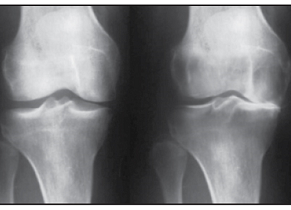
Arthritis is the inflammation of the joints.
Quick read: Arthritis Dietary Tips
Important read: Holistic Health Solutions for Arthritis
UNDERSTANDING THE JOINT AND ASSOCIATED TERMS
Joint
A ‘joint’ in our body is the place where 2 or more bones meet. In some joints, there is a large amount of movement (freely movable joints) like the hip, knee, elbow, shoulder, wrist, ankle, neck, and lower jaw. While at other joints the movement may be minimal or slight like the joints between the vertebrae (bones of our spine- also called the backbone or vertebral column) or no movement at all (between bones of the skull).
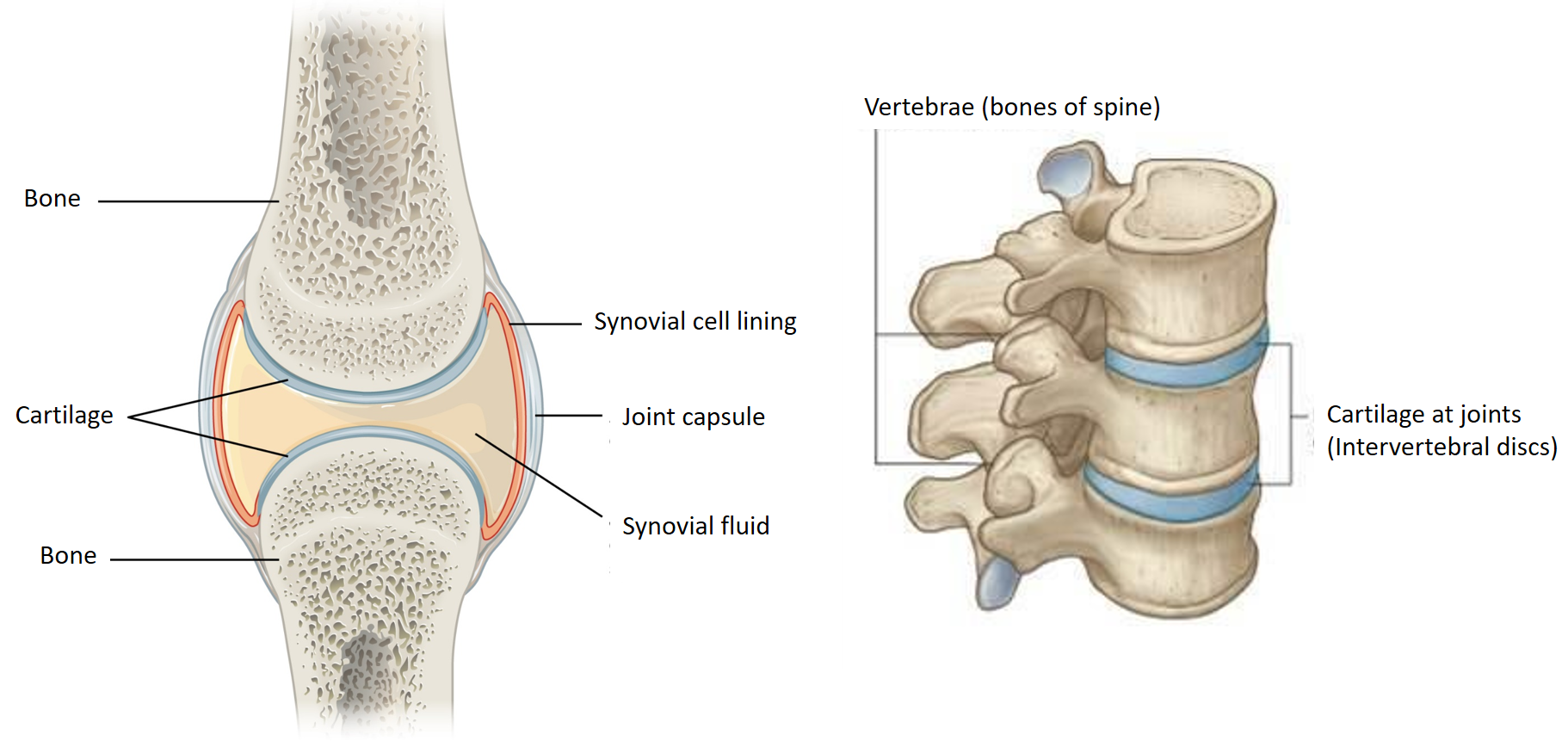
Cartilage
To protect the bones from directly rubbing against each other (which can cause a lot of wear and tear, and injury), the bone surfaces at movable joints are protected by cushioning padding called cartilage. The cartilage is much softer than bone, has strong but flexible proteins called collagen (type II in cartilage) and a water-based matrix (consisting of substances called proteoglycans). This makes the cartilage act like a shock absorber and bone protector during movement.
