WHAT IS IBS AND WHAT ARE ITS SYMPTOMS?
Irritable bowel syndrome (IBS) is a disorder that affects the large intestine of our body, causing repeated disturbed bowel symptoms which can sometimes significantly impaired Quality of Life (QOL).
The signs and symptoms of IBS can vary from person to person. The most common ones include abdominal pain or cramping that is typically relieved or partially relieved by passing a bowel movement, feeling excess gas or bloating, diarrhea or constipation which can in some cases be alternating, mucus in the stool and sometimes nausea.
Most people with IBS experience certain times when signs and symptoms get worse, and times of improvement or even complete absence of symptoms. IBS is seen more commonly in women, and people under 50 years of age. Around one-third of cases may have underlying psychological factors like anxiety and depression
HOW IS IBS DIAGNOSED?
There is no specific test by which IBS can be diagnosed. IBS is a clinical diagnosis based on the history and symptoms of the patient. Blood, stool or other tests may be ordered only to rule out or diagnose other/co-existing conditions. IBS is diagnosed based on the following Symptom criteria (Rome IV):
- Recurrent abdominal pain, on average, at least 1 day/week in the last 3 months, associated with 2 or more of the following symptoms:
- Pain related or relieved by the passing of stool
- Associated change in frequency (number of times) of passing stool. (also includes symptoms of excessive straining during passing stool, urgent/sudden-uncontrollable need to pass stools, and a feeling of incomplete evacuation.)
- Associated change in form or consistency (appearance- watery or too hard) of stool.
Above criteria should be fulfilled for the past 3 months with symptom onset at least 6 months prior
- Other symptoms supporting a diagnosis of IBS include gas (flatulence) with bloating or mucus in stools
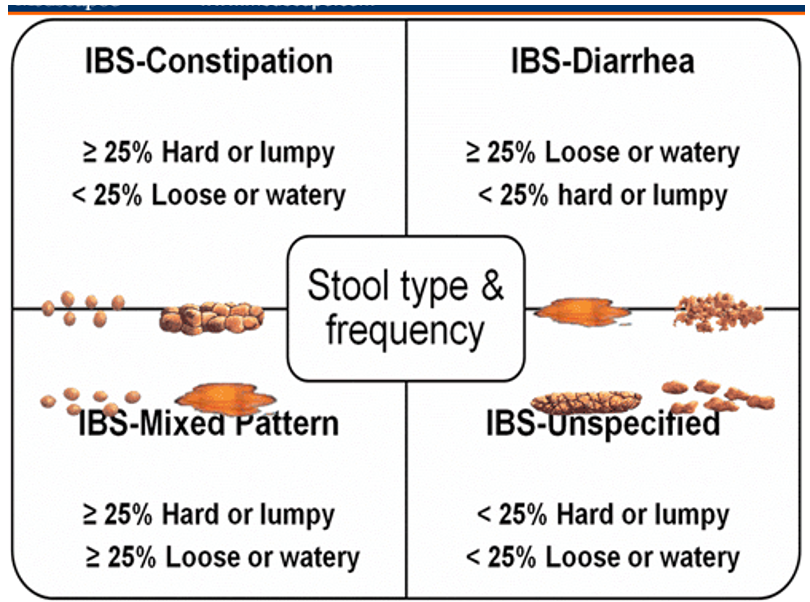
WHAT ARE THE TYPES OF IBS?
IBS is classified based on whether diarrhea or constipation is the predominant symptom along with abdominal pain.


WHAT ALERT SIGNS AND SYMPTOMS POINT TOWARDS ANOTHER DISEASE AND NOT IBS?
If any of the following are present, additional investigations are recommended, and other clinical diagnoses apart from IBS should be explored.
- Onset after the age of 50 years
- Unintended weight loss
- Symptoms at night time or disturbing sleep
- Major or sudden change in day and night symptoms
- Recurrent vomiting
- Blood in the stools or presence of Anemia
- Fever
- Any mass or swelling in the abdominal
- Family history of colon cancer or Inflammatory Bowel Disease (IBD)
WHAT IS THE CAUSE OF IBS?
There are multiple causative factors linked to the pathology of IBS. The most accepted scientific explanation is that IBS occurs due to, or a combination of – Abnormal nerve signals between the Brain and Gut (Brain-Gut Axis), Abnormality in the motility (contraction and relaxation movements) of the Intestine, and Hypersensitivity (lowered pain threshold) of the Intestine to stretching by stools/gas, certain food items, and substances like drugs/medicines.
There is often an exaggerating influence of stress, anxiety, depression and even hormonal changes (during PMS in women) on IBS symptoms. A role in IBS has also been postulated of Gut immunity and inflammation or a change in the local ‘good’ bacteria which help in digestion, nutrition and preventing infections. In some genetic factors and a family history of IBS may be present.
Sometimes patients of IBS may also have a condition known as SIBO (Small Intestinal Bacterial Overgrowth). This is due to abnormal and harmful bacteria growing in the small intestine that cause abdominal pain, gas, and changing stool patterns. SIBO is diagnosed by tests to detect hydrogen/methane gases in the breath.
HOW IS IBS MANAGED AND TREATED?
IBS health measures involve Lifestyle therapy, Diet therapy, along with Drug therapy and in some cases, Psychotherapy.
LIFESTYLE THERAPY
Reassurance and awareness are important that though it is a long term, sometimes a life-long condition, it is not a serious or life-threatening disease. This is important to understand for both patient and family members. Also, IBS does not increase the risk of any cancer, or any other serious condition. IBS has a waxing & waning course, and with appropriate health measures, it can be well controlled to live a full-filled life.
Regular physical exercise and adequate (at least 8 hours) sleep, along with stress management (through Yoga, breathing exercises and meditation) are recommended and beneficial.
DIET
Major or drastic dietary restrictions or modifications are usually not required. It is important to identify triggers foods, and avoid them. Reducing caffeine, alcohol, fatty foods/gas-producing foods, milk/milk products is useful. High fiber diet is useful, especially in constipation-type IBS. The amount of fiber intake should be increased gradually by 3 to 6 grams every 1-2 weeks. Water should be taken adequately of at least 2 to 2.5 liters a day.
A group of difficult to digest carbohydrates called Fermentable Oligo-, Di-, Mono-saccharides And Polyols (FODMAPs) should be reduced and avoided in diet, to reduce IBS symptoms and improve quality of life.
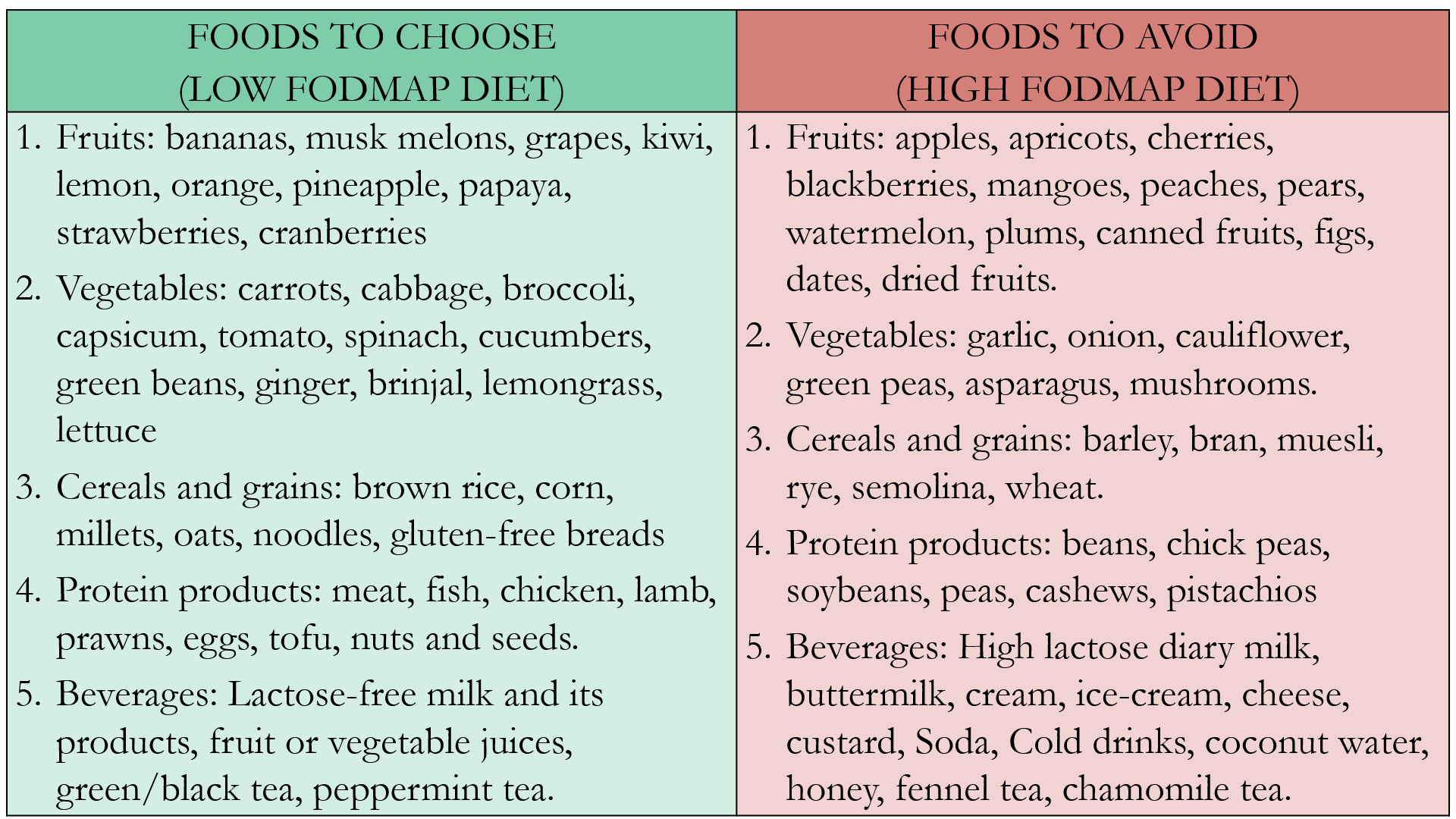


Sugar and glucose are considered Low FODMAP. Artificial sweeteners like Saccharin and Aspartame are Low FODMAP, while Xylitol and Sorbitol are High FODMAP. Spices like turmeric, fenugreek, saffron, chili, and asafoetida may be used in cooking
SYMPTOM-DRIVEN DRUG THERAPY
The treatment of IBS needs to be customized as per the symptoms of each patient, and the symptoms vary widely in the same patient at different times, therefore symptomatic treatment is the usually preferred approach.
To reduce abdominal pain, antispasmodic agents (like Mebeverine) are used.
If constipation is the predominant symptom, laxatives are used in treatment. These laxatives may be fiber or Bulk type (like Psyllium husk), Osmotic type (Poly-ethylene glycol PEG or Lactulose), Stimulant type (Sodium picosulphate, Biscodyl), Secretory type (Lubiprostone, Linaclotide), or Prokinetic type that increase intestinal motility (like Prucalopride).
When diarrhea is the predominant symptom, antidiarrheal agents like Loperamide, Cholestyramine, Rifaximin or Ramosetron may be used.
Probiotics are basically doses of good gut bacteria, which may also sometimes be added to treatment. Sometimes, Pancreatic enzyme supplements may also be used part of the treatment regimen.
Sodium butyrate, a short-chain fatty acid, shows promise as a treatment for IBS due to its anti-inflammatory and gut health-promoting properties. Studies suggest it can alleviate IBS symptoms like abdominal pain, bloating, and irregular bowel movements by potentially normalizing gut health and reducing gut hypersensitivity
In certain refractory cases or where a psychological/mood basis is also associated, antidepressants (TCA group in IBS-D and SSRI group in IBS-C) or Anti-anxiety agents (like Chlordiazepoxide) may be added to treatment.
SIBO, if present, is treated with a course of Antibiotics.
PSYCHOTHERAPY
Psychological counseling and support, often coupled with behavioral/cognitive therapy are recommended and helpful. Even though psychological therapy or medicines may be used in IBS management, IBS is not a psychological or psychiatric disease and the symptoms are real and definite, not imagined
Dr Manish Bhatnagar is the Director and HOD of Gastroenterology at ICON HOSPITAL, Vastrapur, Ahmedabad, Gujarat. He is a fellow of the American Gastroenterology Association as well as the American College of Gastroenterology. He was awarded the Times Health Icon of India in 2018 and 2019. He has special interest in Bowel diseases and was the first to do the Fecal Microbiata Transplant (FMT) in western India. He has several national and international publications and book chapters to his credit.
Also read:
Constipation – Multifactorial Problem Needing Multifaceted Health solutions


