Water and food borne diseases and conditions due to contamination include diarrhea (gastroenteritis, food poisoning), dysentery, typhoid, hepatitis, and leptospirosis. Knowing the symptoms, and simple household protective measures can go a long way in controlling and preventing these water-borne diseases
Which are the common water and food borne diseases?
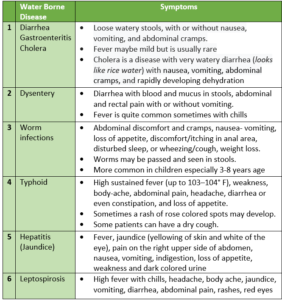


DIARRHEA AND DYSENTERY
These are caused when water or food contaminated with bacteria, viruses, or parasites is consumed, or when food contaminated or prepared with such water is eaten. That is why sometimes the word food poisoning is used. ‘Gastro-enter-itis’ means inflammation (itis) due to injury to the stomach (gastro) and intestine (enteral) lining which causes the symptoms. Flies (houseflies) are often responsible for transmitting such diseases as they sit on dirty areas/garbage (where germs flourish) and then sit on open food, thus contaminating it.
Diarrhea
It can be caused by bacteria (the commonest bacterium is E coli – also called traveler’s diarrhea due to roadside eating/drinking). Cholera, caused by the Vibrio cholerae bacteria, is also often found in contaminated water and food.
Diarrhea can also be caused by the parasite Giardia (Giardiasis) that lasts for 2-4 weeks or longer with a bad taste in the mouth, foul-smelling greasy stools, belching, gas, and weight loss. Therefore Giardiasis should be suspected if any diarrhea lasts more than one week.
In children under 5 years, a virus called Rotavirus can cause profuse watery diarrhea, fever, vomiting, and abdominal pain, for which a vaccine is now available and given by 6 months of age to all children.
Dysentery
This refers to diarrhea with blood and mucus in stools. It can be caused by a parasite (Entamoeba) or by bacteria (the commonest bacteria is Shigella).
Amoebic dysentery (amoebiasis) presents with around 6-8 motions/day with each motion having large amounts of foul-smelling, semi-formed stools that do not stick to the sides of the commode and contain dark red blood.
Bacterial dysentery presents with >10 motions a day with each motion having small amounts of odorless, watery stools that stick to the sides of the commode and contain bright red blood.
TREATMENT
Preventing dehydration is the most important treatment for diarrhea and dysentery. Oral Rehydration Solution (ORS) is available in all chemists and these should be regularly taken mixing in clean boiled 1-liter water. Similar solutions can be prepared at home with half teaspoon salt and 6 teaspoons sugar in 1 liter clean boiled water. Hospitalization for giving intravenous fluids and antibiotics should be done if the patient is unable to take fluids orally and has developed signs of dehydration.



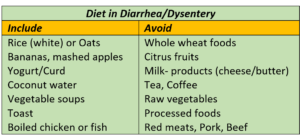
Diet should be nutritious and soothing to the gut. Given below is a guide to an appropriate diet when having diarrhea or dysentery.


Doctors may sometimes order a stool test to identify causative parasites or bacteria.
In severe cases or when required, a combination of antibiotic-antiparasitic medicines are prescribed.
INTESTINAL WORMS
Intestinal worms (helminths) live inside the intestine and feed off the human body. Intestinal worms may be of the following types:
- Tapeworm (from undercooked pork or beef)
- Hookworm (enter through contaminated soil via the feet)
- Fluke (by eating or drinking freshwater plants infected with fluke eggs – adult worms enter the body, and settle in the bile ducts and liver.)
- Pinworm or Threadworm (spread through direct skin contact or by sharing an infected object – female worms crawl out of the anus at night and lay eggs, causing severe itching around the anus).
- Round Worm or Ascariasis (acquired from contaminated food and water).
Symptoms
These include abdominal pain, loss of appetite, indigestion, nausea and vomiting, gas or bloating, weakness, and sometimes weight loss. Sometimes there may be no specific symptoms. Passing pieces of worms in the stool has been sometimes reported by those infected.
Occasionally, parts of the worms can get stuck inside the intestines, causing blockages and impacting normal bowel movement.
Management
If symptoms suggestive of possible worms are present, especially in children, a stool test is helpful to detect worms and their type. Appropriate de-worming medication is given by the doctor.
TYPHOID
Typhoid is caused by a bacteria called Salmonella typhi (sometimes related bacteria called S.paratyphi may cause a similar illness).
Symptoms
Symptoms include a fever showing increasing temperatures each day sometimes with chills, headache, body ache, fatigue, loss of appetite, indigestion with constipation or diarrhea or in some cases abdominal pain, liver inflammation (mild hepatitis), and vomiting, sometimes a cough, and skin rashes.
In some cases, the symptoms of typhoid can be quite similar to viral flu or some of the mosquito-borne fevers (like malaria and dengue).
Management
Usually, a blood test (called Widal test) is done, along with blood ‘culture’ (to grow, isolate and confirm the presence of the causative bacteria) is performed. The doctor may simultaneously order blood tests for typhoid, malaria and dengue to confirm the diagnosis. Sometimes additional urine and stool tests may also be performed to confirm typhoid.
Typhoid is usually managed on an outpatient/ home-care basis. Treatment includes appropriate antibiotics, fluids to maintain hydration and supportive medicines for fever and pain.
Diet should be soft and easily digestible like soft rice, with pulses (dal khichdi), cooked vegetables, coconut water, buttermilk, fruit juices, mashed bananas/apples and potatoes.
Hospitalization is needed if the patient is unable to take fluids or medicines orally due to severe vomiting.
Complications
Typhoid recovers well with treatment but rarely, complications can occur, like perforation of the intestine with internal bleeding and spread of infection in the abdomen.
Typhoid may also cause complications by affecting the lungs (pneumonia), heart (myocarditis, endocarditis), urinary bladder (cystitis), pancreas (pancreatitis) and brain-spinal cord (meningitis). The fatality rates are about 1 in 1000.
Prevention
Typhoid Vaccination is available and now part of the childhood immunization schedule. Both injectable and oral vaccines are available.
HEPATITIS
Water-borne Hepatitis is caused by 2 kinds of viruses (Hepatitis A and E virus), while the other forms of Hepatitis (B, C, D) are spread by blood contact and have more serious and long-term consequences. Hepatitis as the name suggests is primarily an infection of the liver. Hepatitis A occurs mostly in children, however, it can affect adults also in whom it can rarely cause complications of liver failure (mortality around 5 in 1000). Hepatitis E mainly affects young adults, but in pregnant women, it can be severe with complications (sometimes fatal 1 in 5).
Symptoms
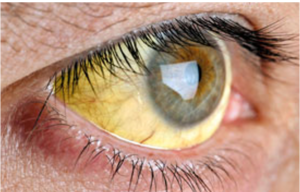