Freely movable joints in addition to cartilage also have a lubricating joint fluid called synovial fluid in between the two cartilage surfaces, to further reduce friction during movement. That is why freely movable joints are also called synovial joints. The bone ends, with the cartilage padding, and the lubricating fluid is enclosed in a protective synovial capsule.
In the synovial fluid, there are some cells (called ‘phagocytes’) that are capable of ‘eating up’ and clearing the debris and pieces of cartilage resulting from constant joint wear and tear. The body has the ability to synthesize and regenerate cartilage to cope with the loss during this wear and tear at the joints.
The joints between the vertebrae allow scope for small amounts of movement, so there is cartilage in between the vertebrae also called ‘intervertebral discs’.
Joint related terminologies
The word ‘arth’ is related to joints and the word ‘itis’ means inflammation.
Inflammation is the body’s response to injury. The injuring agent can be germs (bacteria, viruses, fungi, or parasites), irritants, toxins, debris, deposits, foreign bodies, direct trauma, some drugs, chemicals, or food items, and sometimes our body’s own immune system (auto-immune reaction).
The inflammatory response consists of increased blood supply to the affected body part (causing redness), leakage of blood with proteins and white blood cells into the affected site (causing swelling), and release of ‘inflammatory mediators’ (causing pain and rise in temperature). This leads to both symptoms of discomfort as well as temporary reduction/loss in the function of the affected joint.
Therefore, arthritis is an umbrella term for all conditions where there is joint inflammation.
Adding the suffix ‘osis’ refers to degeneration (deterioration with aging/ongoing wear and tear). So arthrosis refers to degeneration of the joints, which can progress to inflammation of the joints (arthritis – plural arthritides). The word ‘pathy’ means any disease, So arthropathy is the term for any joint disease (including arthrosis, and arthritis).
The term ‘spondylo’ refers to conditions affecting bones (called vertebrae) and joints of our spine (backbone). So the terms spondyloarthropathy, spondyloarthrosis (also called spondylosis), and spondyloarthritis (also called spondylitis) would imply diseases, degeneration, and inflammation respectively, of the vertebrae and the intervertebral discs of the backbone. Spondylitis can be cervical or lumbar depending on whether it is the upper or lower spine involved, the movement being more in the upper and lower spine, and least in the mid (thoracic) spine.
The term ‘osteo’ is related to bone. Therefore, osteoarthrosis or osteoarthritis specifically implies that there is degeneration and inflammation respectively, involving the bones of the joint.
The term ‘rheumatic’ refers to those conditions causing inflammation of the connecting or supporting structures of the body which can include the joints, bones, muscles, tendons (muscle-bone connectors), ligaments (bone-bone connectors), and sometimes certain other body organs also.


Arthritis (joint inflammation) can occur directly as a result of some insult/injury to the joints, or it can happen indirectly as a result of arthrosis (degeneration of the joints). The latter is commonly seen with age.
