We sometimes suffer from a burning feeling in our stomach area or lower chest, which we describe as ‘acidity’ or ‘heartburn’.
Quick Read – 5 Tips to reduce Acidity
ACID IN OUR STOMACH
The stomach is the organ of our digestive system that produces acid (Hydrochloric acid). The purpose of this acid is 2 fold – firstly to create the required acidic environment to activate the protein digestion enzyme called Pepsinogen, and secondly, to destroy a number of harmful germs and infective organisms that come into our body by way of food/mouth.
Therefore, the acid in the stomach has an important role. Some amount of ‘basal acid’ is always present in the stomach, while the acid release is greatly stepped up during – a) stimulation by seeing/smelling/tasting food, around mealtime due to conditioning, b) when protein substances from the food enter the stomach, and c) during stress. The acid returns to basal levels once any of these stimulations stop.
TYPES OF STOMACH CELLS AND ACID PRODUCTION MEDIATORS
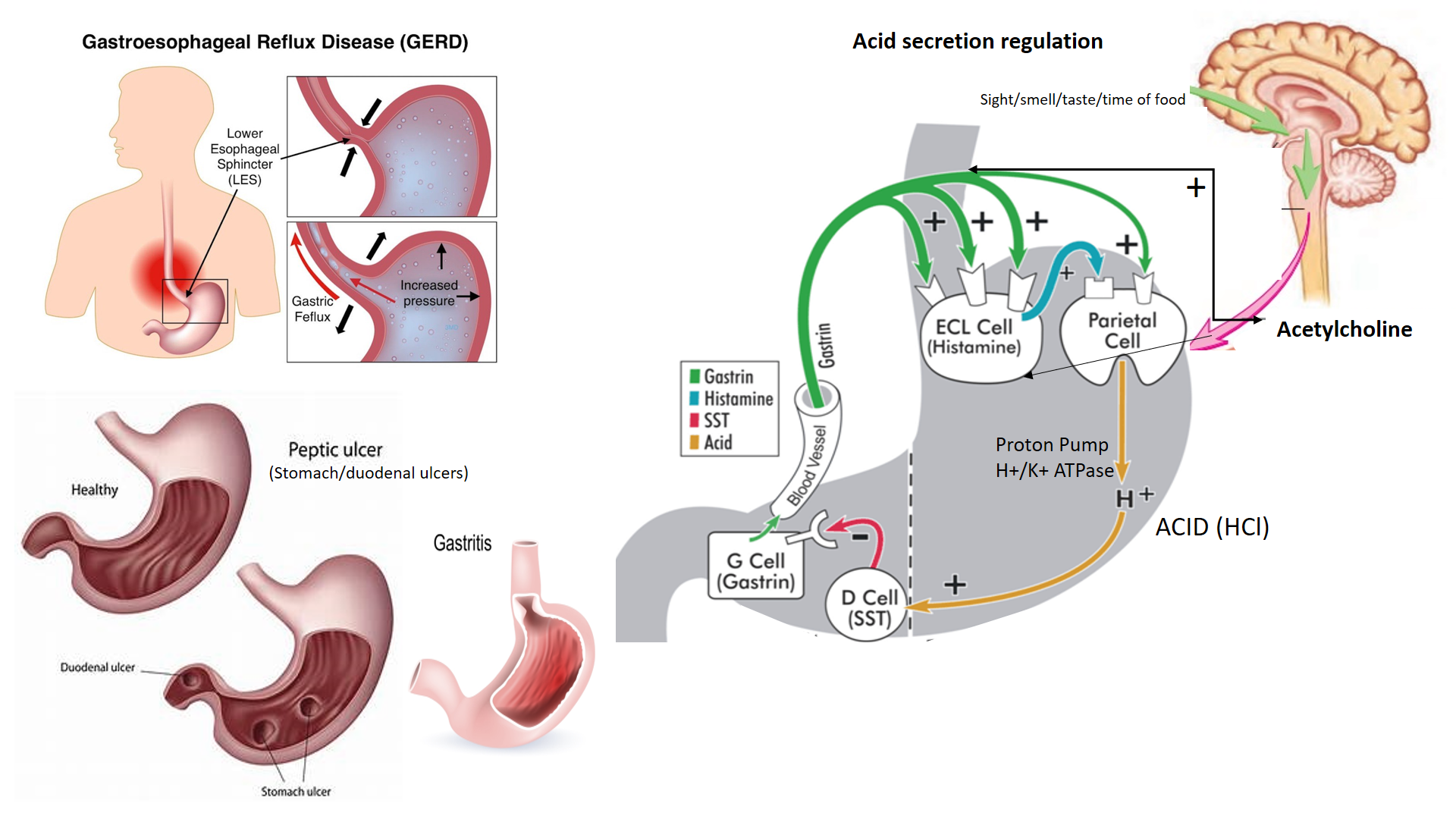
The acid of the stomach is produced in the parietal cells through the proton pump (H+/K+ATPase). In addition to acid, these cells also produce a factor (called intrinsic factor) which helps to absorb vitamin B12. The acid acts on the chief cells to activate the protein digestion enzyme pepsinogen to its active form called pepsin.
