The two most common times when a calcium supplement is prescribed are during pregnancy and later in life for weak bones. Calcium, the crucial mineral for bone often needs to be supplemented after 45-50 years of age, especially in post-menopausal women, to help cope with or prevent bone thinning and osteoporosis. The market is flooded with calcium supplements, so it is important to be aware of what parameters to look for in the calcium supplement you are taking.
THE ACTUAL AMOUNT OF CALCIUM IN THE SUPPLEMENT -ELEMENTAL CALCIUM
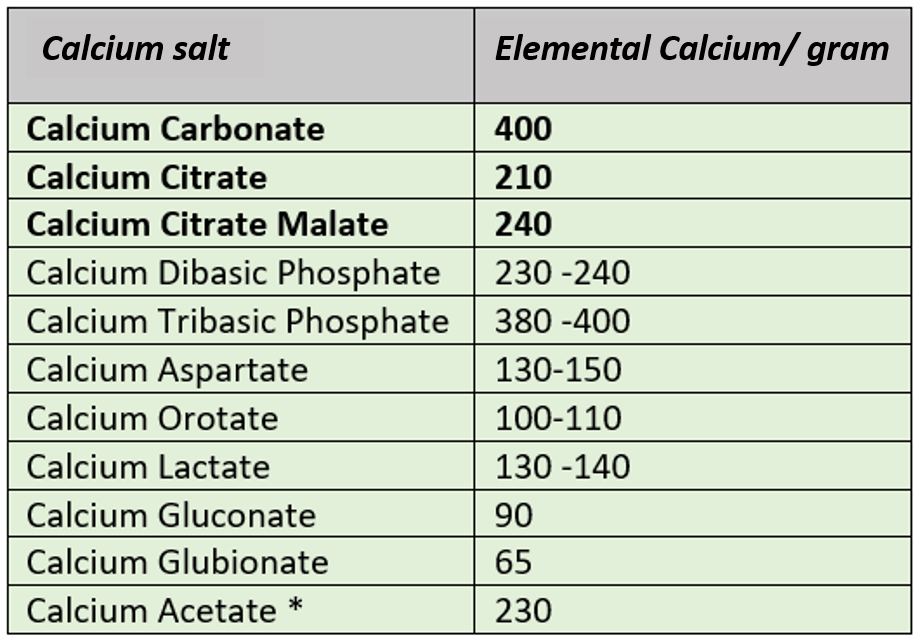
The required daily amount of calcium in adults is around 800-1000 mg daily. Calcium occurs in nature and in supplements in the form of its ‘combination salts’. So, it is important to look at the amount of ‘elemental’ calcium mentioned on the pack and not the amount of the calcium salt. For example, if three packs mention 500mg of calcium carbonate, 500mg of elemental calcium, and 500mg of calcium citrate, the amount of actual calcium in the 3 packs will be 200mg, 500mg, and 105 mg respectively! The table below shows how much actual (elemental) calcium is contained in 1 gram of the various calcium salts used in supplements.
If you have been diagnosed with osteoporosis, you will need to take at least 1000mg/day of calcium. If your supplement gives you only 250mg of elemental calcium or less, you will need 4 tablets/day, compared to a supplement that has at least 500mg of elemental calcium so can be taken twice daily.


DOES THE TYPE OF CALCIUM SALT IN THE SUPPLEMENT MATTER?
Calcium carbonate has the maximum amount of calcium per gram as compared to all other calcium salts, so it works out to be the least expensive for making supplements. It is the most studied and used form of calcium so is the most commonly prescribed too.
Most calcium salts have the drawback that they need stomach acid to release the calcium which is then taken up into the blood from the intestine. So generally, calcium supplements should be taken with meals. The calcium supplements may not work that well if you are taking acid-lowering drugs (like antacids or other medicines for acidity) and in very elderly people who have low stomach acid.
Sometimes gas, belching, and constipation may occur with calcium supplements.
Calcium citrate and calcium citrate malate (CCM) have the advantage here, as they can be taken anytime irrespective of meals, and are suitable even for people taking anti-acidity medicines. These are also less constipating and gas-producing than calcium carbonate.
So if you want to take your calcium anytime irrespective of meals, or you are on and off taking medicines to lower acidity or have a tendency to have gas or be constipated, calcium citrate or calcium citrate malate (CCM) is the supplement for you (but do check if it is offering you enough of elemental calcium that you need daily).
If you do not have acidity or constipation issues, or any need for anti-acidity medicines, you can take calcium carbonate with meals as an effective and most economical option.
Most calcium salts are taken up (absorbed) from our gut (intestine) to the tune of about 30-40%. This can be further stepped up by 20-30% by adding vitamin D. Calcium absorption is very well regulated by our body hormones based on the body’s need and blood calcium levels.
Some of the other calcium salts which have lower amounts of actual calcium to offer, like aspartate and orotate claim very high absorption (85-95%) from the gut to compensate for the lower amount of calcium in them and higher price. However, proper scientific substantiation is lacking for the same. Similarly, some sources of calcium carbonate like corals and algae claim to have much higher absorption as well as extended health benefits, which again needs more scientific data for a clinical recommendation.
*Calcium acetate is not used as a calcium supplement as it ends up binding phosphate (phosphorus), another important mineral for bone, and making it unavailable. So, this calcium salt is reserved for the treatment of some kidney failure patients, where phosphate levels rise dangerously high.
