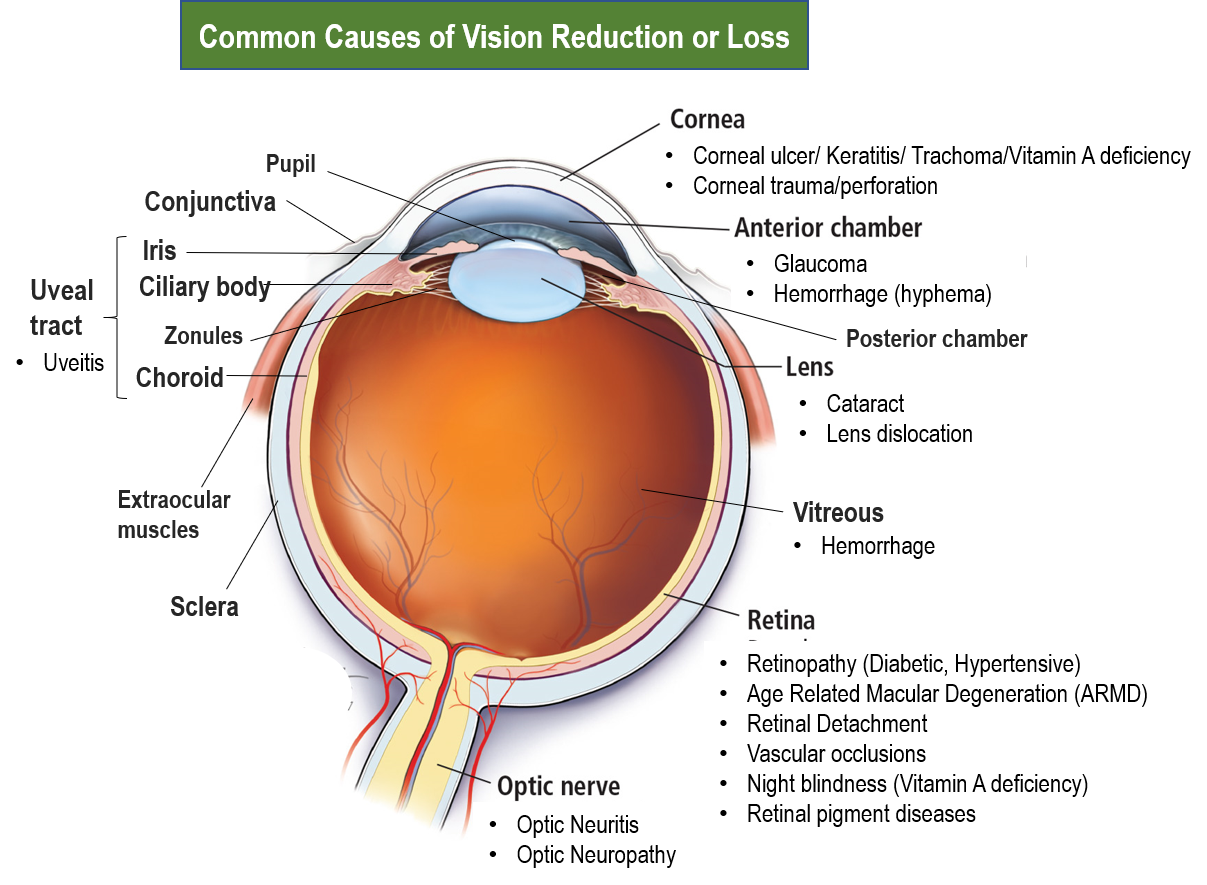


STRUCTURE OF THE EYE
The eyes are actually 2 eyeballs placed in bony sockets called orbits on either side in the skull and coverable by eyelids. The eyeball consists of the transparent cornea in the central front, and the white sclera all around. The exposed part of the sclera in front adjoining the cornea, is covered by a thin membrane layer called the conjunctiva. Extraocular muscles called the recti and the obliques facilitate coordinated eye movement in all directions and eye alignment, a problem of which can lead to squint (strabismus).
