Skin Infections can be caused by bacteria, fungi, viruses, or parasites.
Common predisposing factors for skin infections are:
- improper hygiene
- tight clothes or irritating fabric
- infrequently changed diapers
- heat with moisture (tropical climate)
- cuts, injuries, scrapes, and insect bite
- repeated itching (especially in inflammatory skin diseases like eczema and psoriasis)
- crowded living/schools/workplaces
- poor nutrition
- coexisting diabetes or poor circulation
- underlying immune deficiency
BACTERIAL SKIN INFECTIONS
Bacterial skin infections are the most common. They often involve the hair follicles on the skin (from where the skin hair arises). The causative bacterium is usually Staphylococcus aureus.
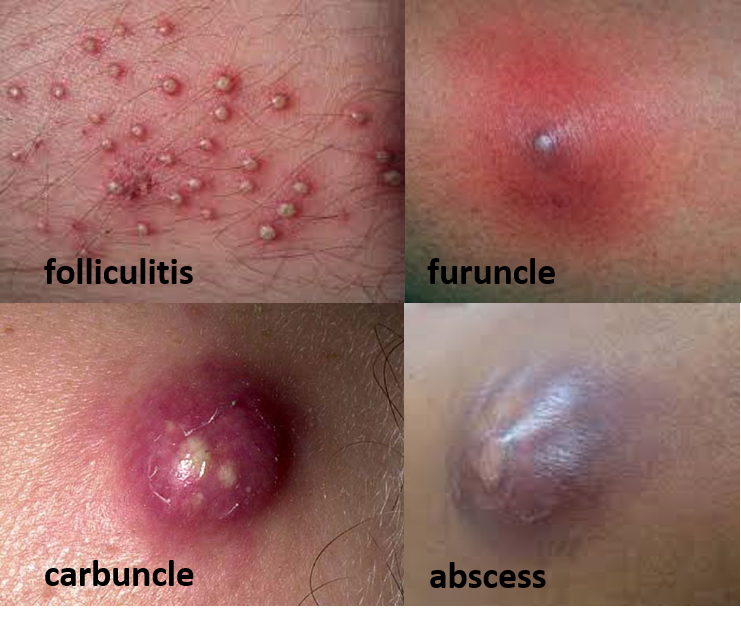
- Folliculitis is an infection of the hair follicle confined to the upper outer layer of the skin (epidermis).
- Furuncle (also called boil) implies a deeper infection in the dermis and appears as a pus-filled bump that is painful on touching.
- Carbuncle is formed sometimes when furuncles join together.
- Skin abscess is a deep pocket (walled off enclosed area) of pus (bacteria, white blood cells, and dead skin cells).


Some skin infections can also be caused by the bacterium Streptococcus pyogenes (Group A Streptococci- GAS) in addition to Staph aureus. This can occur through small breaks and cracks in the skin.
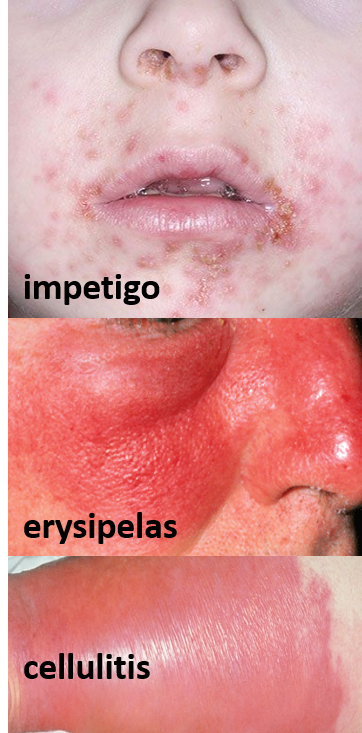
- Impetigo is a contagious skin infection causing red sores. These sores break down to ooze pus in a few days and then form yellow crusted scabs, that usually heal without scarring. Sometimes blisters maybe present (bullous impetigo). Impetigo is commonly seen in young children (2-5 years) around the nose or mouth and on the arms or legs. When impetigo affects deeper skin layers, it is sometimes called ecthyma (deep impetigo). It usually resolves with antibiotics in 7-10 days.
- Erysipelas is an infection involving the epidermis and the superficial dermis along with the draining lymphatics. The affected skin is bright red, firm, painful, and swollen with sharp raised borders. Sometimes blistering, dimpling, surface break down of the skin, or bleeding into the skin (purpura) may also be seen. It is more common in children and the elderly, and can be seen on the face (usually in a ‘butterfly’ distribution) and on the arms or legs. It usually resolves with antibiotics in a few days without scarring.
