WHAT IS MULTIPLE SCLEROSIS (MS)?
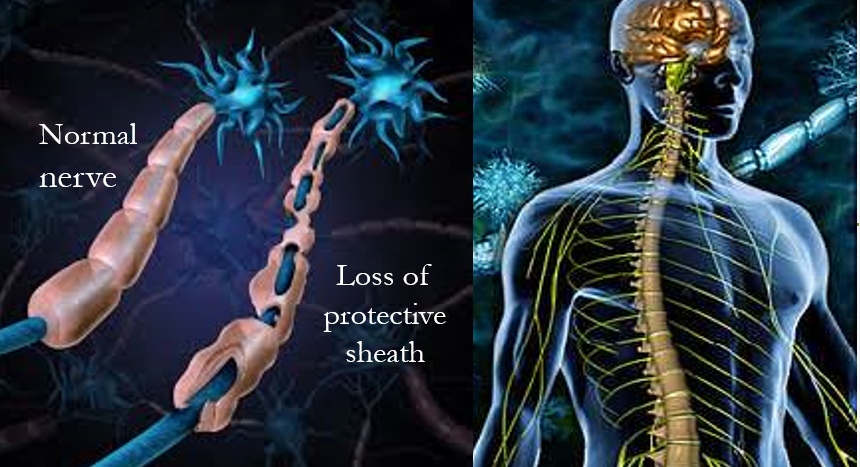
Nerves in our body are covered by a sheath (myelin) which not only acts as a protective covering but also makes the transmission of impulses faster and more effective. In MS, this protective sheath is damaged resulting in the nerves getting exposed and inflamed, and communication between the brain and different parts of the body getting affected. The cause postulated is the abnormal reaction by the body’s immune system (autoimmune response) which attacks and damages this protective sheath. Other examples of autoimmune diseases include inflammatory bowel disease (IBD), type 1 diabetes and rheumatoid arthritis.


WHAT ARE THE SIGNS AND SYMPTOMS OF MS?
The symptoms can vary from person to person according to nerves affected and progression of the disease. Symptoms may start with numbness, weakness, and tingling on one side and progress to tremors, lack of steadiness and co-ordination of movements (ataxia), difficulty in walking, dizziness, slurred speech and significant fatigue. An electric shock-like feeling while moving the neck, and burning pain or touch-temperature sensitivity in the limbs may be seen. Eye problems like blurring, double vision, pain on eye movements and even complete/partial loss of vision may also be manifesting symptoms.
Severe symptoms and complications include muscle spasms and leg paralysis, disturbed functioning of bowel and bladder, affected sexual function, sometimes seizures, as well as mental health issues like depression, mood swings and memory lapses.
The disease can have episodes of ‘flare-up’ when symptoms are strong, followed by prolonged periods of remission and control. However, with progression, the disease may eventually show constant symptoms. While MS can affect anyone, the risk is higher if one has another auto-immune disease or a family history of MS. Smokers have a tendency for more recurrent flare-up’.
HOW TO DIAGNOSE MS?
Diagnosing early multiple sclerosis (MS) requires a combination of clinical evaluation and diagnostic tests. Imaging tests include brain and spinal cord MRI scans to detect lesions. Other tests like evoked potential (EP) measure nerve responses. A lumbar puncture to analyze cerebrospinal fluid (CSF) for inflammatory markers, along with various blood tests to rule out other conditions, is recommended. Ophthalmic examination and Optical Coherence Tomography (OCT) are also important.
HOW IS MS TREATED?
Diagnostic tests used for MS include brain scans (MRI), blood tests to rule out other or co-existing health conditions, and sometimes a spinal tap to test for specific antibodies.
Though there is no cure, MS may be controlled to improve quality of life through a holistic approach of lifestyle modification, and medicines.
Lifestyle modification
The following factors may help in coping better with MS-
- Being in cool environments
- Adequate rest and sleep
- Exercises like walking, stretching, swimming, cycling, yoga or aerobics. Physical and occupational therapy for these strengthening and stretching exercise schedules is recommended
- Stress management, relaxation techniques and hobbies.
- Support groups and counseling
- Nutritious diet with vitamin D supplementation
Medical therapy
Medicines are given firstly for controlling the inflammation during flare-up periods, secondly to control and improve symptoms, and thirdly to reduce relapses and slow the progression of the disease (DMT- Disease-Modifying Therapy).
For controlling the inflammation, medicines like corticosteroids are usually used.
Some medicines may be prescribed to control a particular prominent symptom like muscle relaxants, anti-depressants, medicines to improve sleep, bladder or bowel function, reduce fatigue and increase walking speed.
Medicines to slow the progression of disease (DMT) include:
Oral drugs
- Sphingosine 1 phosphate receptor modulators: fingolimod, siponimod, ozanimod, and ponesimod (USFDA approved March 2021)
- Fumarates: dimethyl fumarate, monoethyl fumarate
- Others -Teriflunomide (pyrimidine synthesis inhibitor), cladribine (purine antimetabolite)
Injected drugs
- Peginterferon beta-1a and 1b
- Glatiramer acetate (injected into skin/muscle)
- Cladribine (IV infusion)
- Biologicals (Monoclonal Antibody agents -MAbs): ocrelizumab, alemtuzumab, ofatumumab (USFDA approved August 2020), rituximab, and natalizumab.
These medicines given in MS act as immune-suppressive agents and therefore patients taking them should be protected for and monitored for infections. Drugs used in MS may have side effects, therefore they should be taken only under the guidance of a Neurologist.
Procedures that are used to treat MS patients include autologous hematopoietic stem cell treatment (aHSCT) which is intensive chemotherapy combined with reinfusion of blood stem cells to rebuild the immune system and plasmapheresis which is a technique of plasma (fluid and protein component of blood) exchange.
