UNDERSTANDING TEARS AND DRY EYES
‘Dry eyes’ is a common problem, and can present at any time or age.
Symptoms of Dry Eyes
Dry eyes present as a tired and sandy feeling in the eyes. Keeping eyes open may be difficult especially after prolonged screen work or reading, and the eyes appear dull or sometimes red. Dry eyes can also cause blurring of vision, and a sticky sensation in the eyes which leads to a constant desire to repeatedly clean or remove mucus from the eye.
Composition of Tears
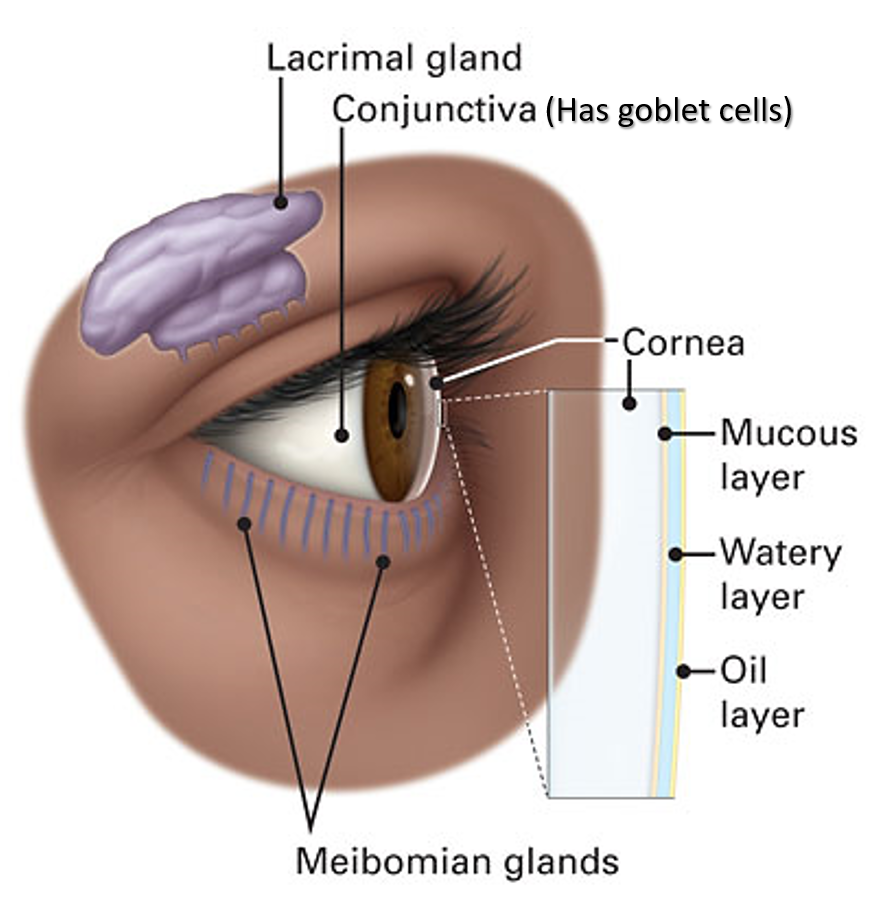
Tears have 3 components –
- Inner mucous layer- It is sticky and helps spreads the tears, and also protects and nourishes the surface of the eye. It is produced by cells of the conjunctiva called goblet cells.
- Middle watery (aqueous) layer – It maintains fluidity and lubrication of the tears. It is produced by the lacrimal (tear) gland in the upper outer portion of the eyeball socket (orbit).
- Outer oily layer- It reduces evaporation of tears and also prevents constant overflow. It is produced by the meibomian glands in the eyelids.
Dry eyes can occur due to abnormality in any of the 3 tear components.


Production of Tears
Tear production is of two types –
- basal (normally required to keep eyes healthy, moist and comfortable)
- reflex (tearing due to emotional stimulus, or eye irritation/trauma).
While basal tears are proportionally made up of the 3 layers mentioned above, reflex tears come predominantly by nerve stimulation of the lacrimal gland, so are more watery and overflow easily. Regular blinking helps in uniform distribution and reduced evaporation of basal tears. Tears drain out of the eye through the tear duct with openings (puncta) at the inner nasal side of the upper and lower eyelids.