OSTEOARTHRITIS
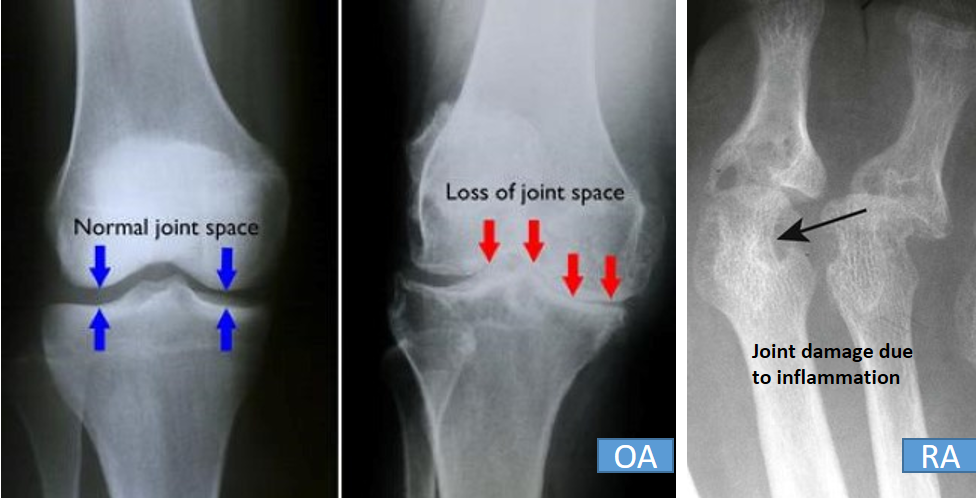
Arthritis due to age-related degeneration is called osteoarthritis where degeneration is the primary pathology and inflammation is secondary (as a consequence) to this. As one ages, joint wear and tear increases, while the effective production and regeneration of cartilage by the body decreases. This leads to a gradual loss of cartilage at the joint. The bone surfaces then start to rub against each other. On an X-ray, the bone ends look irregular and frayed, and sometimes show abnormal outgrowths called spurs.
With age, the amount of lubricating synovial fluid produced also decreases, leading to more friction and injury on movement, as well as decreased clearing of cartilage debris.
These degenerative effects are mainly and prominently seen in joints where there is maximum movement with weight-bearing like the hip and knee.
Signs and Symptoms
Degenerative changes of the joint cartilage, fluid and bone ends constitute osteoarthrosis. Usually, this is diagnosed only on a routine X-ray and the patient is asymptomatic at this stage.
However, going further, the continuing loss of cartilage, bone injury due to rubbing, as well as debris lying in the joint space, trigger inflammation. At this stage, the patient presents with pain, stiffness, reduction or limitation of mobility, and sometimes swelling of the joints. This is called osteoarthritis (OA). The pain and stiffness are maximum on waking up (called morning stiffness) and lessen within half an hour or so.
Risk factors for developing Osteoarthritis
Why some people get osteoarthritis and some others do not, is related to individual factors apart from increasing age alone (usually>50 years). Weight-bearing on the hip and knee joints has been seen to be more in women and in obese/overweight people thereby increasing their risk of developing osteoarthritis. A genetic predisposition plays a role in the physiology of cartilage and synovial fluid production.
Also, individual physical activity can affect the amount of wear and tear. More regular and trained activities like regular exercise lead to muscle-building. Effective muscle action keeps joints taught and reduces wear and tear. It also increases cartilage and synovial fluid synthesis by the body, thus reducing OA risk. Repeated injuries or trauma to joints increases the risk of developing OA later in life.
Chondromalacia patella, also known as runner’s knee occurs when the cartilage on the underside of the kneecap breaks down and softens, causing the kneecap to rub against the thigh bone. This leads to pain in the front or side of the knee that increases after sitting for a long time, or physical activity, using stairs, or getting up from a chair. This may be accompanied by swelling and tenderness of the knee. It occurs more in women and sports people, due to overuse/misuse and injury of the knee cap, weak or tight muscles of the knee, or misalignment of the patella itself.
Osteoarthritis is a major cause of disability in older adults. Around 10% and 18.0% of men and women respectively above 60 years (Around 25% in India) have symptomatic arthritis and almost >50% show X-ray evidence.
