DASH- Dietary Approaches to Stop Hypertension is a well-structured diet which helps control conditions like High BP, and high BMI.
High Blood Pressure (BP), is a risk factor for developing Cardiovascular Disease (CVD), which includes conditions like Angina, Heart attack and Stroke, as well as other organ complications.
Lifestyle and diet modifications are the corner-stone of preventing and managing high blood pressure as well as reducing the risk of the various cardiovascular complications associated with high BP. Incorporating lifestyle measures is the initial and first recommended management of high BP and continues life-long even if and after BP lowering medicines are started.
DASH (Dietary Approaches to Stop Hypertension)
This is a diet rich in fruits, vegetables, and low-fat dairy products, with moderate amounts of whole grains, legumes, nuts, fish and poultry, and low amounts of fat and sugar content. This is a scientifically evaluated and studied diet and is now recommended by major health associations.
The DASH diet was designed to reduce blood pressure and cardiovascular risk, but it can be followed by anyone for maintaining good health and fitness.
Up to 5-6mm Hg drop can be achieved in blood pressure with regular incorporation of the DASH diet. This diet aims to supply 2000 Kcalories /day (55-60% from carbohydrates; 25-30% from fats and 15-20% from proteins).
The DASH diet helps to maintain weight (and even lose weight in the range of 1-5 kg or so). If a larger amount of weight loss is required to reach the recommended BMI of <25 kg/m2, a further reduction in calorie intake and a structured weight loss program is recommended. (BMI is Body mass index – calculated by dividing the current weight by square of height. Healthy BMI range is 18.5-24.9 kg/m2)
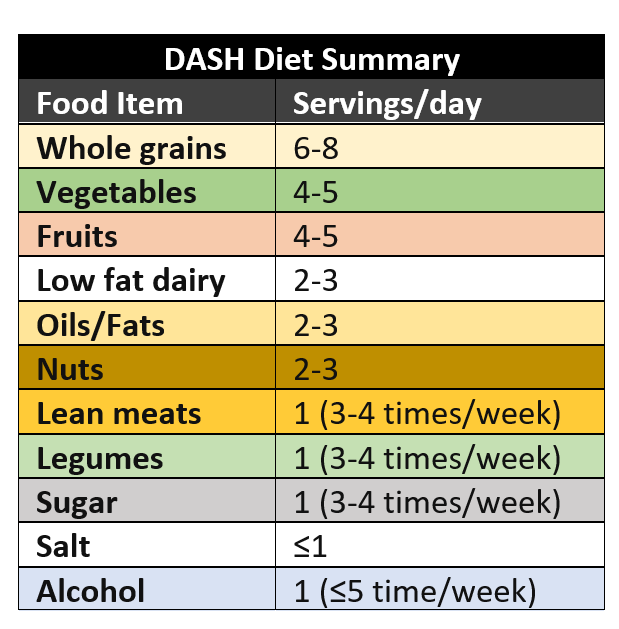
Below is a practical guide to incorporate and achieve the DASH diet.
(Note ‘cup’ refers to any utensil which accommodates around 240-250ml of water; 1 tablespoon =15ml=3 teaspoons).
CEREALS/ GRAINS
- Move to whole-grain cereals that have higher nutrition and fiber, with less fat – like whole-wheat bread/pasta.
- Though brown rice has slightly more calories compared to white rice, it has a higher content of fiber, antioxidants and some B group vitamins, manganese, and magnesium. Therefore in hypertensive patients especially with accompanying diabetes, high cholesterol and/or obesity, brown rice may have health benefits over white rice. Brown rice also helps in reducing constipation.
- 6- 8 servings/day is recommended. 1 serving = 1 bread piece, 1 regular wheat chapati/roti, 30 g (approx 1 cup of dry cereal) or ½ cup for cooked cereal/rice.
- Do not add butter, ghee, oil, cream or sauces.
VEGETABLES
- Include plenty of fresh vegetables in diet –Green vegetables, carrots, tomato, and sweet potatoes, as these offer a range of vitamins and minerals including potassium.
- 4-5 servings/day is recommended. 1 serving = 1 cup raw/leafy green vegetables or ½ cup for cut/cooked vegetables.
- If using canned vegetables go for ‘low salt’ preparations or 1-2 rounds of rinsing.
FRUITS
- Most fruits are low in fat (exceptions like coconut) and high on fiber, vitamins, and minerals like potassium.
- 4-5 servings/day is recommended. 1 serving = 1 full medium-sized fruit, ½ cup of cut fresh, frozen or canned (no added sugar) fruits or 120ml (half cup) fruit juice.
- Fruits can be consumed with meals and as inter-meal snacks.
DAIRY PRODUCTS
- These include milk, yogurt, and cheese which are good sources of protein, Vitamin D and minerals like calcium and potassium.
- For milk 4 options are available: whole milk(3.25% milkfat), reduced-fat milk (2% milkfat), low-fat milk (1% milkfat) and fat-free/skimmed milk (0.1-0.2% milkfat). Choose low fat or fat-free/skimmed options for milk, yogurt, and cheese.