Behind the cornea is the iris with a central opening called the pupil. The diameter of the pupil is reduced in bright light (constricted), and increased in dim light (dilated), and this is controlled by the sphincter iris muscle. The iris contains pigment and gives the characteristic ‘eye color’. The iris leads behind into the ciliary body which suspends the lens of the eye just behind the cornea and pupil, with the help of fibers called zonules. Contraction of the ciliary muscle makes the lens more biconvex (fatter or thicker) to view near objects clearly. This is called accommodation which helps in reading and doing near work.
The space between the cornea and iris is called the anterior chamber, and that between the iris and lens is called the posterior chamber. These chambers are connected, and are filled with a nourishing fluid called aqueous. The aqueous drains out of the eye through the angle of the anterior chamber which contains a sieve-like structure called the trabecular meshwork (TM). Any reduction in aqueous drainage due to narrowing of the angle or abnormality in the TM, can lead to an increase in eye pressure, called glaucoma.
The ciliary body continues behind as the choroid which forms the layer behind the retina. The iris, ciliary body and the choroid are together called the uveal tract. The space between the lens and the retina is filled with vitreous (a gel-like transparent substance).
The retina is the innermost back layer of the eye and has an outer pigmented layer and an inner light-sensitive layer (neural retina). The neural retina has photoreceptors called rods (perceive contrast sensors) and cones (perceive color), which are especially present in high density in the central area of the retina called the macula. The macula is responsible for the central, high-resolution, color vision. The retina receives visual signals and sends them through the optic nerve to the brain for the interpretation of vision. The pigment layer of the retina contains protective carotenoid xanthophyll pigments lutein and zeaxanthin, the latter predominating in the macula.
The front 1/3rd of the eye in front of the vitreous is called the anterior segment, while the back 2/3rd is called the posterior segment. The anterior segment includes the cornea, iris, ciliary body, lens and both anterior and posterior chambers (filled with aqueous). While the posterior segment includes the vitreous, choroid, retina and the emerging optic nerve. (So, the ‘chambers’ and ‘segments’ of the eye should not be confused!)
For performing an effective eye examination and to visualize the eye behind the iris for evaluation of cataract, and condition of the vitreous, retina and optic nerve, the pupil of the eye has to be dilated with suitable eyedrops. This may temporarily cause glare and blurring of near vision, till the drug effect wears off in a few hours.
WHEN TO SEEK IMMEDIATE GUIDANCE OF EYE SPECIALIST
This should be done if any of the following sight-threatening signs-symptoms appear:
- Sudden blurring, reduction or loss of vision
- Curtain falling/ red ink filling up perception
- Seeing flashes of light
- Seeing blurred/blind spots
- Seeing large number of floating spots/webs
- Seeing colored haloes around lights
- Increased sensitivity to light or glare
- Seeing double images
- Sudden severe pain in or around the eyes
- Pain on eye movement
- Severe red eyes with swollen lids
- Thick discharge coming from the eye
- Change in color of eyes or white spots
Regular eye screening and check-up is advised in the following conditions:
- Diabetes
- Hypertension (high BP)
- Cardiovascular disease
- Age>60
- Family history of eye diseases
REDUCTION OR LOSS OF VISION
Refractive errors
The presence of spectacle number for distance and/or near are the most common cause of reduction in vision. Some of the signs include:
- Feeling eye strain or blurring more after screen work, reading, or at the end of the day
- Headaches, that are worse at the end of the day and typically felt at the lower part of the forehead and brow.
- Inability to read fine text
- Need to pinch the eyes half shut to see more clearly
- Move near objects or texts away for clarity
Getting a vision test and prescription for glasses from an optometrist/ophthalmologist restores visual clarity and removes eye strain symptoms.
The presence of a minus or plus number is called myopia and hypermetropia respectively, while an asymmetric number is called astigmatism. With increasing age the ability of accommodation reduces due to increasing rigidity of the ciliary muscle of the lens, which is called presbyopia (glasses/ add-on number for reading). These errors are corrected with concave lenses for myopia, convex lenses for hypermetropia and presbyopia, and cylindrical lenses for astigmatism.
