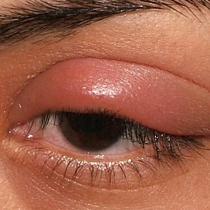
A swollen eyelid (swelling on the eyelid) is common and distressing due to both irritation and cosmetic disturbance. These are mostly innocuous and resolve within a few days to weeks.
STRUCTURE OF THE EYELID
The eyelid is made up of protective eyelashes (hairs) that come out of hair glands (called follicular glands) on the lid margins. Just behind the row of eyelashes, is another row of the openings of oil-producing glands (called meibomian glands). The oil (called sebum) from these glands helps prevent the tears from evaporating or flowing easily.
The eyelids are made up of loose thin skin, lid muscle and fat, but are kept stiff by the tarsal plate and orbital septum (made up of dense and fibrous tissue respectively). The eyelash follicular glands and the meibomian glands are in this tarsal plate. The orbital septum separates the eyelid from underlying structures within the orbit (eyeball socket).
A muscle called levator palpebrae superioris elevates the upper eyelid to open the eye. If the action of this muscle is affected, it can lead to drooping of the eyelid called ptosis.



STYE (HARDOLEUM)
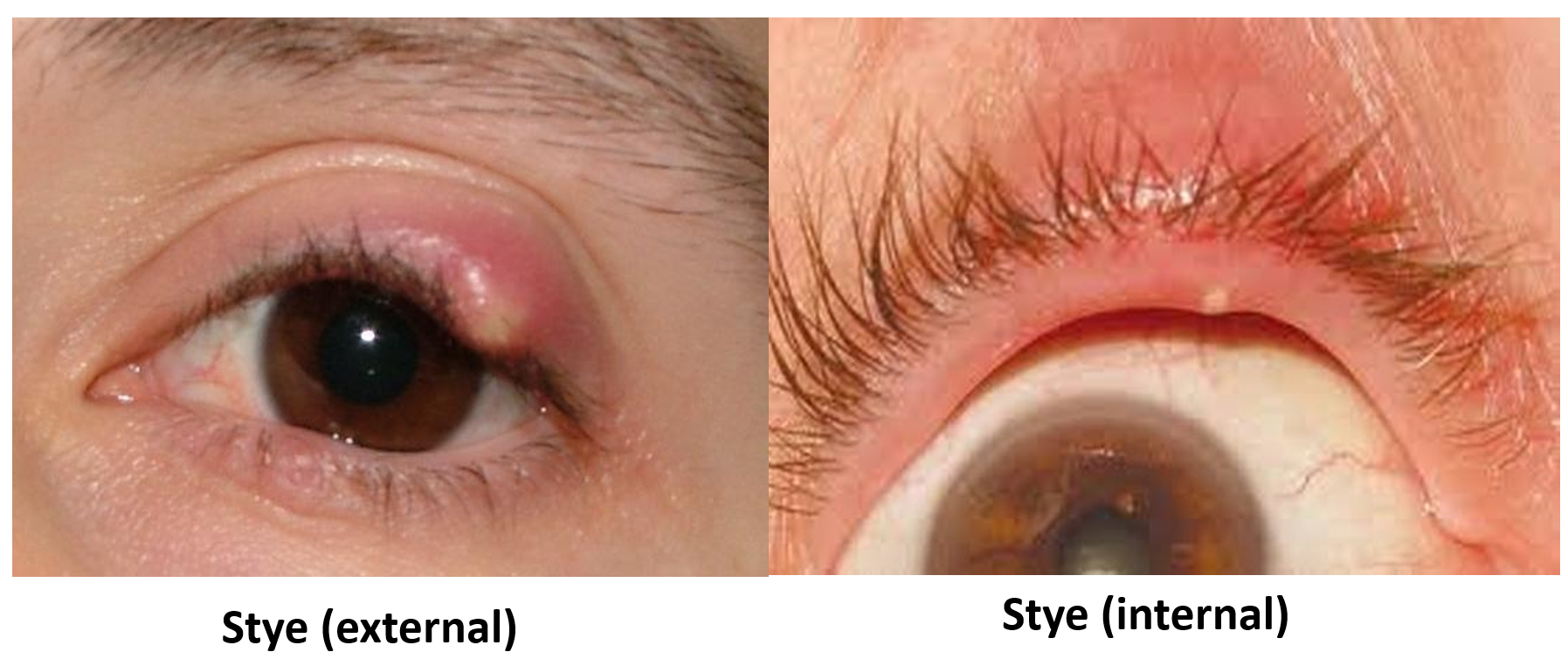
A stye (also called sty) is one of the most common causes of a swollen eyelid. It is a localized bump on the eyelid (upper or lower), caused due to infection and pus formation in one or more glands. It is commonly due to infections of the eyelash follicular gland (external stye), but can also be due to infections of meibomian glands (internal stye). The lid swelling usually appears red, boggy and tender to touch, with the pus point often visible. Staphylococcus is the most common bacteria involved.