The term Dry Eye Syndrome (also called KCS – Keratoconjunctivitis sicca) refers to inflammation of the cornea and surrounding conjunctiva due to dryness of eyes.
Factors leading to Dry Eyes or Dry Eye Disease (DED)
Dry eyes can occur due to one or a combination of the following factors affecting the basal tears:
- reduced production
- altered proportion of components
- improper spread or distribution on the eye surface
- increased evaporation
Dry eyes can paradoxically lead to more tearing due to eye irritation and discomfort which may increase reflex tearing from time to time. So, while the presenting symptom may be watering of eyes or too much tearing, the actual diagnosis may be dry eyes!
CAUSES OF DRY EYES
Here are 10 possible causes of dry eyes to be kept in mind –
Aging: There is a decrease in basal tear production with increasing age. Dry eyes are more common in people above the age of 50 years. In women, hormonal changes during and after menopause can also cause dry eyes (as may also occur during pregnancy).
Prolonged screen time: The absence of adequate blinking due to prolonged staring and focusing on the screen leads to increased tear evaporation and lack of effective tear distribution. This is one of the most common causes of dry eye in current times and is seen across children, teens, and adults. This is now considered part of the Computer Vision Syndrome (CVS). The heat emanating from gadgets further aggravates the problem. Sometimes dry eyes may also happen with prolonged daily reading or driving.
Environmental causes: AC blast on the face, working in hot dry environments, or occupations involving prolonged exposure to dry heat, wind blasts, hot plates/gas stoves, ovens, hairdryers, etc. can be causes of dry eyes. Air pollution and smoke are also known causes of dry eyes and eye irritation.
Eye allergies: This may not be the direct cause of dry eyes, but may often co-exist and aggravate dry eyes. Similar environmental factors can trigger eye allergies and dry eyes, and often medications used to treat allergies can cause dry eyes. Eye allergies and irritation can also increase the mucus component of the tears which can make the eyes feel less moist and more sticky.
Medications: Medicines like antihistamines (antiallergics), decongestants, hormone replacement therapy (HRT), oral contraceptives, antidepressant or antianxiety pills, some drugs for high blood pressure, acne medicines (retinoids), and drugs for Parkinson’s disease also cause dry eyes by affecting tear production and composition. Prolonged use of eye drops in chronic eye conditions (like glaucoma) can cause dry eyes due to preservatives in the drops, which cause ocular surface and tear film abnormalities.
Vitamin A deficiency: This is a cause to be considered especially in children (xerophthalmia) and in people eating a diet low in vegetables (greens and carrot), and other food items like fish, walnuts and oils.
Cornea problems – Abnormalities of the surface of the cornea (the central transparent portion of the eye) can cause dry eye due to loss of tear film spread and uniformity. This may be seen in people who wear contact lenses, temporarily after LASIK (eye number correction by laser), or due to corneal conditions like epithelial dystrophies.
Eyelid problems: The openings of the meibomian glands in the eyelids just behind the eyelash layer might become clogged (meibomian gland dysfunction – MGD). As these glands produce the oily layer of the tears, in such cases the tears can become stickier, and the watery layer evaporates more easily, resulting in a feeling of dry eyes. Blepharitis, a common eyelid inflammation, significantly contributes to dry eye syndrome by disrupting meibomian gland function, and the two conditions often occur together, sharing symptoms like redness, itching, burning, and gritty sensations in the eyes. Rarely, abnormalities of the eyelid contour (out-turning or ectropion and in-turning or entropion), and conditions preventing proper eyelid closure can also affect tear film distribution and evaporation, leading to dry eyes.
Systemic diseases: There are certain conditions associated with dry eye syndromes (keratoconjunctivitis sicca), and a combination of problems like dry eye, dry mouth, dry skin and joint inflammation due to immune-system mediated (auto-immune) mechanisms. These include Sjogren’s syndrome, rheumatoid arthritis, lupus, scleroderma, graft vs. host disease, and sarcoidosis. Some disorders like hyperthyroidism (Grave’s disease) or Parkinson’s disease can lead to dry eyes due to lid retraction and decreased blinking.
Post-procedures: Surgeries or radiation therapy for cancers in the region, can lead to removal or damage of the lacrimal gland, with dry eyes being an expected consequence.
