There are a number of doubts, myths and beliefs about cholesterol and fats in our diet as well as their impact on our health. Let us start by understanding, in what forms do we take fats in our diet –
LIPIDS are a chemical class that includes all oily, fatty substances which do not dissolve in water but dissolve in organic liquids (organic substances contain Carbon which forms ‘covalent’ or electron-sharing bonds with Hydrogen). We take lipids in our diet in the form of FATS and CHOLESTEROL.
FATS
Fats contain ‘fatty acids’ which are made of chains of Carbon (C) atoms forming bonds with Hydrogen (H) atoms. Some of the fatty acids may have double bonds in one or more sites in these chains. At these sites, the fatty acid chain acquires flexibility and can be bent. Fatty acids are a vital component of the membranes that cover and line all the cells in our body. However, only the ‘flexible’ fatty acids can be incorporated and used in the cell membranes.
Understanding Saturated and Unsaturated Fats
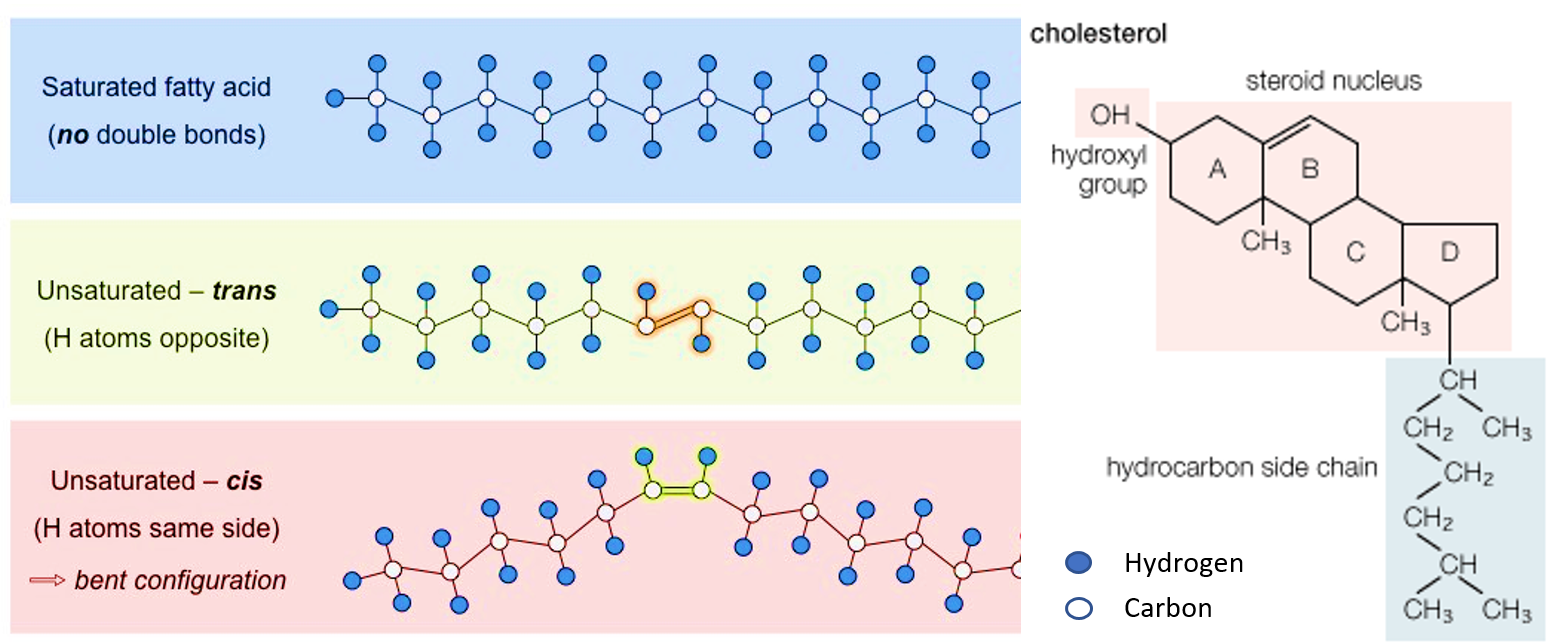
Those fatty acids which do not contain any ‘double bonds’ are called saturated fatty acids. These fats are not flexible and bendable, so do not get incorporated into our cell membranes. They get stored as triglycerides (TGs) by our body in the liver, muscle, and adipose (fat under the skin and in between body organs). This storage form of fat may be used as a source of energy once carbohydrates (carbs) are exhausted. It is also important to note that excess carbs in diet are also converted and stored as triglycerides by our body.