Some foods like spinach, collard greens, sweet potatoes, rhubarb, beans, wheat bran, seeds, nuts, and soy products may contain phytic or oxalic acid which prevents calcium absorption from the gut, and so should not be eaten at the same time with supplements. Chronic industrial/occupational exposure to metals like aluminum, cadmium, lead or mercury, can interfere with calcium absorption
WHAT ARE THE OTHER IMPORTANT INGREDIENTS IN CALCIUM SUPPLEMENTS?
Vitamin D (also known as vitamin D3, or cholecalciferol) is a must in your calcium supplement as it increases the uptake of calcium from your gut as well as helps to push calcium into the bones. Most supplements have between 125-800 IU of vitamin D in accordance with the daily 400-800 IU requirement by our body.
However, if the doctor feels you are significantly deficient in vitamin D, you may be additionally treated with large doses of vitamin D as an injection (1 lakh IU), liquid shots/sachets (60,000 IU) at regular intervals (weekly for a few weeks, followed by monthly for a few months) in addition to what you are taking as part of the daily calcium supplement.
Vitamin D to exert its actions in the body is converted to its active form called calcitriol in a 2 step process taking place in our liver and kidney respectively. Some of the supplements may give calcitriol (usually 0.25 micrograms) instead of vitamin D, which may be useful in the elderly with very low bone density and high fracture risk, especially in those with compromised kidney function who cannot convert vitamin D to its active form.
DO CALCIUM SUPPLEMENTS POSE ANY RISK TO THE HEART?
Calcium can get deposited in blood vessels as plaques. Plaques are usually made by the deposition of fats (cholesterol), calcium, and clots. These can grow over a period of time as deposition increases and can cause blockage of the blood vessels leading to a risk of heart problems like angina or heart attack (myocardial infarction -MI).
As alarming as this may sound, calcium supplements if given with vitamin D have not shown a risk of forming plaques, as vitamin D pushes the calcium to deposit into bone rather than deposit elsewhere. However, the doctor may take extra caution while giving calcium-vitamin D supplements to patients with known heart disease, high BP or cholesterol, obesity, smoking, diabetes, family history of heart attack, or even in the elderly >60-65 years of age.
Vitamin K2 or MK7: Some calcium supplements available have in them a substance known as vitamin MK7 (also called menaquinone or vitamin K2 – usually added in a dose of 25-50mg). This vitamin plays two independent roles in preventing calcium from depositing in the blood vessels and also helping in improving bone density. Calcium supplements containing calcium with vitamin D (or calcitriol ) along with vitamin K2 are preferable supplements in elderly patients, those with osteoporosis and high fracture risk, and existing cardiovascular disease or its risk factors.
ARE THERE ANY OTHER RISKS ASSOCIATED WITH CALCIUM SUPPLEMENTS?
Calcium supplements can increase the risk of kidney stones. For patients having a history of or existing stones and who have to take a calcium supplement, calcium citrate is the best choice.
Iron and calcium supplements should not be taken at the same time as there will be interference in the uptake of iron from the gut. Calcium can also interfere with the uptake of certain BP and heart medicines, antibiotics, oral steroids, and other medicines for osteoporosis so its best to inform your doctor about any kind of medicines you are taking, at the time of being prescribed a calcium supplement.
OTHER INGREDIENTS IN CALCIUM-VITAMIN D SUPPLEMENTS: NOT A MUST BUT CAN BE USEFUL
Sometimes your calcium supplements may have other added vitamins and minerals. How much value any of these actually add to the calcium-vitamin D3 action on bone, can’t be really said with certainty.
Magnesium is known to improve calcium absorption from the gut, help in activating vitamin D, and prevent loss of calcium from bones. Magnesium is usually adequately available through diet, but sometimes during pregnancy and in the elderly, it can be deficient. However, if large doses of magnesium (especially >250mg) are taken along with calcium, then it can reduce the amount of calcium absorbed. So, supplements that have added magnesium usually keep the dose to around 50-100mg.
Zinc has also been linked to the strengthening of bones, so some supplements have added 4-10 mg of zinc which is in the recommended daily dosage range.
Vitamin C is known to improve calcium absorption and also helps in building a substance called ‘collagen’ present in skin, bones, and tendons, so some calcium supplements may have added vitamin C in a dose of 40mg. A similar function has seen to be performed by a substance called lysine (which is an amino acid – the building block of proteins).
Phosphorus is another important mineral for bone along with calcium but is usually well available through diet and also well absorbed, so rarely put in supplements if at all in a dose of 100-200mg.
B group vitamins – Vitamin B6 (also called pyridoxine), B12 (as mecobalamin/methylcobalamin or cyanocobalamin) and folic acid may be added to calcium supplements which are positioned for pregnant women as these vitamins are known to have maternal and fetal benefits.
———————————————————————————————
Further reading –
Weak, Thinning Bones: Osteoporosis Risks and How to get Screened
Understanding the Parathyroid Hormone, Calcium Regulation and Associated Conditions
Arthritis – Holistic Health Solutions, Medicines and Therapies
For any query, additional information or to discuss any case, write to info@drvarsha.com, and be assured of a response soon.
References
Clinical Interventions in Aging 2018:13 2443–2452
JAMA. 2018;319(15):1630
Ann Intern Med. doi:10.7326/M16-2193
Journal of Bone and Mineral Research, Vol. 33, No. 5, May 2018, pp 803–811
BioMed Research International Volume 2018, Article ID 4629383, 8 pages
Mayo Clinic and NIH.gov