There are bifocal glasses where the upper part is for distance and the lower part is for near. These are used when a person develops presbyopia in addition to his distance number. Varifocal or progressive glasses have corrections for multiple distances, mainly distance, intermediate and near, and help those who use laptops and computers regularly.
Cataract
Cataract is the clouding of the lens due to aging and is the most common cause of a gradual decrease in vision in the elderly age group. Rarely cataracts can occur at a younger age due to the use of steroid medicines, diabetes, excessive smoking, radiation exposure or sometimes after lens trauma.
Cataract is treated by surgical removal of the lens and placing a synthetic intraocular lens (IOL). In current practice, this is done as a daycare procedure by phacoemulsification where the cataract is broken down by an ultrasound probe, and removed through a small cut (incision) which makes healing very fast and avoids stitches. Foldable/flexible IOLs are available for insertion through these small incisions.
Glaucoma
This is a condition of an increase in eye pressure causing optic nerve damage and vision loss over a period of time. It occurs due to impaired drainage of aqueous at the angle, due to abnormality of the trabecular meshwork (open-angle glaucoma OAG) or the angle being narrowed/closed (angle-closure glaucoma ACG). ACG can sometimes be acute leading to sudden painful red eye and vision loss.
Glaucoma is diagnosed through an eye pressure check (tonometry), visual fields test for peripheral vision (perimetry), viewing of the angles (gonioscopy), optic nerve damage evaluation by visualizing the optic nerve head (also called the optic disc) by an ophthalmoscope and imaging by optical coherence tomography (OCT).
Glaucoma is treated by various classes of anti-glaucoma eyedrops and medications which act by different mechanisms like lowering aqueous production, increasing aqueous outflow and lowering intraocular pressure (IOP). Surgery (trabeculectomy) may be required in non-responsive cases. In the case of acute ACG, laser iridotomy (creating a small opening in the iris by laser) is done urgently to facilitate aqueous drainage.
Ocular trauma
It is the most common cause of sudden loss of vision. An eye specialist should be immediately consulted in case of any trauma to the eye, as urgent intervention/surgery may be needed in some cases. Eye trauma causing loss or reduction of vision can be due to:
- corneal injury or perforation
- hemorrhage or bleeding
- anterior chamber hemorrhage (hyphema)
- vitreous hemorrhage
- dislocation of the lens
- detachment of a part of the retina
- traumatic optic neuropathy
Note: Blindness after head injury can also be due to damage to the vision area of the brain.
Eye Infections
Conditions that affect the cornea (inflammation of cornea – keratitis, and corneal ulcers), often reduce vision and are painful. These need to be treated immediately with appropriate antibiotic eyedrops/eye ointments. Large corneal ulcers and perforations can cause scarring, formation of corneal opacities, and long-term reduction in vision. Such cases may require a keratoplasty (corneal transplant).
Vitamin A deficiency
This is known to cause severe dry eye (xerophthalmia), corneal ulcers and sometimes clouding and softening of the cornea (keratomalacia). Vitamin A is a part of the rods of the retina that perceive contrast, so its deficiency can also cause night blindness (reduced vision in dim light and low contrast). This is a significant problem in children from underdeveloped or poorer areas and is far rarer today due to the fortification of many food items with vitamin A as well as social programs for both nutrition awareness and administering vitamin A to children.
Retina conditions
Retinal detachment
This can manifest as a sudden visual loss (like a curtain falling) which can be due to trauma or spontaneous (especially in people with high myopia, degenerated retina or prior retinal tears).
Retinal detachment is treated by surgery involving sealing the tears with freezing (cryotherapy) or laser, followed by placing a buckle to attach and hold the retina. This is usually performed by a retina specialist.
Age-related macular degeneration (ARMD)
This is a common cause of gradual progressive vision loss with aging due to deterioration and deposits in the retina especially the macula. Apart from increasing age, other risk factors linked to ARMD include family history, cardiovascular disease and associated obesity and smoking, however many times no particular cause is established. Vision reduction usually central, manifests as inability to work/read in dim light, blurring, dullening of colors, distortion of lines, decreased recognition ability and noticing blind/blurred spots while seeing. Sometimes the presence of abnormal new leaky vessels can cause swelling and bleeding leading to quick deterioration of vision, and the ARMD is then said to be ‘wet’. Otherwise, in most cases the ARMD is called ‘dry’.