Those fatty acids which contain double bonds are called unsaturated fatty acids or fats. If only one double bond is present, they are mono-unsaturated and if more than one is present, they are poly-unsaturated fatty acids (MUFA and PUFA respectively).
Cis and Trans Unsaturated Fats
It has recently been researched that just having double bond/s does not bestow flexibility on the fatty acid. If both the H atoms are on the same side of the double bond, they are said to be in ‘cis’ configuration while if the H atoms are on opposite sides of the double bond, they are said to be in a ‘trans’ configuration. Flexibility and bendability are present in the cis configuration while the trans ones cannot be bent and are not flexible. So it is the cis unsaturated fatty acid that gets incorporated into cell membranes, while the trans ones go into storage just like the saturated ones.
Most naturally occurring unsaturated fatty acids occur in cis configuration however on deep frying or during processing for packaged foods, the cis configuration is changed to trans (by a process called hydrogenation) which increases the stability and shelf life of these products. Therefore, cis-unsaturated fatty acids are the best forms of fat for us to take in our diet to ensure least is stored or deposited, and more is actively utilized in our body.
PUFAs are additionally also utilized by our body to make some chemical mediators that play an important role in the process of Inflammation. There are 2 types of PUFA – Omega 6 and Omega 3 (the number reflects the position of the double bond). They should be taken in a ratio of around 4:1 in our diet for an effective balance of the inflammatory mediators. However, most diets are low in Omega 3 (that produces anti-inflammatory mediators) with this ratio often going up to 12:1 to 25:1 in favor of the Omega 6 (that produces pro-inflammatory mediators). So it is important to consciously include some sources of Omega 3 fatty acids in our diet.
Medium and Long-chain Saturated Fats