- Cellulitis is a bacterial infection involving the deeper part of the dermis and subcutaneous layer that can be fast-spreading, serious, and life-threatening requiring urgent medical care. Complications can also rarely occur like abscesses, gangrene, and sepsis. Sometimes other structures may also be infected by the GAS bacteria like blood vessels (thrombophlebitis), joints (septic arthritis), tendons (tendonitis), heart valves (endocarditis), kidneys (glomerulonephritis), and very rarely clots in the brain (cavernous sinus thrombosis).


Treatment
Bacterial infections are usually treated by topical antibiotics like mupirocin, fusidic acid, framycetin, neosporin, clindamycin, or nadifloxacin. Sometimes topical povidone-iodine (Betadine) ointment/cream may also be prescribed. Topical antibiotics alone are usually enough for superficial infections like folliculitis and furuncles. Oral antibiotics like amoxicillin/clavulanate or cephalosporins are prescribed in case of more extensive or deeper infections like impetigo, and erysipelas. Intravenous antibiotics (like vancomycin in resistant Staphylococcus infections -MRSA) are needed in cellulitis and sometimes in erysipelas. Antibiotic treatment duration is usually 7-14 days. Rarely long-term antibiotics may be needed in persistent or recurrent infections like erysipelas.
An abscess often requires incision and drainage. Supportive treatment includes dressings, wet compresses for removing crusts, medicines to reduce pain and inflammation, and improvement of skin hygiene.
FUNGAL SKIN INFECTIONS
TINEA
The most common fungal skin infections are superficial and caused by the mold like or filamentous fungus Tinea (condition is called Dermatophytosis). Predisposing factors include the triad of heat and moisture, restrictive or irritant clothing/soiled diapers, and poor hygiene. It is characterized by skin redness and itchy rash (prominent itchiness differentiates fungal from bacterial skin infections). Sometimes the rash may show scales, blisters, and crusts.
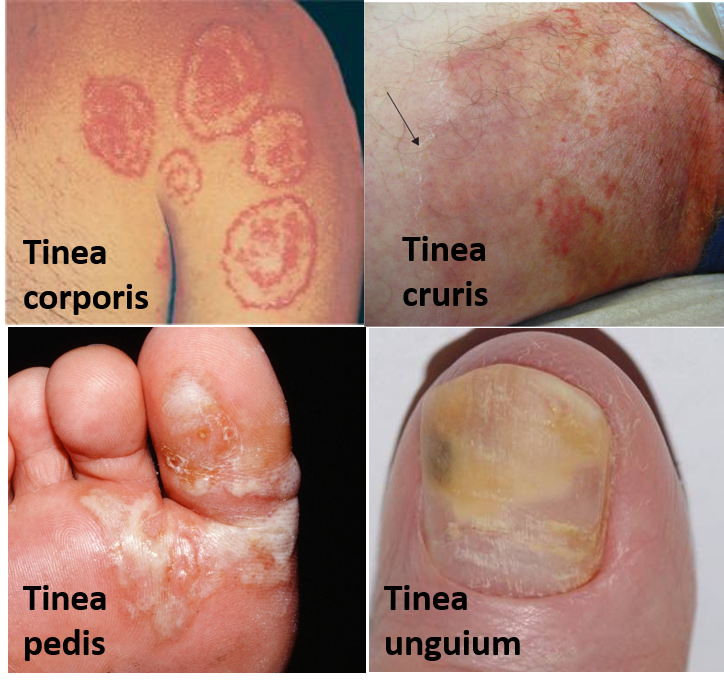
Tinea infections are named according to the part of the body involved as shown in the figure. For example, Tinea corporis involves the body and causes a typical appearance known as ringworm (progressing active border of the rash with central clearing – also called tinea circinata or tinea glabrosa). Tinea cruris commonly known as crotch itch, gym itch, jock itch and ringworm of the groin (seen more common in men). Tinea pedis is also called athlete’s foot as it is common in athletes who are sweating in socks-shoes for long hours. Tinea unguium (onychomycosis) is a fungal infection of the nails that causes discoloration, thickening, and separation from the nail bed.


These infections are treated by antifungal drugs. Those commonly used are
Topical antifungals:
- Imidazole group (clotrimazole, miconazole, sertaconazole and luliconazole): These are available as creams, lotions, solutions/suspensions or powders. For scalp infections, ketoconazole and sertaconazole are available as shampoos/scalp lotions.
- Allylamine group (terbinafine and amorolfine): Terbinafine is available for both topical and oral use, and as a nail lacquer. Amorolfine is available as a cream and as a nail lacquer for onychomycosis.
