Post-COVID care and awareness are very important, and an area of continued research and learning.
The term ‘recovered from COVID’ is technically accorded to those who have been free of fever (>100 deg F) for 3 consecutive days with normal oxygen saturation after a minimum of 10 days (7 days for Omicron) from COVID symptom onset. This implies recovery from the infection and active ongoing inflammatory damage. Therefore, this time frame can be 7-14 days for people who had mild disease and were in home treatment, and longer (2-4 weeks) for people with moderate-severe disease who were on oxygen therapy and hospitalized.
However, healing of the body from the impact of COVID is a longer, gradual process, and may take a few weeks to months. The 3 months post COVID recovery is important for observation, recouping, and rehabilitation. COVID can have an impact on multiple organs of the body including the lung, heart-blood vessels, and brain. Sometimes the impact of COVID on the body may be experienced even longer than 3 months when it is called ‘long COVID’.
POST-COVID SYMPTOMS
These are some of the symptoms seen in many people for several weeks post-COVID. It is important to know that most of these common symptoms improve and go away with time and should not become the cause of undue stress, strain, anxiety, or depression. However, one should keep one’s treating physician informed of these symptoms for reassurance and appropriate action where needed.
- Weakness, tiredness, fatigue, low energy levels
- Headache
- Body ache
- Feverish feeling (especially towards the end of the day with temperatures 99 deg F and above but below the 100 deg F fever mark)
- Indigestion, low appetite and nausea
- Subnormal taste/smell
- Feeling breathless after physical exertion
- Palpitations
- Anxiety-depression
- Brain fog (forgetfulness, feeling mentally less sharp)
- Insomnia (sleeplessness)
Immunity may be suboptimal after suffering from COVID and even more so if medicated with steroids, immunosuppressant drugs and antibiotics, if hospitalized for COVID, or if having diabetes or immunosuppressive comorbidities. It is important to be aware and watch out for symptoms of other infections especially Mucormycosis that was seen with the delta variant in the 2nd wave, and report any new or suspicious symptoms immediately.
Rarely post-COVID stroke, heart problems, venous thrombosis, and effects on other body organs have been seen. There is still more research underway on this. Alarm or red flag symptoms which require immediate medical attention are those which are sudden and not witnessed before:
- numbness or weakness in the face, arm, or leg, or one side of the body.
- confusion, trouble in speaking or understanding speech.
- severe unbearable headache
- vision problems
- loss of balance, or coordination
- chest pain
- breathlessness which is severe or along with cough
- swelling, cramping pain, or discoloration in limbs
- persistent bone-joint pains
GENERAL HEALTH CARE
- A nutritious preferably home-cooked diet with plenty of vegetables, fruits, proteins (pulses, soy, boiled eggs, chicken/fish), and curd should be taken.
- Drink at least 1.5 liters of water daily, along with other fluids like coconut water, buttermilk, fresh fruit juices and herbal tea.
- Have meals on time, chew thoroughly, and eat at a relaxed pace.
- Avoid foods high in sugar and refined flour (aerated carbonated drinks, and packaged/junk food).
- Continue prescribed nutritional supplements as directed by the doctor.
- Give up smoking. Limit alcohol to not more than 1 small glass twice a week.
- Take adequate rest with at least 8 hours of uninterrupted night sleep and 1-2 hours of additional rest during the day.
- Take up a relaxing hobby like reading, music, crafts, etc. or join a like-minded social group. Avoid stressful and disturbing online or media content.
- Mental health needs special attention. Post-COVID stress disorder (PCSD) is now a recognized condition with symptoms of anxiety, fear, difficulty sleeping, feeling edgy, unpleasant flashbacks, low moods and outbursts, feelings of guilt, being forgetful, and losing the ability to enjoy. Counseling services and psychotherapy are available and can be very helpful in relieving and managing PCSD and anxiety-depression.
- Vaccination if incomplete or not done, should be taken 3 months post-recovery.
IMPROVING LUNG FUNCTION
‘Stiff lungs’ and reduced oxygen delivery/breathing capacity are common after COVID. This is due to the inflammation of the lung and resultant scarring (fibrosis). While most of it is temporary and resolves over 2-3 months, in some cases it may be severe and even permanent. Some people may need intermittent oxygen therapy at home with oxygen concentrators after being discharged from the hospital.
- Simple breathing exercises like pranayama (alternate breathing) can be done twice daily.