Saturated fatty acids are classified into short-chain (less than 6 C atoms), medium-chain (6-12 C atoms) and long-chain (>12 C atoms). Medium and long-chain saturated fatty acids are found in diet, while short-chain fatty acids are produced by bacterial action on the dietary fibers in the gut. These short-chain fatty acids reduce gut inflammation and strengthen gut immunity, therefore including more fibers (through salads – fruits and vegetables) is beneficial.
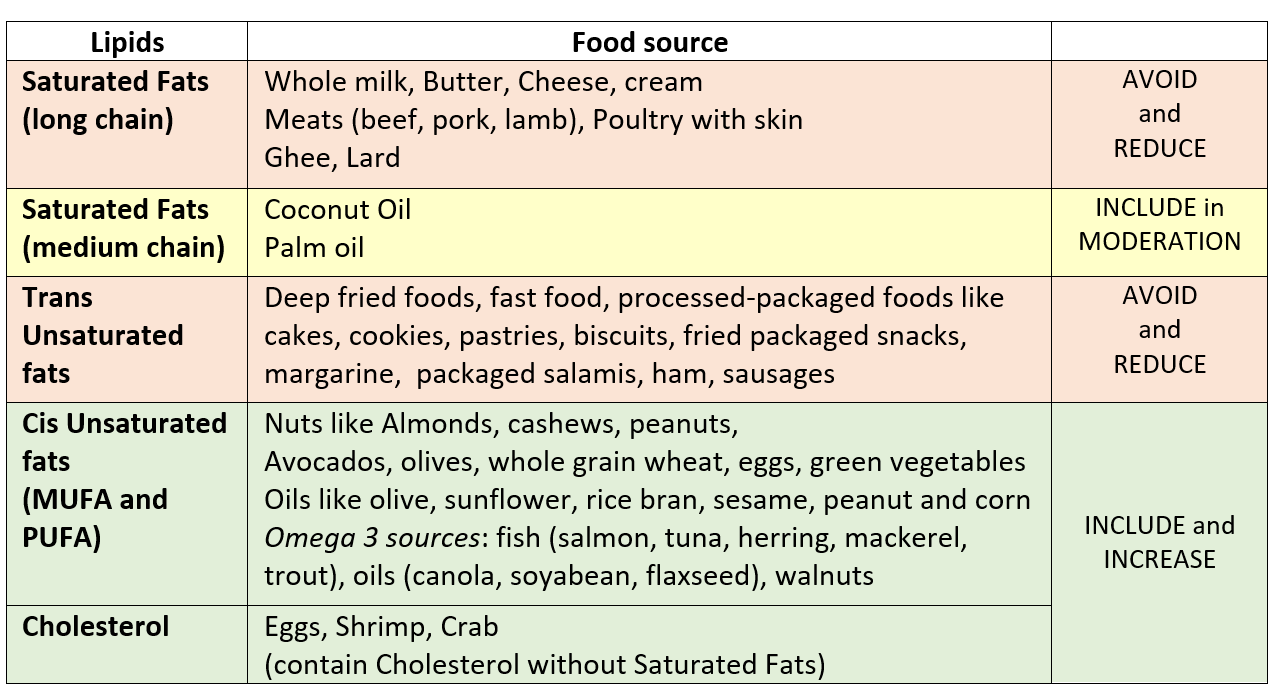
Recent research has shown that the long-chain fatty acids from diet are easily stored as TGs while the medium-chain fatty acids are preferably burned up as a source of energy. So among the saturated fats, medium-chain ones are preferable to include than long-chain ones. Coconut oil and palm oil have 50% and 40% medium-chain saturated fats respectively while other sources from meat and dairy have less than 15% medium-chain and mostly long-chain fatty acids. Coconut oil is also rich in vitamins and minerals so it is the preferred one in the saturated group.
So one should include preferably cis unsaturated fats along with some amount of specifically omega 3 fatty acids and some amount of medium-chain saturated fats in the diet for an appropriate and healthy lipid balance.


CHOLESTEROL
Cholesterol is a type of lipid that has an entirely different structure than fats. It has a complex structure derived from the steroid class of substances. Cholesterol is also an important component of cell membranes and is additionally used by the body to make vitamin D, bile and hormones.
It is found in many foods we take in diet but most of the cholesterol found in our body is synthesized by the body itself (usually 20% from the diet; 80% by the body). Due to the important role of cholesterol in our body, the synthesis of cholesterol is meticulously regulated, which means, if less comes in through the diet, the body will automatically synthesize more and vice versa. Therefore, total cholesterol in the body remains almost constant!


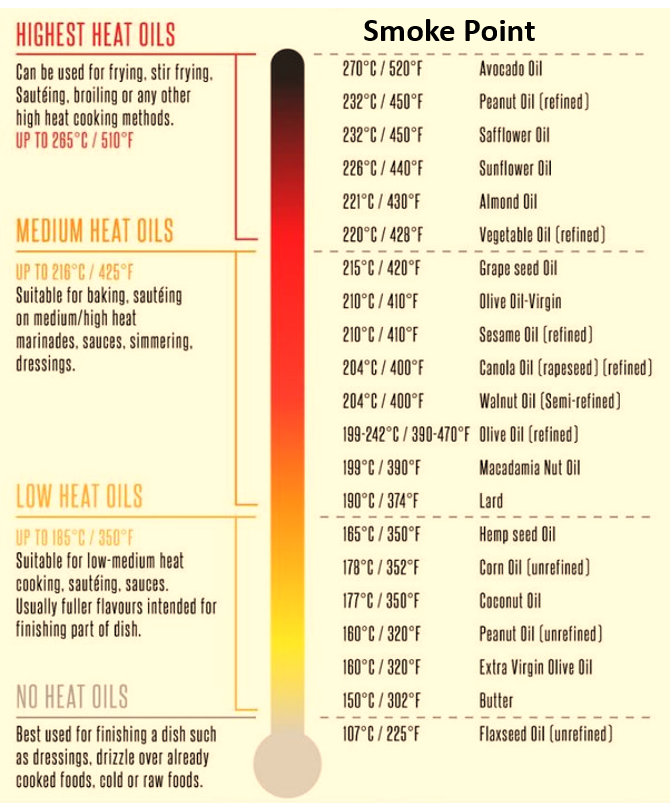
SMOKE POINTS OF OILS
This is the temperature at which an oil smokes or burns, and breaks down the fats into harmful substances like free radicals and carcinogens. Therefore depending on the smoke point of the oil, it should be used in cooking and food preparation appropriately.