- Ciclopirox: It is available as a topical solution/suspension, cream and nail lacquer but is less popular than the others mentioned.
Oral antifungals: These may also be needed in case of more severe, recurrent or persistent infections, for which the triazole group (fluconazole and itraconazole) or terbinafine are commonly used.
Antifungal treatment duration: It may range based on the type and location of the infection. Tinea corporis usually needs 1-2 weeks while Tinea cruris and capitis may need 2-4 weeks. Tinea pedis may need up to 6 weeks, while Tinea unguium may require 3-6 months treatment.
Supportive care includes proper hygiene, and keeping the area dry and aerated.
MALASSEZIA
This fungus (formerly called Pityrosporum) is a yeast like fungus present as part of our skin flora. It can sometimes cause skin rash, itching and discoloration.
Excess and persistent dandruff (small pieces of dry skin flakes from the scalp) is associated with Malassezia.
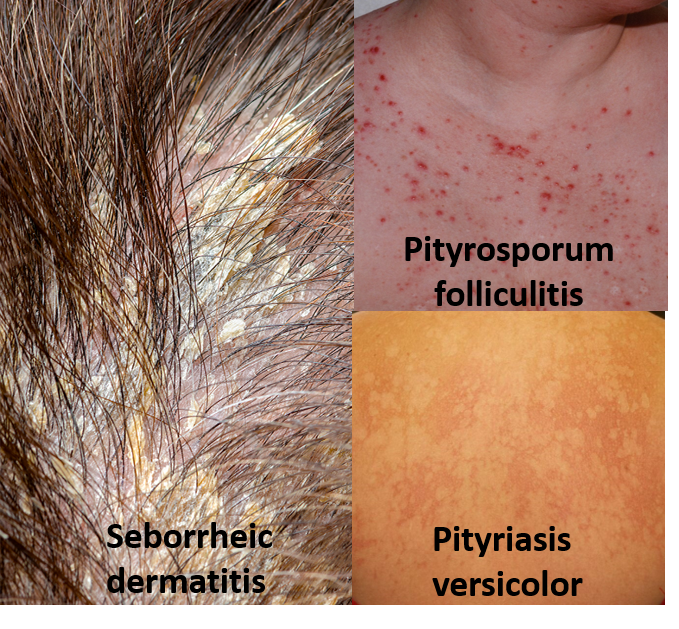
Seborrheic dermatitis (‘seborrhea’ implies excess sebum which is the oil produced from the hair follicle sebaceous glands) is a condition presenting with greasy and itchy patches with flaky white/yellow scales or crust on the hairy areas like scalp, face, eyebrows, eyelids (blepharitis), ears, nose, chest, armpits, groin or under the breasts. Seborrheic dermatitis is sometimes also called seborrheic eczema. The treatment involves frequent washes with anti-dandruff shampoo/scalp lotions. These contain zinc pyrithione, selenium sulfide, antifungal agents like ketoconazole or sertaconazole, and sometimes keratolytic agents to remove scales like coal tar or salicylic acid. Treatment may be required from a few weeks to few months.
Pityrosporum folliculitis is the term used to describe the infection by Malassezia of hair follicles producing excess sebum. This may sometimes be hard to distinguish from bacterial folliculitis or acne. However, presence of itching favors the diagnosis of Malassezia (but sometimes diagnostic culture and microscopy tests may be needed). Pityrosporum folliculitis does not respond to antibiotics or acne medications, and requires topical antifungal creams or lotions.
Pityriasis versicolor (formerly misnamed Tinea versicolor due to its resemblance to Tinea corporis) is a rash caused by Malassezia that appears patchy in color due to skin pigment production irregularity. This is also treated by antifungal creams and lotions.