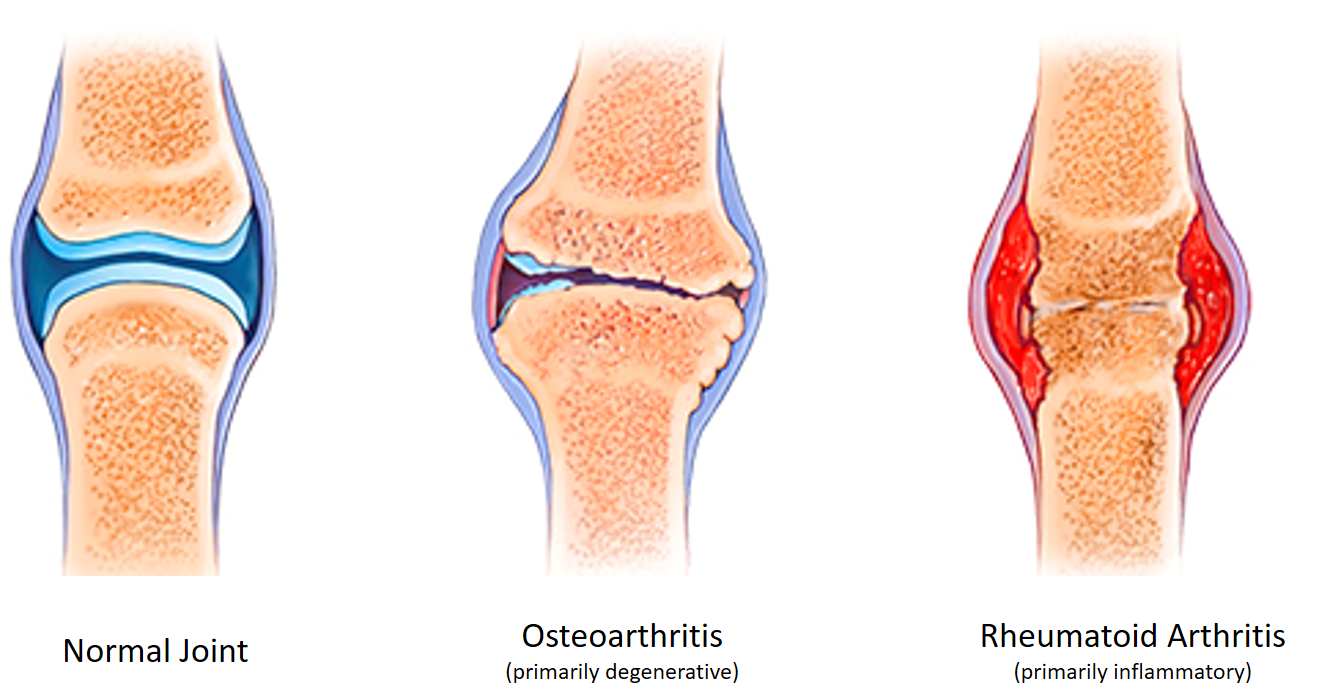


INFLAMMATORY ARTHRITIS
In such cases, inflammation is the primary event in response to some injurious agents attacking the joint. This may be acute (quick onset and short term) like seen with infections of the joint (septic arthritis) or trauma. Sometimes arthritis can even be in response to an infection in another part of the body (reactive arthritis) like infections of the urinary tract, intestine, genitals, or sometimes eye and skin.
Arthritis may be ongoing or chronic, lasting for several years with periodic flare-ups as seen in conditions where there is an agent causing continuous injury. This is seen in autoimmune and other metabolic conditions.
Rheumatoid Arthritis (RA)
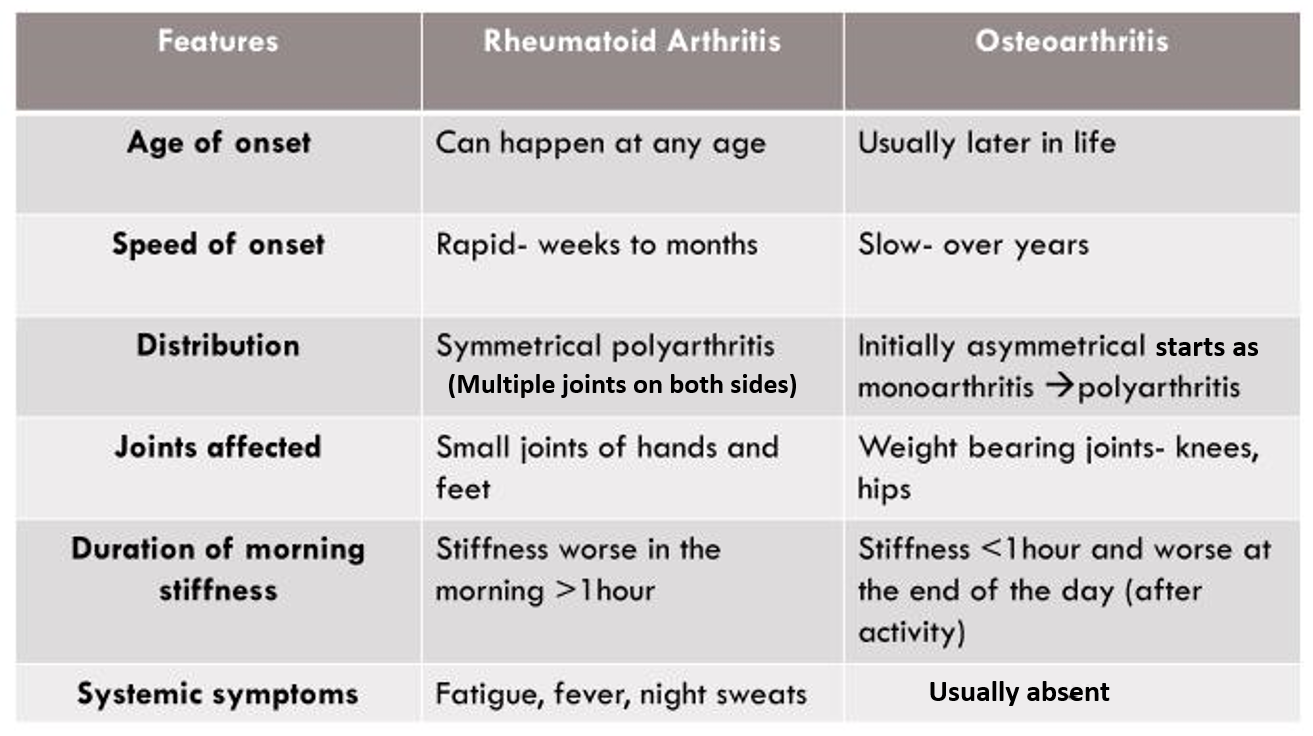
This is a condition in which the body’s own immune system attacks the joint cartilage due to a ‘self versus foreign’ recognition error (autoimmune disorder). This leads to inflammation and damage to the cartilage causing the symptoms of arthritis. In contrast to osteoarthritis (OA), RA is much more rapid in onset, comes at a younger age, and involves the smaller joints (like fingers, wrist, elbow, ankles, and toes) often simultaneously on both sides. RA is symptomatically more severe compared to OA with a much longer duration of morning stiffness (a few hours), severe joint pain and swelling with frequent flare-ups, and worsening over time. Sometimes RA may be associated with fever, night sweats, weight loss, and fatigue.




Other Autoimmune Arthritis