HEALTH RISKS WITH HIGH DIETARY FAT AND CHOLESTEROL INTAKE
The fatty acids (fats) are stored in the liver as triglycerides (TGs) along with cholesterol. Special proteins combine with TGs and cholesterol and carry them in the blood to other parts of the body from the liver. Proteins combined with lipids are called ‘lipoproteins’.
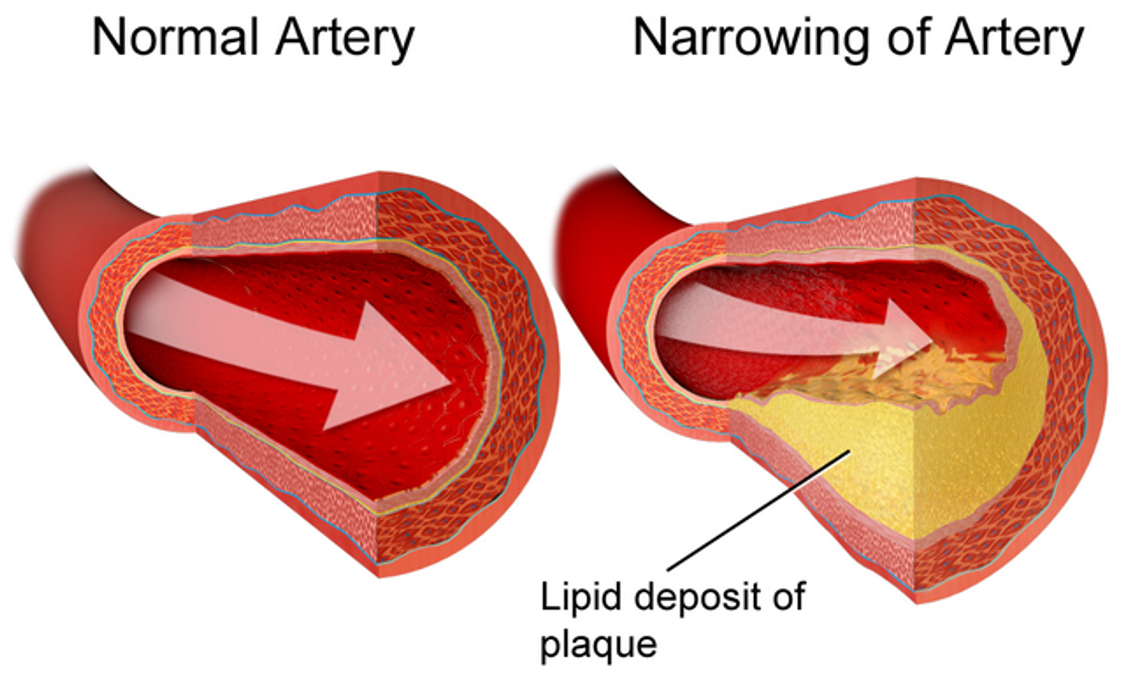
VLDL (very low-density lipoprotein) carries a large amount of TG along with some cholesterol in the blood. After giving off the TG to other storage sites like muscle and adipose, the lipoprotein left behind is called LDL (low-density lipoprotein) which has mostly cholesterol and some TG. VLDL and LDL (especially the latter) if present in high quantities in the blood can form plaques (called atherosclerosis) that can lead to blockages of blood vessels. The smaller and denser LDL has the greatest propensity to form these plaques. The more the number of VLDL and thereby LDL particles circulating in the blood, the more is the risk of plaque formation, atherosclerosis and blood of arteries.