Symptoms include redness and pain (especially on touching or moving the lids), with the swollen eyelid causing droopiness, irritation, itching and discomfort while blinking. Other symptoms include increased tearing, and mucus discharge, which can also cause yellow crusting on the lid margin and sticky lids. Internal stye causes more irritation and foreign body sensation in the eye than external stye.
Anyone can get a stye sometime, however recurrent stye can be attributed to some risk factors. These include improper lid cleaning and hygiene, not removing eye makeup before sleeping, using irritant or outdated cosmetics, improper contact lens hygiene, poor sleep, nutritional deficiency, diabetes and hormonal imbalance. It may also occur due to blepharitis (see below).


A stye is treated as follows:
- Warm compress application for 5-10 minutes, 3-4 times a day. This can be done with a clean cloth, gauze or cotton dipped in warm water and applied on the eyelid. It helps to decrease pain and ease out drainage of pus.
- In some cases, medicines for pain and inflammation like ibuprofen, diclofenac or aceclofenac with paracetamol may also be taken for quicker relief.
- Antibiotic eye ointments are usually prescribed to be applied on the eyelid 3-4 times/day. Sometimes eye drops are given if there is eye irritation especially if it is an internal stye. Oral antibiotics are not usually needed.
- If the swelling of an external stye is very painful, and the pus is not draining out, removal of that eyelash and draining the pus out with a needle is helpful. This is to be done only by a qualified eye specialist.