- 2-3 servings recommended per day. 1 serving = 1 cup milk; 1 cup yogurt or 40-50g cheese
- If lactose intolerant- go for lactose-free milk, yogurt or cheese options which are now available
- Cheese should be checked for salt content (should be in the range or less than 300-330mg sodium/g of cheese)
FATS
- Fats are important for the absorption of vitamins A, D, E, and K and the healthy functioning of our cells. But care needs to be taken to have just enough for maintaining good health and not increase the risk of obesity, diabetes and cardiovascular disease.
- Out of the daily recommended intake of 2000 calories, about 30% should come from fats.
- Good fats (include in diet) – mono and polyunsaturated fats (oils like sesame, sunflower, soybean, olive, canola, rice bran, linseed/flaxseed, and peanut oils, fish/fish oils, margarine, and nuts like cashews, almonds, walnuts, peanuts, avocados, and pine nuts)
- Bad fats (avoid in the diet – keep to 5% or less) – saturated fat (found in butter, cheese, coconut and palm oil, lard, cream, whole milk, red meats) and trans fat (processed and fried foods).
- 2-3 servings/day is recommended. 1 serving = 1 teaspoon oil/margarine or, 1-2 tablespoons salad dressing/mayonnaise or ¼ cup nuts.
- Nuts should be eaten in moderation (3-4 times/week)
NON-VEGETARIAN FOOD
- Meats are not only a rich source of protein but also of vital minerals and vitamins.
- While choosing meats, go more with lean meat (low fat) instead of red meats, use poultry with skin/fat removed, consume as grilled/boiled form instead of fried, and substitute fish (salmon, tuna, herring) and shrimp for meats on some days.
- 1 serving/day is recommended. 1 serving = 150-200g for meats/fish/poultry or 1 egg
LEGUMES
- They are good sources of protein for vegetarians and nonvegetarians
- Soybean is a very good option for meat in vegetarians in the same measure.
- 1 serving/day is recommended. 1 serving = ½ cup cooked lentils/peas/beans per day
- Limit peas/beans to not more than 4 times/week.
SWEET (SUGAR)
- Try as much to go for low fat/low sugar options with sweet.
- Artificial sweeteners such as aspartame or sucralose can be substituted but not overused.
- 1 serving/day (not more than 3-4 servings/week) is recommended. 1 serving = 3 teaspoons sugar/jam
- (Diabetics require separate restrictions)
Beverages
- 1-2 cups of tea or coffee are fine in a day (200ml/cup).
- Coffee may affect immediate BP so avoid BP measurement within half to 1 hour of taking coffee. However, a long-term consistent rise in BP or development/worsening of BP has not been seen with coffee taken within limits.
- Make sure the added sugar remains within daily limits of 3 teaspoons of sugar.
SALT
- Aim for reducing daily salt intake to 1.5-2 teaspoon./day On any single day keep maximum use of salt in the range of 3-5g sodium. (salt contains 38-39% sodium).
- Total salt intake should be always kept less than 1 teaspoon per meal (6g salt giving 2.3g sodium) and aim to push it to 1/2 to 2/3 teaspoon per meal over a period of time. This may sound like a tough task for the taste buds but with time and other seasoning options, the adjustment of the taste buds can be achieved.
- Non-salt seasoning and spicing options include – garlic, onion, celery, mustard, cilantro, ginger, lemon, and vinegar
- It is important to explore low salt/low sodium options in foods, as well as read the salt content mentioned on the pack of food items before buying.
- Canned foods and pickles are high in salt. 1-2 rounds of rinsing can help cut the salt down.
- In addition to lowering sodium, the amount of potassium should be stepped up in diet to 3.5-5g/day. This is automatically achieved with high amount of fruits, vegetables, low-fat dairy items and food items like fish part of the DASH diet. Roasted options instead of boiling, yields more potassium.
ALCOHOL
- Drinking in moderation is permitted and may contribute to relaxing the mind, and also raising good cholesterol (HDL) but some do’s and don’ts need to be observed.
- Limit to a 1 serving/day or 5 glasses/week. On a single day do not go beyond 2 glasses.
- Do not gulp drinks, or binge drink, or drink on an empty stomach.
- 1 serving=1 glass.
- Vodka, Whiskey, Brandy, Rum (contain around 40% alcohol). 1 glass=45 ml (If the alcohol content is 50% or more, make it 30ml)
- Wine (contains around 10-20% alcohol). 1 glass =120-140ml depending on alcohol content mentioned on the bottle
- Beer (contains around 5% alcohol). 1 glass=350ml


Also read-
High Blood Pressure (BP) – Risks and Solutions for Hypertension
For any query, additional information or to discuss any case, write to info@drvarsha.com and be assured of a response soon
References
American Heart Association: DASH Diet – Feasible for everyone
Salt and Sodium intake recommendations