The unutilized cholesterol and TG are brought back to the liver by the lipoprotein called HDL. Therefore, while VLDL and LDL keep the fats in circulation, HDL removes fats from circulation and brings them back to the liver. That is why VLDL and LDL are called bad cholesterol while HDL is called good cholesterol.
The amount of cholesterol we take in the diet has hardly any relevance to the amount of circulating VLDL and LDL particles. Cholesterol plays a supportive role in transporting TGs in blood, and most of the cholesterol body pool remains constant due to well-regulated cholesterol synthesis by the body. However, more the saturated and trans fatty acids we take in diet, the more will be stored in the liver as TGs and more will be the released VLDL and thereby LDL particles circulating in the blood.
Therefore, it is not the dietary cholesterol intake but the dietary intake of saturated and trans fats which increases the risk of developing cardiovascular disease (CVD) due to plaque blockage of arteries (which can result in serious conditions like heart attack and stroke). Plaques are made of deposited lipids (fats and cholesterol) with calcium and some trapped blood cells (RBCs and platelets).
Though the amount of cholesterol intake in diet has no direct risk, most food sources of cholesterol also contain significant amounts of saturated fats. The exceptions here are eggs and shrimp which are now often recommended in the diet without any attributed health risk.


When we measure blood cholesterol, we do not actually measure the amount of cholesterol in our body. What we measure is the amount of cholesterol in VLDL, LDL and HDL particles circulating in the blood. More the VLDL and LDL and less the HDL particles in the blood, the more is the cardiovascular risk due to the formation of plaques in the blood vessels. Lab reports mainly use the amount of LDL and HDL (and sometimes their ratio- ideal LDL: HDL= 3.5-4), as the risk indicator for atherosclerosis and CVD. Apart from this total blood triglycerides is measured which gives us an idea of the body’s fat overload (which in addition to the risk of plaques in blood vessels, also signifies an increased risk of diseases like obesity, diabetes, fatty liver, pancreatitis and thyroid disorders).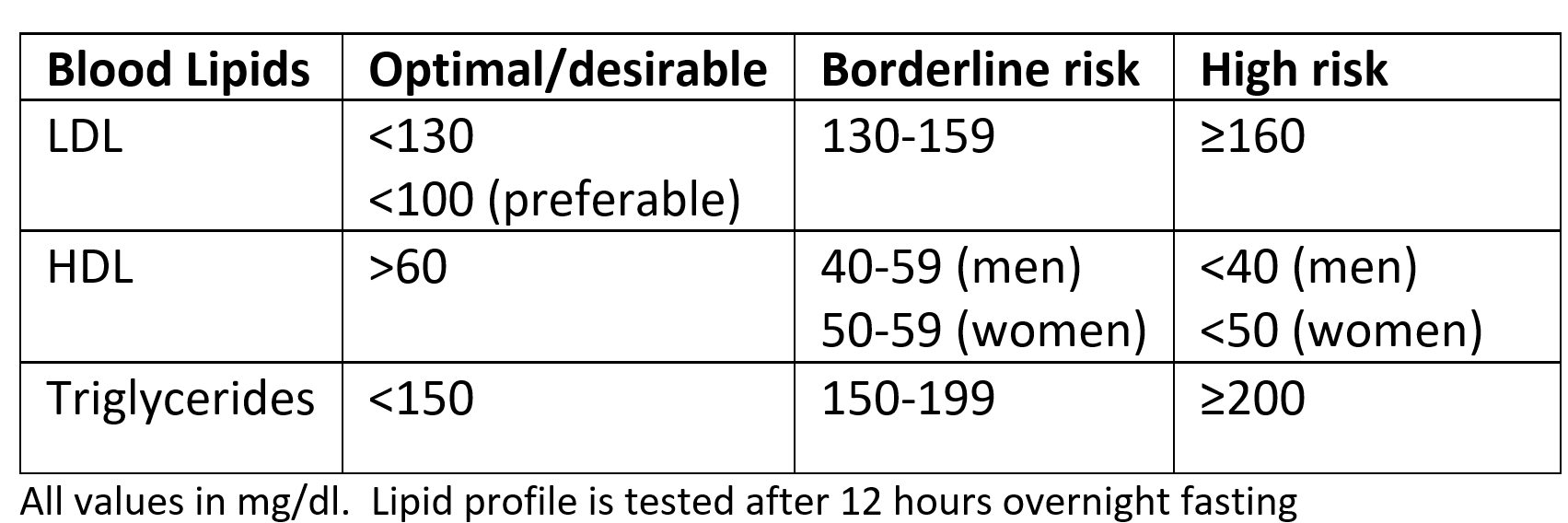


It is important to note that the risk of cardiovascular disease (CVD) is not considered in isolation based on the lab values of blood LDL, and TGs. The risk increases in proportion to the presence of other CVD risk factors like high BP, diabetes, obesity, smoking, physical inactivity, increasing age and family history/predisposition.