- Avoid using contact lenses, eye makeup and cosmetics in this period. Once the stye resolves, use a fresh pair of contact lenses and replace them in disinfectant contact lens liquid daily. Avoid kajal (kohl) inside the eyes.
Styes should not be squeezed. Most styes resolve completely and cause no long-lasting problems. Injury during drainage can sometimes cause a localized absence of eyelash growth, scarring or lid deformity. Very rarely the infection can spread throughout the lid into the deeper layers, and cause preseptal cellulitis (see below).
CHALAZION
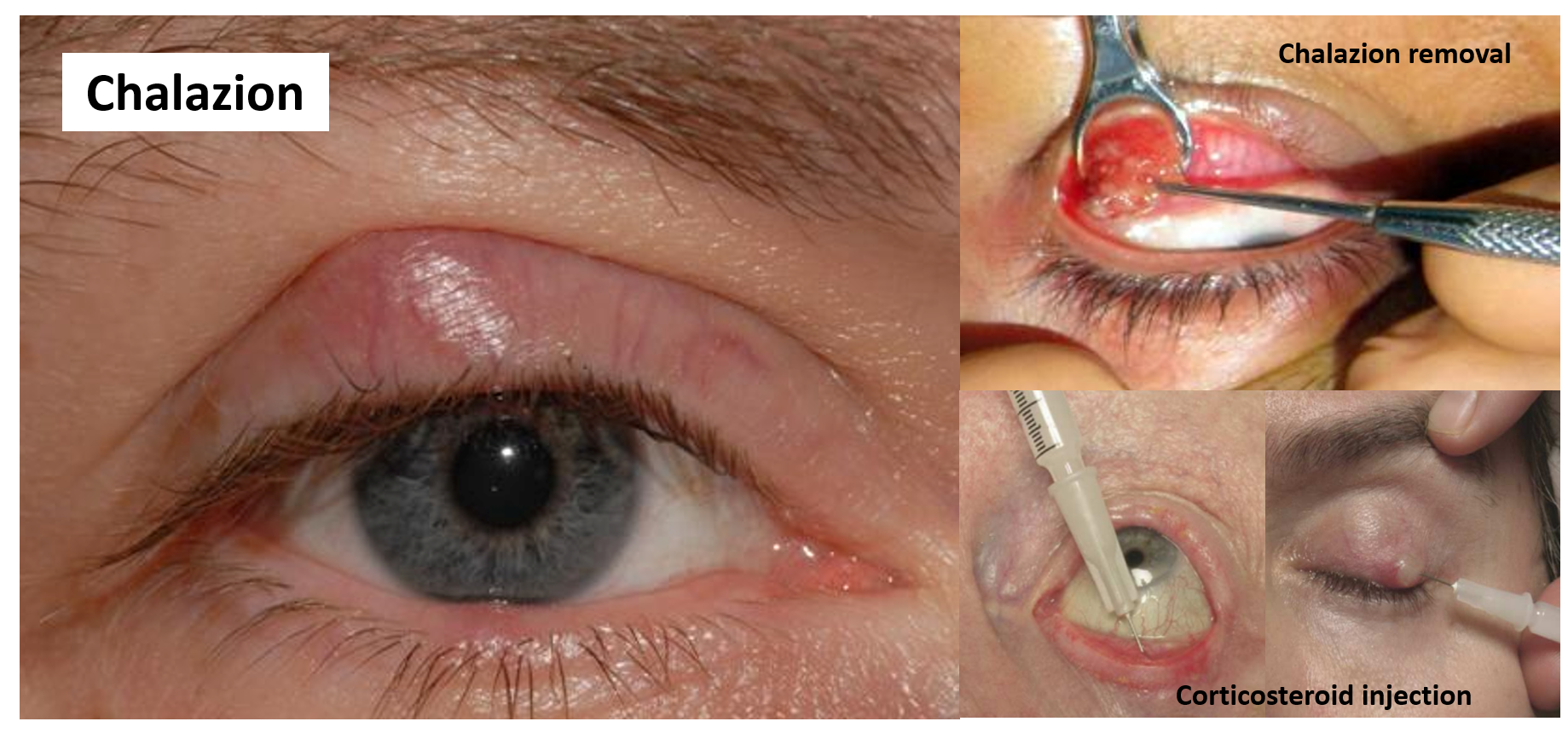
A chalazion is a cyst-like localized swelling that appears like a reddish bump on the eyelid (more commonly the upper one), giving the appearance of a swollen eyelid. It is caused due to the blockage of the opening of the meibomian (oil gland) and the subsequent swelling and inflammation of the gland. A chalazion is non-infectious, usually painless, and hardly produces symptoms except for mild irritation and cosmetic disturbance. A chalazion can result from an internal stye once the infection has resolved, or can occur by itself. A chalazion can also turn into an internal stye if the oil gland gets infected and forms pus.


A chalazion is treated as follows:
- Warm compress helps to ease out the blockage
- Antibiotic ointment may be applied 3-4 times daily. Sometimes a combination ointment of an antibiotic with a corticosteroid is used, to reduce the gland inflammation.
- A chalazion usually resolves in a few weeks. They should not be squeezed.
- A chalazion that does not resolve is either injected with corticosteroid medicine or more commonly removed by a simple outpatient drainage procedure under local anesthesia.