Diagnosis is established by ophthalmoscopy, optical coherence tomography (OCT) and angiography with a colored dye like fluorescein (blue) or indocyanine (green), can help identify the leaky vessels.
Dry ARMD is managed with low vision aids, nutritional vitamin-mineral and antioxidant supplements with regular eye check-up and controlling cardiovascular disease risk factors. Wet ARMD is treated by eye injections of medicines that reduce leaky vessels (anti-VEGF drugs: ranibizumab, bevacizumab and aflibercept), and by sealing the leaky vessels with laser (photocoagulation) or using a photoactive drug (photodynamic therapy with verteporfin).
Retinopathy
It occurs due to the damage of the walls of the delicate blood vessels of the retina over time. The most established cause is diabetes (diabetic retinopathy) but it can also be linked to high blood pressure (hypertensive retinopathy) or cardiovascular disease and formation of plaques (atherosclerosis).
The damaged vessels can leak and bleed causing swelling and hemorrhages in the retina, especially the macula (maculopathy). This causes visual deterioration, blurring, distortion and seeing spots. Sometimes abnormal new leaky vessels can grow and bleed significantly (proliferative retinopathy) or an entire major retinal blood vessel may get blocked (retinal vascular occlusion) causing sudden vision reduction or loss.
Treatment involves meticulous sugar control, managing other cardiovascular risk factors including blood pressure, along with retinal angiography. This is followed by laser (photocoagulation) which can be focal for certain leaky vessels, done mainly in the macula region, or scattered all over the retina. Other treatments especially in proliferative diabetic retinopathy include anti-VEGF drugs: ranibizumab, bevacizumab and aflibercept), and photodynamic therapy (with verteporfin).
Retinal pigment diseases
These are rare and can be hereditary with the most well-known being retinitis pigmentosa. Symptoms are gradual reduction in vision especially of contrast, peripheral or night vision. These conditions are diagnosed on a retina examination, and treatment usually involves low vision aids and rehabilitation.
Vitreous hemorrhage
Hemorrhage and leakage of blood in the vitreous is usually caused by proliferative diabetic retinopathy, wet ARMD, retinal detachment or trauma. Vitreous hemorrhage is usually managed by observation for spontaneous clearance. If it is not resolving and is significantly affecting vision, a procedure called vitrectomy may be performed sometimes along with the sealing of the underlying tear/bleeding site with cryotherapy or laser, combined with retinal detachment surgery where needed.
Sometimes black shadowy specks called floaters may appear in front of the eye which move directionally with eye movement and are more prominent against clear backgrounds. These do not need any intervention as these are usually due to protein particles, fibers or blood cells in the vitreous. However, if they increase suddenly and significantly, it may suggest a vitreous hemorrhage or detachment.
Uveitis
It is the inflammation of parts of the uveal tract and includes iridocyclitis (inflammation of iris and ciliary body), and choroiditis (inflammation of the choroid). It can occur post-trauma, infection or surgery, and also be associated with other inflammatory autoimmune conditions in the body like arthritis, ankylosing spondylitis, systemic lupus erythematosus (SLE), sarcoidosis, or inflammatory bowel disease (Crohn’s type IBD).
The symptoms include eye redness, pain, light sensitivity (called photophobia), with blurring or decreased vision, and the presence of floaters in front of the eye.
The treatment includes using corticosteroids as eye drops, or sometimes as eye injections or oral tablets to control the inflammation. In severe cases, stronger immunosuppressive injections may be needed. Eye drops to widen (dilate) the pupil are also given as this helps to relieve pain and reduce the formation of adhesions (called synechiae) between the iris and the lens or cornea. Infection, when present is treated with antibiotics.