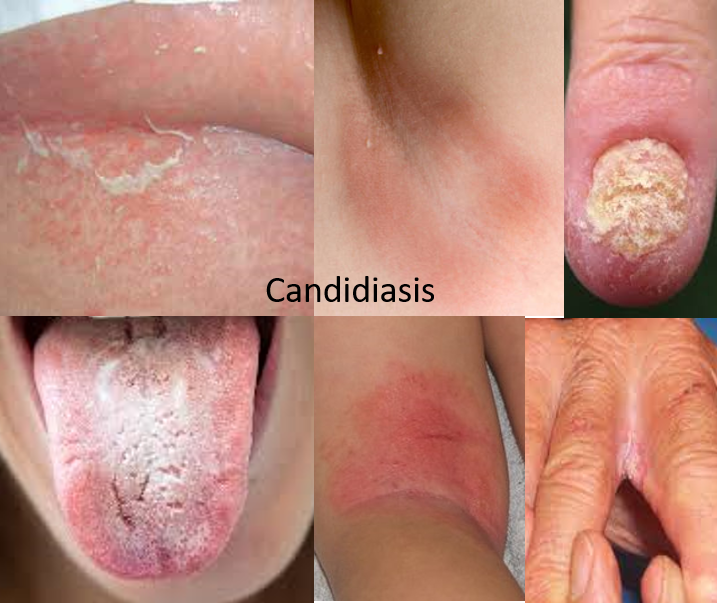
CANDIDA
Candida is a yeast like fungus and its infection is more common in babies (cause of diaper rash), and in people with coexisting conditions like diabetes, obesity (more sweaty, unexposed skin creases), prolonged antibiotic use, and weakened immunity due to corticosteroid use, chemotherapy or conditions like HIV. It commonly causes infections of the skin (cutaneous candidiasis), mouth (oral thrush) and vagina (vaginal candidiasis). It leads to a red, itchy rash or patch that can bleed on scraping. It occurs in skin creases and folds (intertrigo), armpits, groin, and nails.
It is treated with topical antifungals (clotrimazole, miconazole, sertaconazole or nystatin) and if required oral antifungals (fluconazole or itraconazole) till resolution of symptoms.


Important Points
Sometimes bacterial and fungal infections may coexist as predisposing factors are often common. Itching in fungal infections can also lead to a secondary bacterial infection. It may be difficult to distinguish bacterial and fungal infection in some cases, especially in case of the presence of other skin inflammatory conditions. Therefore, there are several topical combination creams and ointments of antibiotic and antifungals available and these are often prescribed in practice. However, these combinations should be used judiciously, and not as an alternative to making a correct diagnosis, as irrational usage can lead to antimicrobial resistance.
Itching, skin irritation and rash can sometimes be distressing, and there is need for early symptomatic relief. This is especially true when infections occur in the presence of eczema (dermatitis – skin inflammatory conditions). In such cases, topical corticosteroids are also prescribed. There are several topical triple combinations of antibiotic-antifungal-corticosteroid available. However rampant use of such combinations can sometimes lead to worsening or persistence of the infection. Therefore, these combinations should not be used irrationally or as over-the-counter treatments.
Skin care and hygiene is the cornerstone for preventing and managing bacterial and fungal skin infections.
VIRAL SKIN INFECTIONS
A variety of viruses can affect the skin, and they cause contagious infections. A weakened immune system predisposes more to viral skin infections.
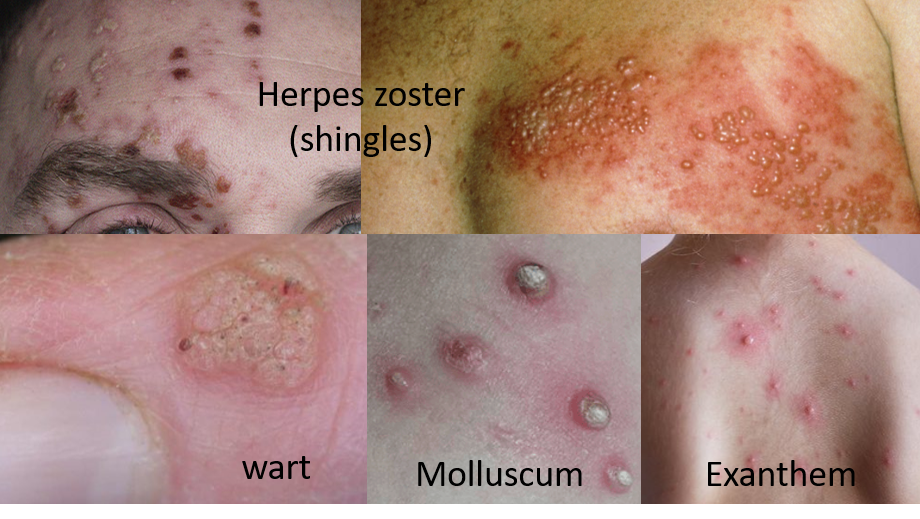
Shingles (Herpes zoster-HZ) in adults is caused by the same virus which causes chickenpox called varicella zoster. This is a type of herpes virus that can remain dormant in our nervous system for years and get activated later in life due to stress and immune factors. It produces a red, painful/burning, itchy rash with blisters on one side of the trunk, neck, or face. Sometimes fever, headache, and weakness may be associated. It usually clears spontaneously in 2-3 weeks but the pain/burning may linger on (post-herpetic neuralgia – PHN) for 1 or 2 months, rarely longer. If the rash is near or involving the eye/ear, immediate treatment is needed to avoid effects on vision/hearing. HZ is treated with oral antiviral medications (acyclovir, famciclovir, valacyclovir) for 7-10 days. PHN is treated with a combination of local anesthetics and capsaicin, and oral drugs like amitriptyline/nortriptyline and pregabalin/gabapentin, tramadol and sometimes opioid analgesics.
Viral warts are caused by human papillomaviruses (HPV) and are fleshy, painless outgrowths on the skin, commonly seen in the hands, feet and genitals. They can occur at any age, and are usually benign and harmless. Treatment includes topical medications like salicylic acid, cantharidin or injecting bleomycin, and by procedures like cryotherapy (freezing), laser, curettage (scraping/scooping) or excision (total removal).
Viral exanthems are rashes and eruptions with fever due to viral infections. These are more common in children and usually spread rapidly due to close contact in school. The viruses causing measles, chickenpox, and HFMD (hand, foot and mouth disease) are more common in young children, and manifest as itchy skin rashes and eruptions on the skin and mouth, with fever. However, vaccination being available for measles and chickenpox has greatly reduced the same. Viral exanthems are self-limiting and do not need treatment. Repeated itching can lead to viral spread, secondary bacterial skin infections and prevent sleep. In such cases, calamine lotion or oral antihistamines may be prescribed.
Molluscum contagiosum is a virus, also more common in children, that produces small bumpy, usually painless eruptions with waxy looking centers, that disappear spontaneously, generally without scarring. Sometimes the bumps can last for a few months to years. Usually, no treatment is required but in case of large bumps, treatment with cryotherapy, curettage, laser and acid peels are available.


PARASITIC SKIN INFECTIONS
These include conditions like scabies, lice and bedbugs.
Lice in the hair is a common problem, especially in school-going children. It produces severe itching of the scalp, and the lice can sometimes be seen on hair inspection or come out in the comb. Wet combing with fine-tooth comb 3 times a week is an effective solution. In severe cases, medicated shampoos would be needed which contain permethrin, pyrethrin, ivermectin, lindane or malathion. These should be used preferably under medical supervision. Pillows, bed linen, hair accessories and combs should be soaked in hot water for 5-10 minutes and then washed.
Scabies is an itchy skin condition caused by a burrowing mite called Sarcoptes scabiei. Itching occurs in the area where the mite burrows, which is intense in the night as the mites come out. Scabies spreads very fast through close physical contact in households/ schools. The most common symptom of scabies is intense itching in the area where the mites burrow. Scabies can be treated by killing the mites and their eggs with medication like 5% permethrin cream (most common),10% crotamiton cream, 25% benzyl benzoate lotion, sulfur (5%-10%) ointment or 1% lindane lotion. These should be applied from the neck down and left on for eight hours (overnight) and washed off. The entire family should be treated, and the treatment repeated again a week later. All linen should be washed after soaking in hot water for half-hour.
Bed bugs should be suspected if there is itching and irritation of the skin during sleeping on the bed. Sometimes bugs can also be spotted. The bug bites appear as small red itchy bumps on the skin. Usually, no treatment is needed except calling pest control professionals to do a thorough medicated treatment of the affected beds, and deep washing of the linen.
Also read:
For any query, additional information or to discuss any case, write to info@drvarsha.com, or leave a comment, and be assured of a response soon.
References: CDC Skin infections


6 Comments
Most people I talk to have no clue that shampoos that grow your hair faster and longer (of course with no sulfates, no parabens, no DEA) even exist. Hair styling enthusiasts can now possess longer hair and attain more possibilities. For sure worth investigating.
If you’re discussing alopecia, hair damage, preventing skin disorders, fast hair growth, hair care at large, very similar rules actualize.
Generally, you will want to steer clear of hair products and treatments that contain chemicals like parabens, DEA or sulfates.
What is beneficial for your hair is good for your skin all the same.
It goes without saying your content here is spot on for many reasons. It steers away from the common mistakes and mistakes too many fall into- getting horrible alternatives. Thank you!
It was helpful when you said that antibiotics can help. My sister has been dealing with folliculitis for a couple of weeks now, and she wants to look into finding treatment for it. I’ll pass this information along to her so that she can look into finding the right treatment for folliculitis.
Informative blog! Everyone should be aware about the skin infections, their symptoms, and their treatment. Thanks for sharing it 🙂
It’s awesome for me to have a site, which is beneficial in support of my experience. thanks
Spot on with this write-up, I truly think this website needs far more attention. I’ll probably be returning to read more, thanks for the info!
Greetings! Very useful advice within this article! It is the little changes which will make the most significant changes. Many thanks for sharing!