COMPLICATIONS OF DED
Dry eyes decrease quality of life as they make normal daily activities like reading, driving, cooking, screen work, etc. more uncomfortable. As tears protect the eye surface, a reduction in the amount and quality of tears can increase the risk of eye infections, as well as eye surface injuries like abrasions and ulceration of the cornea, which can produce long-lasting and vision-impairing corneal scars.
PREVENTION AND TREATMENT OF DRY EYES
Dry eyes are diagnosed by a detailed history of symptoms, lifestyle, occupation and personal-family health conditions. Many medications (as discussed above) being used, can cause dry eyes (sometimes along with dry mouth) as side effects and may need to be reviewed.
A thorough eye examination is recommended to diagnose certain underlying eye conditions causing or associated with dry eyes, like eyelid problems, corneal surface abnormalities and eye allergies, which will need treatment/correction. Eye number testing and right glasses should also be given where required.
Some eye tests performed by the eye specialist can confirm the diagnosis of dry eyes.
Tests for Dry Eyes
- Tear film meniscus height on a slit lamp eye examination: A tear meniscus height less than 0.25 mm is suggestive of dry eye
- Schirmer’s filter paper strip test: < 10 mm of moisture on the filter paper in 5 minutes is considered to suggest a deficiency of tears and the presence of dry eyes. Values below 5mm are suggestive of severe dry eye.
- Tear film break-up time (normal 10-35 sec) with dye tests like fluorescein: Fluorescein tear film break-up time – FTBUT<5 seconds is diagnostic of dry eye and tear film instability. Values between 5-10 sec, should raise suspicion and are to be evaluated along with the blinking rate.
- Other more advanced tests for dry eye eyes include tear film osmolarity, tear function index, meibomian gland scans, and tear film bio-markers (like MMP9, lysozyme, lactoferrin).
- Often many of the above tests may be within normal limits or borderline, but patients’ perception of dry eye may be significant, especially if lifestyle, screentime, or environment is the cause. Therefore standardized validated dry eye questionnaires are as important as objective tests in evaluating dry eye and assessing response to treatment. (Dry Eye–Related Quality-of-Life Score Questionnaire DEQS, Dry Eye Questionnaire DEQ, Ocular Surface Disease Index OSDI), etc.)
Lifestyle measures
Avoid working in hot and dry environments. If using ACs for cooling, sit in such a way that the blast does not come on your face. Using air humidifiers can also be helpful. Avoid proximity to smoke and direct hot air blasts (like dryers, fans, heaters, etc.) on your eyes/face, and if professionally inevitable then protective goggles (with top and side protectors) and shields may be used.
Try and reduce screen time. While doing prolonged screen work on laptops/desktops or mobiles, remember to blink frequently. To train yourself to blink more, try to get in the habit of blinking every time you breathe.
Computer screens should be positioned slightly below eye level to prevent too much lid opening and tear evaporation. Every 20 minutes (or at least whenever u remember), take a 20-second break and focus on something 20 feet away (usually towards the end of a standard-size room or best look out of the window if there is one). Then close your eyes and rotate the eyes slowly first clockwise 3 times, then anticlockwise 3 times, in 3 sets.
If wearing contact lenses, regulation of wearing time, care in insertion and removal, and proper hygienic storage is important.
Contrary to some notions, repeated washing or splashing water on the eyes does not help to relieve dry eyes, and may even worsen it. Tap water composition is not at all similar to natural tears, and repeated splashing/washing can remove or drain out more natural tears.
Lubricant drops/gels
Artificial tears or lubricant eye drops/gels are available for over-the-counter purchase and by prescription. Commonly used substances in these drops include methylcellulose (HPMC-hydroxy propyl methylcellulose, and CMC – carboxymethylcellulose), dextran, glycerin, hypromellose, polyethylene glycol (PEG-400), polysorbate, polyvinyl alcohol (PVA), povidone, and propylene glycol, along with sodium/potassium salts. Hyaluronic acid/sodium hyaluronate is a more gel-like ingredient, remains longer in the eye, provides more effective lubrication, and can be used in moderate-severe cases.
Some of these eye drops also come as preservative-free formulations that can be in the form of packs of single-dose/use unims, for long-term and frequent use. Sodium perborate is a preservative that breaks down into water and oxygen upon contact with enzymes in the tears, so is preferred in lubricant eye drops. Technologically advanced nano-preparation and inserts (rice grain size – to be placed under the eyelid) are also now available.