BLEPHARITIS AND MEIBOMITIS
Blepharitis
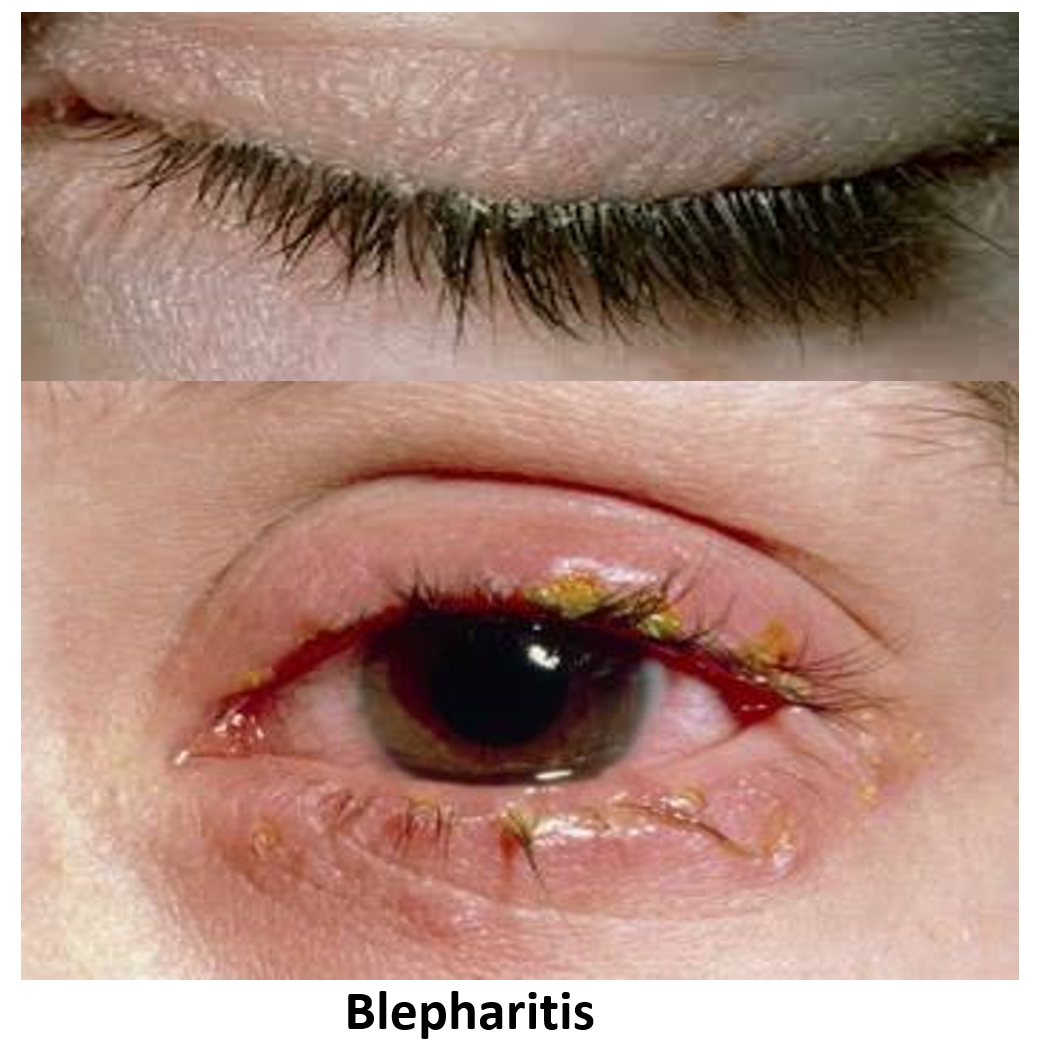
It is a condition resulting from the blockage and inflammation of the eyelash follicular glands. It is usually painless but presents with itching and irritation with a constant desire to rub the eyelids. Typically, flaky or crusted (whitish-yellow) deposits are seen sticking to the base of the eyelashes. The irritation and rubbing can result in a mildly swollen eyelid. There may also be associated watering and a mild redness of the eyes. Blepharitis often affects both eyes together.
The cause of blepharitis is often not known, but some factors implicated include chronic lid infections mainly due to dandruff (seborrhea) or staphylococci bacteria, low lid hygiene, allergy (to cosmetics, lens solutions, or an unknown agent), and dryness of eyes. It is also seen in a condition called rosacea. Demodex blepharitis is an eye condition caused by an overgrowth of microscopic Demodex mites on the eyelashes and eyelids, leading to symptoms like itching, burning, redness, and a “cylindrical dandruff” or collarette at the base of the lashes. It’s a common form of blepharitis, especially in older adults, and can significantly impact daily life.