PRECAUTIONS AND CARE FOR MS PATIENTS
All people with MS are advised to pay attention to and follow guidelines for reducing the risk of infection, especially during a pandemic like COVID. Older people with MS, especially those who also have lung or heart diseases, should take extra care to minimize their exposure to the viruses and pathogens.
Precautions: The World Health Organization recommendations during any epidemic or pandemic include:
- Wash hands frequently with soap and water or an alcohol-based hand rub
- Avoid touching eyes, nose and mouth unless hands are clean
- Keep at least 1-meter distance between yourself and others, particularly those who are coughing and sneezing
- When coughing and sneezing, cover your mouth and nose with a flexed elbow or tissue
- Practice food safety by using different chopping boards for raw meat and cooked foods, and wash your hands between handling them.
- Avoid large public gatherings and crowds, and use of public transport during such a period.
- Where possible, use alternatives to face-to-face routine appointments (for example,video or tele-consults)
- Caregivers and family members who live with, or regularly visit, a person with MS should also follow these recommendations to reduce the chance of bringing infections into the home
- People with MS who are currently taking DMTs like alemtuzumab, cladribine, ocrelizumab, rituximab, fingolimod, dimethyl fumarate, teriflunomide or siponimod are at increased risk of infections.
MS and Infections
- If an MS patient suffers from an infection, then it is recommended to consider stopping DMT [injectable or oral] or delaying the next IV infusion. The MS specialist or Neurologist will advise when it is safe to restart DMT.
- If someone was diagnosed with MS and is planning to choose between various DMT, some are safer than others. Before starting on any new DMT, people with MS should discuss with their healthcare professional which therapy is the best choice for their individual disease course and disease activity in light of infection risk in the region.
- One should consider selecting a treatment that does not reduce specific immune cells (lymphocytes) like interferons, glatiramer acetate, or natalizumab, and avoid medications that reduce lymphocytes over longer intervals like alemtuzumab, cladribine, ocrelizumab, and rituximab.
- If already taking DMT, do not change or stop your medication without first speaking to your MS team. If you have an appointment to come to the hospital for a review or treatment, and you have a cough, high temperature, or shortness of breath, please contact your MS team for advice.
- If you are on interferon beta 1a or 1b, glatiramer, teriflunomide, dimethyl fumarate, or natalizumab, please continue to take these drugs. They do not significantly increase the risk of systemic viral infection.
- If you are on fingolimod (or siponimod, ozanimod), please be aware that the risk of viral infections is moderately increased, making you more prone to coronavirus infection and its complications. For most people on fingolimod, this risk is outweighed by its effectiveness in controlling their MS. So, we recommend most people continue on fingolimod and not stop it without speaking to one’s MS team, because there is a risk that MS will become active and cause relapses in the weeks after stopping the drug.
- Recommendations on delaying second or further doses of alemtuzumab, cladribine, ocrelizumab, and rituximab during epidemics differ between countries. People who take these medications and are due for the next dose should consult their healthcare professional about the risks and benefits of postponing treatment.
- Autologous hematopoietic stem cell treatment (aHSCT) severely weakens the immune system for a period of time. People who have recently undergone this treatment should extend the period they remain in isolation during a pandemic. People who are due to undergo treatment should consider postponing the procedure in consultation with their healthcare professional.
Vaccination in people with MS:
Inactivated Vaccines are generally safe for most MS patients, even those on certain disease-modifying therapies.
- Influenza (Flu) shot given annually, protects against severe illness and death from flu. The injectable shot, not the nasal spray (which is a live vaccine), should be given.
- COVID vaccines have not shown any evidence of increasing MS complications, worsening or relapse, and are recommended annually.
- Tetanus/Diphtheria/Pertussis (Tdap) Booster for those not up-to-date on boosters, can be given.
- Hepatitis B vaccine is recommended for those at risk.
- Pneumococcal Vaccine must be given for protection from pneumonia and invasive pneumococcal disease
- Shingles Vaccine (Shingrix®) is recommended for adults 50 and over, and for those age 19 and over who are on specific MS medications.
- Human Papillomavirus (HPV) vaccine is recommended for some patients regardless of age, especially those on specific treatments.
Live Vaccines are generally not recommended in MS as these carry a risk of causing illness in people with compromised immune systems from certain MS medications. These include Measles-Mumps-Rubella (MMR), and Varicella (Chickenpox).
Some of the drugs used in MS may decrease or dampen the immune response to vaccines. These may be high-dose steroids, or DMT drugs that include the sphingosine 1 phosphate receptor modulators (fingolimod, siponimod, ozanimod), and more so with cladribine, and biologicals alemtuzumab, ocrelizumab, ofatumumab, and rituximab.
It is best to consult your neurologist to guide you on the timing and schedule of the mentioned drugs and vaccines.
Dr. Praveen Gupta is a renowned Neurologist, and currently the Chairman of Marengo Asia International Institute of Neuro and Spine, Gurugram, India. He has established two Neurology departments in Paras and Artemis corporate hospitals. He also started the first Stroke center in Gurugram, was the first to use ‘solitaire’ for mechanical thrombolysis and started DBS (Deep Brain Stimulation) for epilepsy in Asia. He is frequently invited as speaker for advanced interventions in all kinds of stroke, botox, cerebral palsy, multiple sclerosis, epilepsy and Parkinson’s disease. He has been recognized by Forbes India as one of the Most Influential Global Healthcare Leaders in India.
Further reading-
Dementia and Alzheimer’s Disease – Awareness, Understanding and Solutions
Understanding Tremors – Parkinson’s Disease and Other Conditions
References-