Uveitis can present with some short-term and long-term complications. Secondary glaucoma is sometimes seen due to synechiae closing the angle and preventing aqueous flow, or the inflammatory cells clogging the trabecular meshwork. Therefore, eyedrops to lower intraocular pressure may need to be temporarily used. Cataracts can develop due to inflammation as well as the prolonged use of steroid medicines. Choroiditis can sometimes cause inflammation of the adjoining retina (chorioretinitis) which can cause swelling of the retina, especially of the macula (macular edema), leading to a reduction in vision. Chorioretinitis can also cause proliferative retinopathy where abnormal new blood vessels grow on the surface of the retina, which can bleed on the retina or into the vitreous, and cause severe vision loss
Optic nerve conditions
Optic neuritis
It is the inflammation of the optic nerve. It maybe associated with multiple sclerosis, other autoimmune diseases, or infections, but often no cause maybe found.
Symptoms include eye pain which is worsened by eye movement, seeing flashes or flickering of light, along with reduced/loss of vision which can be full, central, one side or color perception.
Ophthalmoscope examination of the optic nerve head, optical coherence tomography-OCT, visual field test (perimetry) and magnetic resonance imaging (MRI)) along with some blood antibody markers are the diagnostic tests.
It is treated with corticosteroid drugs (usually methylprednisolone) given by intravenous injection. Vision usually improves with treatment, but may take a few months to return to normal with residual loss of some vision and/or color perception in certain people.
Optic neuropathy
This condition is sometimes called optic atrophy, and refers to the damage to the optic nerve. This can happen due to different causes like lack of adequate blood supply (ischemia), trauma, radiation, compression by swellings/tumors, infections, toxicity (due to certain drug/alcohol/chemicals/smoking), repeated attacks of optic neuritis, certain nutritional deficiencies (like vitamin B12, B1) and sometimes hereditary/genetic conditions. The symptoms are visual clouding, decrease in visual quality and color perception, and loss of vision over time.
Also read:
For any query, additional information or to discuss any case, write to info@drvarsha.com and be assured of a response soon
References



59 Comments
I am truly grateful to the owner of this website who has shared this wonderful piece of writing at this place.
Remarkable! Its really remarkable article, I have got much clear idea concerning from this article.
Hi, I am also visiting this site regularly, this site is truly nice and the visitors are genuinely sharing nice thoughts.
My partner and I absolutely love your blog and find the majority of your posts to be what precisely
I’m looking for. Would you offer guest writers to write content for you?
I wouldn’t mind producing a post or elaborating on a few of the subjects you write in relation to here. Again, awesome website!
Thankyou Antonietta.. Useful health-related write-ups from qualified professionals are always welcome. Write to info@drvarsha.com
Thanks for sharing your info. I really appreciate your efforts and I will be waiting for your next write ups
thanks once again.
I like how you mentioned that you need to seek immediate guidance when you are experiencing flashes of light. My younger cousin mentioned to me last night that she is having blurry vision and asked me if I have any idea what is the best option to do. Thanks for this informative article and I’ll be sure to get her to a trusted ophthalmologist to figure out what is the problem and give her proper treatment.
Perfectly composed content, Really enjoyed looking through.
Whoah this weblog is fantastic I really like studying your posts. Keep up the good postings! You know, many people are looking round for this info, you can aid them greatly.
Generally I do not learn article on blogs, however I would like to say that this write-up very compelled me to check out and do it!
Your writing taste has been surprised me.
Thanks, very nice article.
Loving the information on this site, you have done outstanding
job on the blog posts.
Hello, I enjoy reading through your article.
I wanted to write a little comment to support you.
Admiring the time and energy you put into
your blog and detailed information you provide.
It’s good to come across a blog every once in a while that isn’t the same outdated rehashed material. Wonderful read! I’ve bookmarked your site and I’m adding your RSS feeds to my Google account.
It’s actually a nice and useful piece of info. I am satisfied that you simply shared this helpful info with us.
Please stay us up to date like this. Thank you for sharing.
Wow, wonderful blog structure! You make blogging glance easy. The full look of your site is great, as
neatly as the content!
I like the valuable information you supply in your articles.
I’ll bookmark your weblog and check again right here regularly.
We’re a group of volunteers and opening a new scheme
in our community. Your site offered us with valuable info to work on. You have done a formidable job and our entire community
will be thankful to you.
Thank you for sharing your thoughts. I truly appreciate your efforts
and I am waiting for your further write ups thank you once again.