People with blepharitis are more at risk of developing a stye or chalazion. Blepharitis can also interfere with the normal tear film, causing dry eyes, and increased predisposition to conjunctivitis. People with blepharitis may also experience falling or loss of eyelashes (madarosis). Repeated rubbing and lid trauma can cause scarring and distortion of the lid contour leading to misdirected eyelashes along with tear film inconsistency that can cause injuries (abrasions) of the cornea. Therefore, blepharitis should be treated in time to prevent such consequences.


Meibomitis
Meibomian glands produce oil, which constitutes the outer tear film layer, preventing tears from evaporating. Their opening can get clogged and the glands inflamed (meibomitis), which can lead to generalized lid swelling and inflammation of the lid margin, and can also cause dry eye by reducing lubrication and increasing tear evaporation.
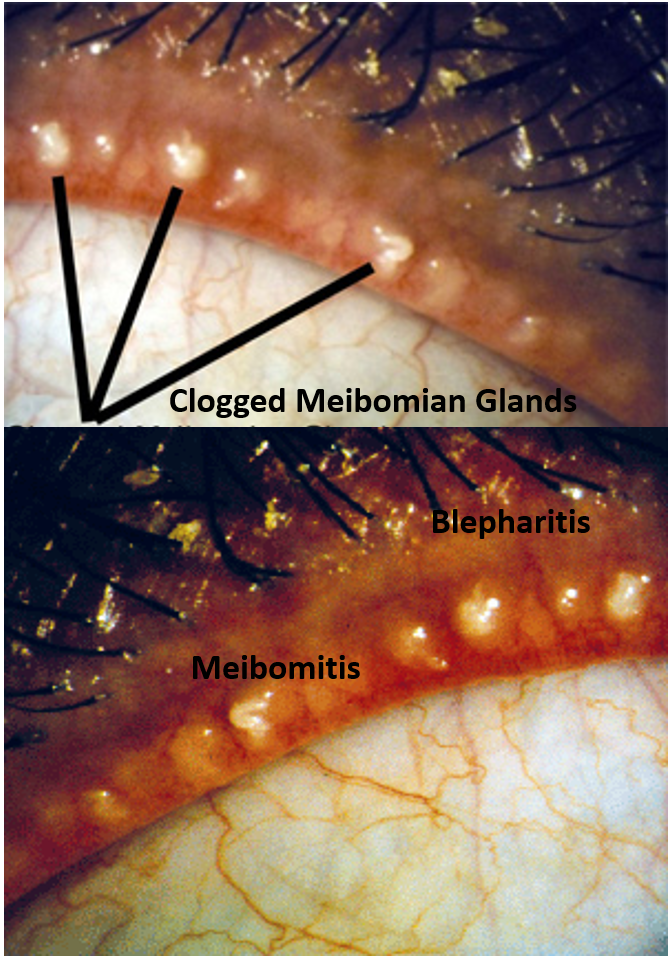


Both blepharitis and meibomitis can coexist.
TREATMENT OF BLEPHARITIS AND MEIBOMITIS:
- Gentle lid scrubs can be done 3-4 times a day. A cue tip or cotton bud is moistened and a few drops of baby shampoo (non-irritant) are added to it. The eyelid should be pulled away from the eye and the base of the eyelashes should be gently scrubbed to remove the flakes and clean the lashes. This also helps to unclog the openings of the eyelash follicular glands. Thereafter the eyelids should be washed well with warm water and patted dry with a clean towel.
- Warm compress 2-3 times daily with gentle lid massage also helps to unclog the gland openings.
- Lubricating eye drops may be recommended.
- Perfluorohexyloctane ophthalmic solution is the first drug specifically for dry eye caused by Meibomian gland dysfunction (MGD). It works by producing oil-like lipids to prevent tear evaporation and stabilize the tear film. It is water-free and preservative-free, applied twice daily.
- Lotilaner ophthalmic solution 0.25%, is the first FDA-approved treatment specifically for Demodex blepharitis.
- Regular hair-washing (3-4 times/week) with antidandruff shampoo should be done. An anti-lice treatment should also be given.