Both Hepatitis A and E present with similar symptoms. These include yellowing of skin or eyes, loss of appetite, indigestion with vomiting, diarrhea and abdominal pain, fever, body and joint pains, fatigue, and altered color of stools.
Management
Diagnosis is made by a blood test to detect the hepatitis virus antibodies and monitored with Liver function tests (blood bilirubin, liver enzymes, and protein levels).
Usually, water-borne Hepatitis resolves on its own with adequate fluid, rest, and appropriate diet (balanced, nutritious diet, low on fats). In fact, no medicines are recommended as they put a load on the liver. Alcohol and smoking should be strictly avoided.
Prevention
Vaccine for Hepatitis A is available, while for Hepatitis E currently it is only developed in China. Sanitization of water, and hygienic food practices remain the cornerstone of prevention.
LEPTOSPIROSIS
The bacteria that cause leptospirosis are spread through the urine of infected animals like rats, pigs, dogs, squirrels, and cattle. Humans can be infected through contact with water or soil containing animal urine. The bacteria can enter the body through a cut or scratch in the skin. Drinking contaminated water can also cause infection. Those people who wade/walk through puddles or accumulated rainwater are especially at risk.
Symptoms
These include high fever with chills, headache, body aches, abdominal pain and vomiting, red eyes, and yellowing of skin.
Management
A specific blood test is available to confirm the diagnosis. Antibiotics, fluids and supportive care for fever are the usual treatment, however, hospitalization is usually recommended as lung or kidney complications can occur, and the fatality rate is about 1 in 20.
LISTERIOSIS
PROTECTION AGAINST WATER AND FOOD BORNE DISEASES
Why is there more water and food contamination during the rains?
Increased contamination of water during rains is because of rain-water falling on garbage dumps, ditches and areas of waste which are rich in infection-causing organisms, and this water flows down as surface ‘runoff’ into our water sources.
When such contaminated water is directly consumed or when food contaminated with such water is eaten, the body can get exposed to these infective organisms (like bacteria, viruses and parasites), leading to what we call the ‘water-borne diseases.’
Prevention is better than cure
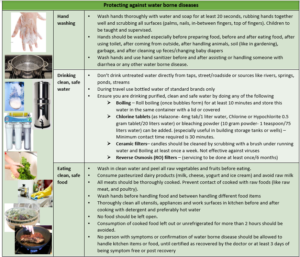



People who wade/walk through puddles or stagnant rainwater without appropriate protective footwear are especially at risk of Leptospirosis. They should wash their legs thoroughly on return.
PRACTICING FOOD SAFETY AND HYGIENE
- avoid raw fish and meat
- thoroughly cook meat to temperatures of at least 145°F (62.8°C) for whole cuts of meat and 160°F (71°C) for ground meat and poultry, till it is steaming hot.
- let cooked meat rest for 3 minutes before carving or consuming
- freeze fish or meat to –4°F (–20°C) for at least 24 hours
- wash, peel, or cook all raw fruits and vegetables
- eat ready-to-eat foods within four hours of taking them out of the fridge
- follow food labels and use opened food within two days
- keep raw and ready-to-eat foods separate
- wash your hands regularly with soap
- wash or reheat any food that falls on soil or unclean floor
References
India Water portal, National Health Portal, Microbeonline
Also read-
Vomiting and Nausea – Understanding Causes, Alert Signs and Health Measures