Does high-fat load (high blood TGs and LDL) always imply a high health risk?
It is possible that people with high LDL or TGs may never get CVD or plaque-related blockages while people with normal LDL may actually land up with plaques. This is due to other CVD risk factors mentioned. If a person is a smoker or has high blood pressure or diabetes, the component of injury to his blood vessel wall is high. So in such a person even a lower level of LDL can end up forming a significant plaque as compared to a person who doesn’t have any of these risk factors. Similarly, a family history/genetic predisposition, and increasing age (>45 years) may play a role in adding risk. Obesity and lack of physical activity (reduced utilization of carbs/fats leading to more storage) also contribute to increased CVD risk. Increased cholesterol and triglycerides can also be linked to other chronic diseases like fatty liver.
So by how much should we aim to reduce the blood LDL?
The most important intervention if LDL and TGs are high is always a reduction in dietary intake of saturated/trans-fat and a relative increase in intake of PUFAs (especially Omega3).
The more the estimated CVD risk, the greater will be the needed reduction in LDL. So a CVD risk categorization is usually done based on all individual factors and the target LDL is set accordingly as below:
- High risk (2 or more risk factors including diabetes or heart disease): LDL target <100 mg/dl (<70 mg/dl sometimes) or >50% reduction
- Medium risk (2 or more risk factors): LDL target <130mg/dl or 30-50% reduction
- Low risk (1 or no risk factor): LDL target <160mg/dl or <30% (range of 10-25%) reduction
What do these cholesterol-lowering drugs like ‘statins’ do?
The decision to start a ‘statin’ drug is based on the inability to bring down LDL with diet alone and the degree of one’s CVD risk.
The statins lower the amount of cholesterol our body makes so that irrespective of the cholesterol coming through diet, the cholesterol made by our body is reduced. Lower cholesterol in the liver will lead to lower quantities of VLDL and thereby LDL particles coming out in the blood. Therefore, the statin drugs reduce the blood LDL and TGs thereby reducing the risk of plaque formation and CVD. Dietary modifications mentioned have to continue hand in hand.
Specific drugs lowering triglycerides (niacin, fibrates) act by reducing triglyceride synthesis and increasing fatty acid breakdown (oxidation) and are used if one’s fat overload (TG level) comes out to be significantly high. Newer LDL cholesterol-lowering medicines include the PCSK9 inhibitor group of drugs, that act by binding to the LDL receptor on the surface of the liver cells (hepatocyte) preventing and reducing the release of LDL particles and increasing their internal degradation. Omega 3 fatty acids supplements are also given commonly, to improve the lipid balance.
So to conclude, cardiovascular disease (CVD) due to plaque-related blockage of vessels (atherosclerosis) is a complicated interplay of several factors! But the drive home message at a practical level still remains that we reduce saturated/trans-fats in our diet, and much rather keep our LDL and TG level on the optimal or desirable side!
Also Read –
For any query, additional information or to discuss any case, write to info@drvarsha.com and be assured of a response soon.
References
American Academy of Clinical Chemistry Lab tests: Lipid panel