I’m not that much of an internet reader to be honest but your site is really nice, keep it
up! I’ll go ahead and bookmark your site to come back later. Many thanks
You ought to be a part of a contest for one of the most useful blogs online.
I will highly recommend this website!
Loving the information on this internet site, you have done outstanding
job on the articles.
bookmarked!!, I love your website!
Fabulous, what a website it is! This website presents valuable data to us, keep it up.
Nice post. I used to be checking constantly this weblog and I’m impressed!
Very helpful information … I used to be looking for this certain information for a very lengthy time.
Thanks and good luck.
Spot on with this write-up, I really believe that this website needs much more attention. I’ll probably be returning to read through more, thanks for the information!
Hurrah! After all I got a blog from where I will be capable of actually getting helpful information regarding my study and
knowledge.
When you mentioned floating spots as something that can affect your vision, I remember something my son told me a few days ago. He said there were “small lights” running around, and none of us in the same room could see something like that at all. If this is something that is affecting his vision, I’ll have an eye specialist examine him right away so we can see what he needs.
I every time spent my half an hour to read this weblog’s articles or reviews all the time along with a cup of coffee.|
This blog is helpful.
I think this is among such a lot of important information for me.
And i’m satisfied reading your article. However want to alsoremark on some common issues, The website look is ideal, the articles are all in fact nice : D. Good activity, cheers
That is the first time I frequented your web page and so far I am amazed with the research you have done to create this portal that is extraordinary.
Magnificent job!
Generally I don’t learn from article or blogs, but I would like to say that from this write-up I did so! Thank you, very great post.
If some one wishes to be updated with most up-to-date info, they must visit this web site.
Thank you for posting such a wonderful article. It helped me a lot.
It is really a nice and helpful piece of info. I am glad that you shared this helpful info with us. Please keep us up to date like this. Thank you for sharing.
This is really a nice Post. And very helpful topics also.
Oһ my goodness! Awesome article dude! Thank you so much..
Great info. Lᥙcky me I reсently found your site by accident (stumbleupon).
I have saved it forr later!
Hi my friend! I want to say that this article is amazing, nice written and include almost all vital infos. I would like to see more posts like this.
Usually I don’t learn from posts or blogs, but I wish to say that this write-up has forced me to try and do so! Your writing style has amazed me. Thanks, quite great post.
Very good information. Lucky me I recently found
your website by chance (stumbleupon). I’ve book marked it for later!
Hello it’s me, І am also ѵisiting this website regularly, this website is really
informative and people are actually sharing faѕtidious thoughts.
Terrific work! This is the type of information that should be shared around the internet. Shame on the search engines for not positioning this post higher!
This article opened my eyes, I can feel your mood, your thoughts, it seems very wonderful. I hope to see more articles like this. thanks for sharing.
Great article, totally what I was looking for.
I like what you guys are usually up too. Such clever work and reporting!
Keep up the terrific works guys I’ve incorporated you guys to my blogroll.
Hi, the whole thing is going nicely here and ofcourse every one is sharing information, that’s truly good, keep up
writing.
Valuable information. Lucky me I found your web site by accident, and I am shocked why this accident did not happened earlier! I bookmarked it.
I could not refrain from commenting. Exceptionally well written!
Hello to all. I think every one is getting more from this site, and your views are fastidious for new users.
It’s very simple to find out any topic on the net as compared to textbooks,
as I found this article at this website.
Awesome article.
Hello! I just want to give you a huge thumbs up for the great info you have got right here on this post.
I am returning to your blog for more soon.
Solid and useful points. Keep up the amazing work.
Hi to all, how is the whole thing, I think every one is getting more from this site, and your views are pleasant for new viewers.
Ahaa, its pleasant conversation on the topic of this article at this place at this website, I have read all that, so at this time I’m also commenting at this place.
I don’t unremarkably comment but I gotta admit regards for the
post on this amazing one :D.
My web-site new88
It’s remarkable to see this web site and reading the views of all colleagues, while I am also getting knowledge.
I’ve read some good stuff here. Definitely worth bookmarking for revisiting. I’m surprised at how much effort you have put to create this sort of magnificent informative web site.