Arthritis can also be a part of autoimmune reactions of other body organs like skin-psoriasis (psoriatic arthritis), dry eye syndromes, uveitis of the eye, Inflammatory Bowel Diseases (IBD), reactive arthritis (post-infection), diseases of salivary glands, lungs, heart, blood vessels, or kidneys.
Gout and Pseudogout
Gout and Pseudogout are conditions caused by the deposition of crystals of uric acid and calcium pyrophosphate respectively, in the joint space that trigger the inflammation. These crystals are formed due to abnormalities in their metabolism or excretion by the kidneys.
SPONDYLITIS – SPINE ARTHRITIS
Aging, accentuated in today’s lifestyle by improper posture, occupational strain, and extensive gadget usage can lead to degenerative changes in the bones and joints of the cervical or lumbar backbone causing spondylosis (spondyloarthrosis). This can similarly progress to inflammation, just as it happens in OA, and is then called spondylitis (spondyloarthritis) causing frequent neck or back pain.
Autoimmune arthritis has also been seen in the backbone which leads to damage and inflammation of the intervertebral discs and adjoining vertebra. This makes the spine appear fused like a ‘bamboo’ on X-ray, a condition called ankylosing spondylitis which causes a stiff and painful back. Sometimes this may be associated with similar arthritis of other joints as well.
Read further – Health Solutions for Arthritis (Medicines, Herbs, Foods, Lifestyle and Surgical options).
Arthritis – Holistic Health Solutions, Medicines and Therapies
Weak, Thinning Bones: Osteoporosis Risks and How to get Screened
Autoimmune Diseases: 15 Well-Known Types and Medical Management
For any query, additional information or to discuss any case, write to info@drvarsha.com, and be assured of a response soon.
REFERENCES