- Avoid eyelid makeup and cosmetic use as much as possible.
- Antibiotic ointments (sometimes in combination with corticosteroids) may be applied after the lid scrubs.
- A course of oral antibiotics sometimes with oral anti-inflammatory medicines like corticosteroids or cyclosporine may be recommended in more severe and non-responsive cases.
Blepharitis has a tendency to recur, and can sometimes be stubborn to treatment. Many natural remedies have been described for blepharitis about which you can check with your doctor. Blepharitis should be treated properly and with appropriate methods that work for the specific person.
Read: Natural remedies for Blepharitis
OTHER CAUSES OF EYELID SWELLING
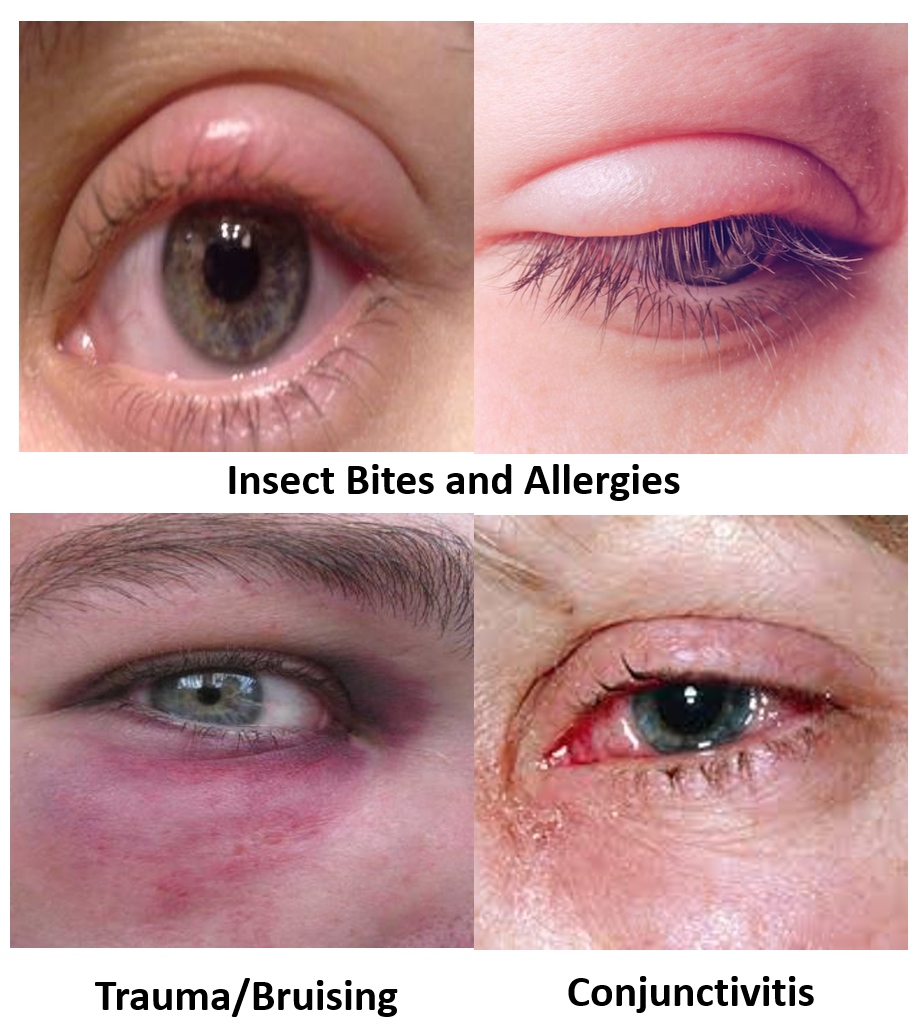
A swollen eyelid can also occur as a result of insect bites/stings (like mosquitoes, bees, wasps, etc). Allergy to pollen, dust, or food ingredients, and reactions to chemicals in cosmetics or medicines (contact dermatitis/eczema) are also common causes. In such cases, the lid swelling is usually painless and boggy with associated itching. It usually resolves on its own, however, if the swelling is large, one or two doses of an oral antihistamine medicine may be given.