Normally the cells lining the stomach lumen are protected from the acid by an alkaline mucus (containing bicarbonate) released by mucus cells (also called goblet cells). In addition, substances called prostaglandins (PGs) also play a protective role against acid damage of the stomach (gastric) lining cells.
Acid production is stimulated by 3 important mediating substances acting on the proton pump-
a) Acetylcholine – Released from nerves in response to signals from the brain receiving sensations of sight/smell/taste, or signals of any physical/mental stress, this substance also increases saliva production.
b) Histamine – Released from ECL cells of the stomach, it helps to maintain basal acid secretion but also increases release in response to stress.
c) Gastrin, released from G cells in response to the presence of protein food entering the stomach.
Both acetylcholine and gastrin act to increase acid secretion directly and also by increasing Histamine.
A substance called somatostatin (SST) is released from D cells of the stomach, in response to sensing too much acid in the stomach and it acts by suppressing gastrin-mediated acid release. It is important to note that histamine is a substance released in the body in response to irritants and allergens causing symptoms like sneezing, running nose, red eyes and itching, but these actions happen through H1 receptors. The histamine in the stomach exerts its action through H2 receptors. So for allergic symptoms, we use H1 anti-histaminic drugs while for controlling acidity we use H2 anti-histaminic drugs.


WHAT CAUSES ACIDITY?
‘Acidity’ is a feeling of a burning pain which can occur due to 4 mechanisms or their combination:
Increased presence of acid in stomach–
This can happen if one does not eat when hungry or during conditioned meal times, or tends to eat hurriedly, irregularly, or under pressure. Acid production is also increased during and due to physical or mental stress, as well as anxiety. (ZE syndrome is a rare condition of a Gastrin releasing stomach tumor causing hyperstimulation of acid production)
Acid refluxing back into the food pipe (esophagus) –
Where the food pipe enters the stomach, there is a valve-like mechanism called the LES (Lower Esophageal Sphincter) which prevents stomach contents from refluxing back into our food pipe (esophagus). Swallowing of food and saliva also helps to prevent such reflux, as it pushes food towards the stomach, along with the advantage of the saliva being more alkaline in nature.
However, when we lie down to sleep, the LES relaxes, the swallowing decreases, and even the advantage of gravity pushing food down is lost. So acid reflux and heartburn are common at night-time, and some relief is obtained by sitting upright. Heartburn can also occur during the day during transient relaxations or decreased tone of the LES. An increase in weight or obesity and a sedentary lifestyle can increase LES pressure, making it more lax, and thereby predisposing to acid reflux.
Heartburn and feeling of acid regurgitation/backlash in mouth constitute the Gastro-Esophageal Reflux Disease (GERD), also called Reflux Esophagitis. This causes a burning sensation in the lower chest called heartburn sometimes along with belching, acidic taste in the mouth, and hoarseness.
Slow emptying out of stomach contents-
The term dyspepsia (commonly called indigestion) is used to describe the feeling of discomfort in the stomach which can include the feeling of acidity, or gas with fullness-bloating, or a combination of these symptoms.
Sometimes the movement of the food from the stomach to duodenum may be slow (gastric hypo-motility) resulting in more prolonged exposure of stomach lining cells to the food with increased acid (decreased acid clearance), along with increased chances of reflux into the food pipe.
In such patients there may be symptoms like early satiety (feeling full prematurely before completing meal), post-prandial fullness (feeling full-uncomfortable just after a meal), bloating (feeling full with a sensation of gas most of the time) along with the tendency for constipation, and sometimes nausea and rarely vomiting.
In the absence of any specific cause found for these symptoms, the condition is called functional dyspepsia. People with diabetes more commonly have significantly slow emptying of stomach contents (diabetic gastroparesis) and have vomiting more commonly along with dyspepsia symptoms. People with depression also more commonly have gastric hypo-motility.
Damage to stomach lining cells –
Inflammation and injury of the lining cells of the stomach is called gastritis. Gastritis may be acute (sudden and short duration) due to eating irritant foods (spicy/deep-fried foods, acidic beverages, large amounts of alcohol), or due to contaminated food (food poisoning) when it may also be associated with nausea, vomiting, or diarrhea (gastroenteritis). Gastritis could become chronic with inappropriate dietary habits and lifestyle factors like smoking, regular alcohol consumption, and stress.
Steroid medicines decrease the production of the protective mucus and also increase acid secretion through histamine stimulation especially in response to stress. NSAID medicines block the production of prostaglandins which also increase the damage to stomach lining by acids. These medicines, therefore, are also causes of gastritis and ulcers.
Helicobacter pylori are bacteria that can be present in the stomach and cause inflammation of the lining cells. Infection of the stomach with H. pylori does not necessarily cause illness, and over 50% are asymptomatic. But persistent presence and colonization can cause chronic gastritis, ulcers, and increase the risk of developing gastric cancer.
ULCERS AND ACIDITY
Ulcers occur due to acid-induced damage and discontinuity of the lining of the lower part of food pipe in GERD (erosive esophagitis), stomach (gastric ulcers), and sometimes the first part of small intestine (duodenal ulcers) which are all exposed to the stomach acid. These ulcers manifest as acidity symptoms and burning pain, which may be aggravated or relieved by meals depending on the location. Sometimes an ulcer may perforate through which can cause severe pain, massive bleeding and infection, while the aftermath scarring can cause a stricture (narrowing/obstruction) leading to difficulty in passage of food.
Sometimes during a stressful episode like hospitalization/prolonged illness or post-surgery, there is damage to the stomach lining cells, decreased capacity to produce mucus, and stress-induced increased acid production all leading to the development of ‘stress ulcers’ in the stomach.
Acid Peptic Disease is an umbrella term to include GERD, gastritis, ulcers (esophageal, gastric, duodenal) and the rare ZE syndrome, which are all conditions caused by acid-induced damage.
Alarm or red flag signs–
These include the following, and the presence of any of these should prompt an immediate consultation.
- recurrent vomiting episodes
- blood in vomit
- weight loss
- weakness or paleness
- difficulty in swallowing with a feeling of food getting stuck in the chest
- feeling a lump in the stomach area
- severe abdominal pain.
HEALTH SOLUTIONS FOR ACIDITY
The solution lies in implementing diet and lifestyle modifications and assessing response after 3 months. Medicines can be additionally taken in case of inadequate response, severe symptoms, diagnosis of ulcers or during a short defined period of stress.
DIET AND LIFESTYLE
If you tend to suffer from acidity symptoms recurrently or over a prolonged period, a relook at your diet and eating patterns is recommended. Diet consists of reducing and restricting the consumption of certain foods while including more of certain other food items.
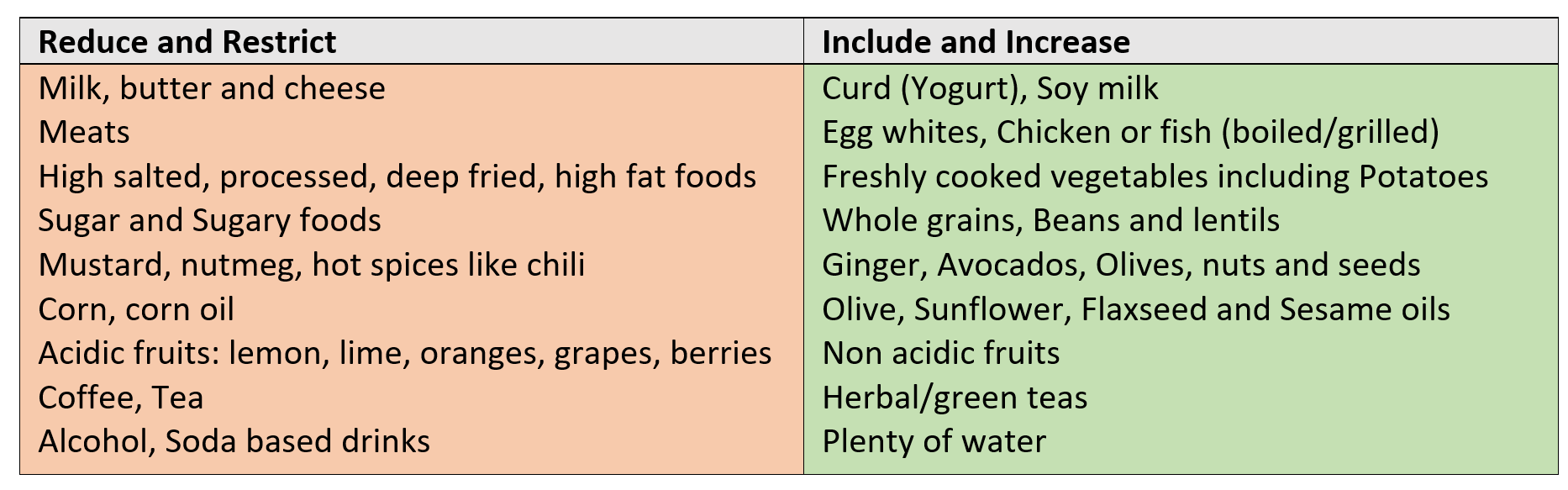


Main meals should be taken at regular time with a small snack every 2-3 hours (one between breakfast and lunch, and one between lunch and dinner – mid-evening). Keep a gap of a minimum of 2 hours between lying down/bedtime and dinner.
Avoid skipping meals, unduly delaying meals, or having hurried meals. Chew thoroughly and enjoy your food. Avoid gulping down food with water.
Include half-hour of exercise (5 days/week) in your lifestyle – swimming, brisk walking, cycling, jogging, yoga, or aerobics. If sitting for prolonged periods of time, take a short walk and do some stretching every 2 hours.
Adequate and good quality sleep is the best natural de-stressor. However, including relaxation techniques in daily routine can reduce unwanted acid stimulation like deep breathing exercises, indulging in hobbies like reading, music, dance, gardening, sports, crafts-work, and time with family and friends.
MEDICINES
Medicines for acidity are loosely clubbed as antacids. These may be drugs to suppress acid production or act by other ways to provide symptomatic relief. Before starting medicines, or based on response to medicines, investigations like endoscopy and testing for Helicobacter pylori infection may be performed to visualize the presence of ulcers and confirm the diagnosis.
Acid Production Suppressors
Medicines to suppress Acid production can act against 3 important steps in acid production:
Proton Pump Inhibitors (PPIs)
These medicines act directly on the final step of acid production in the parietal cells of the stomach. They have become the most prescribed and used medicines for acidity, especially GERD and peptic ulcers. They should be used if acidity symptoms are severe, prolonged, or non-responsive to lifestyle-diet modifications.
PPIs are the drugs of choice when an ulcer has been diagnosed, to aid in its healing and prevent complications or relapse. They are also the drugs co-prescribed with the NSAID class of drugs used for pain and inflammation, and along with antibiotics for Helicobacter pylori infection.
Available PPIs include pantoprazole, rabeprazole, esomeprazole, omeprazole, lanzoprazole, dexlanzoprazole, and ilaprazole
PPIs are given once a day usually half-hour before breakfast or dinner depending on the prominence of symptoms during day or night. They may be given twice a day to give better acid suppression for ulcer healing or to prevent night time acidity (called- nocturnal acid breakthrough NAB). They are usually given for 4-8 weeks, followed sometimes by another 4-8 weeks if the response is inadequate, and thereafter at a maintenance dose for up to 6 months.
Concerns – There have recently been health risks sighted with long-term and continuous use of PPIs (over 1-2 years). Ideally, PPIs should not be continuously used beyond 6 months, to which point no health concerns have been seen in studies. However, if taking continuously beyond 8 weeks, it would be prudent to test regularly for kidney function parameters, magnesium, calcium, and B12 deficiency, and screen for Osteoporosis and bowel infections.
H2 Antihistamines
These medicines prevent the histamine-mediated stimulation of acid production in the stomach. They are taken once or twice a day and are ideal for tiding over short symptomatic periods of acidity due to irregular meals, gastritis, and stress. Commonly used ones are ranitidine, cimetidine and famotidine. They may also be added at bedtime in patients taking PPIs, to give effective basal acid suppression through the night or enhance healing of ulcers.
Concerns – Though no long-term health risks have been reported with H2 Antihistamines, recently many brands of ranitidine were detected to contain amounts of NDMA, a substance known to cause cancer in animals and a probable human carcinogen. NDMA is also found in similar or higher amounts in the environment, industrial waste, and food items like meat, fish, beer, and tobacco smoke. This chemical has been recently found in higher levels in another drug called valsartan (for high BP). Due to this, many manufacturing companies have spontaneously recalled their ranitidine brands, and the USFDA has asked all manufacturers to withdraw all brands of ranitidine from the market. NDMA maximum limit set was 96ng/day (or 0.32 ppm). Most other countries have not yet put out any recommendations or restrictions on doctors or patients for prescribing or taking ranitidine, but have suggested considering other acid suppressant drug options available.
Anticholinergic medicines
These act against acetylcholine-mediated acid stimulation (propantheline, oxyphenonium, and pirenzepine). They are not used much in acidity, GERD, and ulcer management anymore, as they cause disturbing side effects like dry mouth, visual disturbances, constipation, and urinary retention. These drugs may be used when there are associated abdominal cramps (spasmodic pain).
Other medicines for Acidity
Acid neutralizers containing alkaline bicarbonate and hydroxide salts are available as liquid or chewable preparations over the counter. They provide some temporary and short-term relief.
Medicines like sodium alginate that coat and protect the esophagus and stomach lining are also available and may be co-prescribed with acid suppressants and acid-neutralizing agents. Hyaluronic Acid (HA) and chondroitin sulphate (CS) help in mucosal healing and are available as formulations either combined with a coating bioadhesive polymer or with an acid-neutralizing agent like aluminium hydroxide.
Medicines that increase gastric mucus and prostaglandin synthesis (sucralfate, CBS, and misoprostol) are now infrequently prescribed due to multiple dosing and unpleasant side effects.
If symptoms suggest decreased gastric motility like bloating, fullness or nausea, agents called prokinetics are added to the treatment that act by increasing the motility of the stomach as well as increasing the tone of the LES. These include medicines like domperidone, itopride, acotiamide, and levosulpiride.
Digestive enzyme supplements like diastase and pepsin, or pancreatic enzymes, may also be given.
If psychological cause or stress is a likely cause of acidity, appropriate antianxiety-antidepressant medicines may also be added to the treatment regimen under adequate medical monitoring.
Antibiotics (amoxicillin, clarithromycin, or metronidazole) may be added to the PPI for the initial week in case a Helicobacter pylori infection is to be treated. High antibiotic resistance is a problem in treating H. pylori. Alternate or add-on treatment with probiotics (like the gut bacterial strain L. reuteri that also co-aggregates H pylori and reduces its level in stomach) are now becoming available.
Further reading-
Vomiting and Nausea – Understanding Causes, Alert Signs and Health Measures
For any query, additional information or to discuss any case, write to info@drvarsha.com, and be assured of a response soon.
References
Mayo clinic proceedings 2018: Long term PPI health risks
USFDA April 2020 : Ranitidine-NDMA status