Lubricating eye drops can be instilled 3-4 times a day, or more frequently when needed in the eyes. They are usually very well tolerated but sometimes can produce transient blurring, redness or stinging/irritation. It is advised to remove contact lenses while putting lubricant eye drops.
Latest Medicines for Dry Eye
When moderate-severe dry eye is present and not responding to conventional lubricant eye drops, newer medicines that suppress inflammation may be prescribed.
Cyclosporine ophthalmic solution 0.1% in the form of emulsion eye drop acts by immune-modulating mechanisms to reduce inflammation and improve tear production of the lacrimal gland. This medication is particularly useful when dry eye syndromes are present, and can also be given orally or by injectable route in rheumatoid arthritis and Sjogren’s syndrome.
Lifitegrast eye drop is another medication now available for moderate-severe dry eye. It acts by preventing attachment of inflammatory cells, thereby decreasing inflammation and improving tear production. It’s often used along with cyclosporine.
Acoltremon ophthalmic solution 0.003% is a novel treatment that stimulates tear production by activating TRP senso-receptors on the surface of the eye, and is a first-in-class treatment that provides rapid increases in tear production and is a first-line option for those with dry eye disease.
New eyedrops have been launched for specific causes of dry eye.
Lotilaner ophthalmic solution 0.25%, is the first FDA-approved treatment for Demodex blepharitis, an eyelid condition linked to dry eyes caused by microscopic mites.
Perfluorohexyloctane ophthalmic solution is the first drug specifically for dry eye caused by Meibomian gland dysfunction (MGD). It works by producing oil-like lipids to prevent tear evaporation and stabilize the tear film. It is water-free and preservative-free, applied twice daily.
Meibomian gland inflammation (meibomitis) or clogging, should be treated with lid scrubs, warm compress, massage techniques and antibiotics (ointment or drops).
If eye allergies are present along with dry eye, antiallergic eyedrops (antihistamines, cromoglycate or corticosteroids) in combination with lubricants will be needed.
Eyedrops prepared from one’s own blood have also been used to treat unresponsive or severe dry eye. These are autologous serum drops made by centrifugation of one’s own blood for removal of red blood cells, and then made as an isotonic saline solution.
Cornea-protecting and moisture-retaining contact lenses (bandage contact lenses) may be given in certain cases.
Oral drugs for dry eye
Other drugs that may be prescribed in dry eye syndromes include cholinergics (pilocarpine, cevimeline) that help increase tear, saliva, and sweat production, especially in Sjogren’s syndrome.
Vitamin A deficiency, when suspected, should be treated with vitamin A supplementation available as eye drops, oral capsules, and injections.
Meibomian gland inflammation (meibomitis) may sometimes need an oral course of antibiotics.
Antioxidant and herbal oral supplements are sometimes prescribed for dry eye and eye fatigue, however, their scientific evidence should be evaluated adequately. Recently, some herbal extracts like Maquiberry and Bilberry, taken orally have been shown to improve lifestyle and screen time-related dry eye, due to their anti-oxidant and anti-inflammatory properties. Omega-3 fatty acids, particularly EPA and DHA, can help with dry eye symptoms by improving tear film stability, reducing inflammation, and supporting the quality of meibomian gland secretions. However, clinical evidence is not robust, and doses required are high.
Coexisting health problems contributing to dry eye, like thyroid problems, Parkinson’s disease, autoimmune conditions causing dry eye syndromes, and hormonal disturbance, would need diagnosis and management.
Procedures and Surgeries
Sometimes procedures may need to be performed to treat problems of dry eye, like closing/plugging the tear duct that drains the tears (punctal occlusion with silicone/acrylic plugs, or heat cautery) and tarsorrhaphy (joining the upper and lower lid on the side with a stitch to narrow eye aperture and reduce tear evaporation). Correction surgeries for eyelid contour abnormalities (ectropion/entropion) are also performed where required.
Rarely advanced surgeries have been considered like transplanting salivary (saliva producing) glands in place of an abnormal/damaged/absent lacrimal gland, or eye surface surgeries with amniotic membrane/stem cell transplants.
Also read-
Laptop and Computer use – solutions to reduce adverse health impact
For any query, additional information or to discuss any case, write to info@drvarsha.com, or leave a message in the
box below, and be assured of a response soon.
References