Conjunctivitis (viral/bacterial/allergic) can also be associated with a swollen eyelid.
A history of trauma should always be taken as bruises can result in swollen eyelids which soon take on a bluish-purple or blackish color. One should always get a detailed eye examination to rule out external and internal injuries to the eye in such cases.


CELLULITIS
This refers to the spread of infection into the deeper layers of the skin and underlying structures.
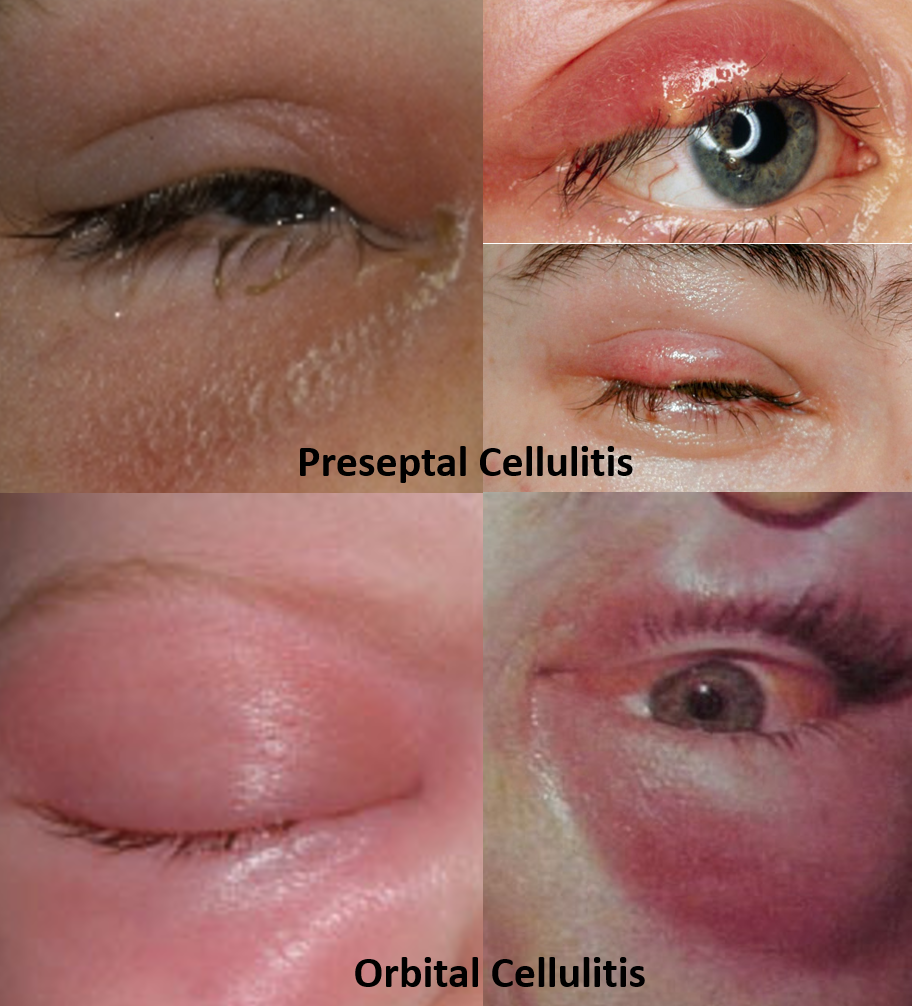
Preseptal (Periorbital) cellulitis
This is seen when the infection spreads throughout the eyelid and part of the face but does not involve the deeper structures in the orbit (does not spread beyond the orbital septum). It can rarely occur as a complication of a stye, insect bite or local trauma.
It presents with red and painful swollen eyelids and some swelling of the adjoining face, difficulty in opening the eyelids and sometimes an associated fever. However, vision or eye movements are not affected.
The patient should be treated promptly with oral antibiotics and pain-relieving anti-inflammatory medicines.
Orbital cellulitis
This occurs when the infection spreads beyond the orbital septum and involves the deeper structures in the orbit like muscles and nerves. This can occur as a complication of sinus infection or trauma.