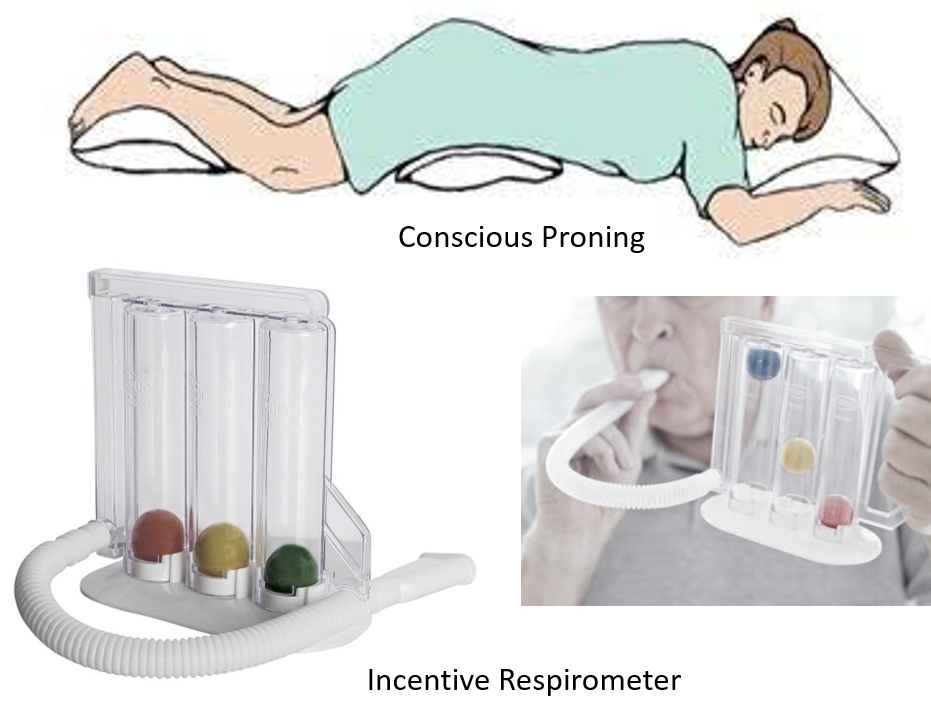
- Continue proning twice daily for half-hour morning and evening, with 10-15 deep breaths 10-15 minutes apart.
- Oxygen saturation should be checked at least once daily before and after physical exertion.
- A home incentive respirometer can be used (for 5-10 minutes twice daily) as shown. These have chambers of different breathing capacity, and one can gradually aim to reach the stage of lifting all three balls over 3 months starting with the first one in the first month. This should be done without strain and stopped if breathlessness, light-headedness or chest pain is perceived at any point.
- It is best to consult your physician before initiating any rigorous breathing exercise.


PHYSICAL ACTIVITY AND EXERCISE
- Resume physical activities in a gradual and graded manner.
- Limit working hours initially and increase the duration of work gradually by an hour every week.
- Take a 15-minute to half-hour break for rest after 2-3 hours of housework or professional work.
- Do not resort to strenuous exercise like jogging, running, cycling, swimming, or going to the gym immediately.
- Start with less rigorous exercises like simple stretches, guided yoga, outdoor walking at a normal pace, and spot exercises for neck-shoulder, arms, legs, and belly. Then step up gradually every week to reach your normal level of physical exercise over 3-6 months.
POST-COVID TESTS
You may be advised certain tests in your post-COVID period depending on the severity of the disease that you had, medicines that had been prescribed, associated comorbidities and risk factors present, and current symptoms and state of health. These tests are not routinely required for everyone and should be done only after evaluation and recommendation by the treating physician. These may include:
- Blood pressure check
- Blood tests to check CBC, sugar, kidney and liver function, lipids, and other inflammatory/coagulation markers where needed.
- ECG and 2D Echo to check heart function.
- Imaging tests like X-ray and Chest CT scan to assess the extent and improvement of lung damage.
- Spirometry to check breathing and lung function.
Note: Post recovery repeat RT-PCR or antibody tests are not routinely needed.
Also read:
Post-COVID Cardiovascular Effects – Know the Symptoms and Causes
3 Effective Techniques to improve Breathing capacity and control
References:


6 Comments
great and amazing blog site. I truly wish to thank for offering us far better info.
I have discovered excellent articles here. I love the way you write. Great!
excellent and outstanding blog. I actually wish to thank you,
for offering us much better information.
Helpful information. Lucky me I found your site accidentally, and I am shocked why this coincidence didn’t took place in advance!
I bookmarked it.
I need to to thank you for this fantastic read!! I absolutely enjoyed every little bit of it. I have you book marked to look at new stuff you post…
Hey very nice blog!