This also presents with redness and painful swelling of the eyelids and adjoining face, difficulty in opening the eyelids and sometimes with a fever. The differentiating features from preseptal cellulitis is that the swelling is usually massive with blurring or decrease of vision, pain on eye movements, difficulty in eye movements (or loss of eye movement in a particular direction leading to double vision), and forward protrusion of the eyeball (proptosis). The patient requires urgent hospitalization and treatment with intravenous antibiotics. Investigations like a CT scan may also be performed on admission.


Alert Signs for Eyelid Swellings
The following red flag alert signs should prompt urgent medical consultation and intervention:
- Lid swelling involving the entire lid and part of the face.
- History of trauma
- Severe pain on the lids or face
- Inability to open the lids
- Decrease in vision (or blurring which does not clear on blinking, or cleaning the eye)
- Double vision in any direction
- Pain on moving the eyes sideways or up and down
- Inability to move the eyes sideways or up and down
- Severe redness of the eyes or eye pain
- Eyeball looks protruded
- Fever
- Headache, breathlessness or vomiting
Rare Causes of Eyelid Swelling
There are some rare causes of eyelid swelling that should be considered if all the above common causes have been ruled out.
Blepharochalasis or blepharochalasis syndrome usually starts in childhood or adolescence and is characterized by episodic inflammation of the eyelids that causes painless swelling of the upper eyelids (rarely lower also) of both the eyes (rarely one of the eyes). The eyelid swelling attacks are usually 3-4 a year, and last 3-4 days. Thereafter there may be a swelling-free interval of 2-3 years where the eyelids appear loose, baggy and ‘paper thin’.
Melkersson-Rosenthal syndrome (MRS) is a rare disorder characterized by recurring swelling of the face especially the eyelid and upper lip, facial weakness or paralysis, and in a few cases the presence of a central furrow in the tongue. Cases of MRS with a monosymptomatic presentation of one-sided eyelid swelling or face/lip swelling only have been documented. Therefore, MRS should be considered in all cases of isolated painless eyelid swelling. The diagnosis is confirmed by an eyelid incisional biopsy.
Orbital Pseudotumor is a noncancerous inflammatory swelling behind the eye. It usually causes painful swelling of the eyelid, along with protrusion of the eye (proptosis), and sometimes restriction of eye movements causing double vision. It is usually diagnosed by an MRI.
The above conditions may be due to immune-mediated (or autoimmune) mechanisms but the etiology is not established. They are usually diagnosed on high clinical suspicion, ruling out of common conditions, and with the help of an MRI and/or biopsy. The initial treatment is with oral corticosteroid medicines, and other drugs including non-steroidal anti-inflammatory drugs, immunosuppressive drugs, dapsone, antihistamines (antiallergics), antibiotics like doxycycline, and nutritional supplements. Lid surgery (blepharoplasty) may be considered for non-responsive cases of blepharochalasis and MRS, or surgical removal/resection of the pseudotumor.
Tumors of the eyelid, orbit or lacrimal gland can also be rarely responsible for lid swellings. An MRI or biopsy can confirm the same. Surgical resection, radiotherapy and chemotherapy are the treatments depending on the type of tumor.
SYSTEMIC CAUSES OF LID SWELLING
Puffy swollen eyelids may also be seen due to excessive crying or lack of sleep and sometimes during a common cold or sinus infection (sinusitis).
Painless, boggy swollen eyelids of both eyes (bilateral) can also be because of other health conditions like heart, kidney, liver or thyroid disease. In these cases, there may be swelling in other parts of the body also like ankles, feet, abdomen and hands.
Rarely autoimmune diseases like lupus and sarcoidosis may also be associated with eyelid swelling.
Angioedema is a rare condition that causes swelling of the face and eyelids along with the tongue, throat, abdomen, arms and legs. It may be associated with hives and itching and occurs as an allergic reaction to a medicine, insect bite, some plants or food. It can also be a result of an inherited enzyme deficiency condition. It can cause severe breathlessness and is a condition requiring emergency hospitalization and management.
Also read-
For any query, additional information or to discuss any case, write to info@drvarsha.com, and be assured of a response soon.
References: