Headache is a common symptom that everyone experiences at some point or the other which typically lasts a few hours to a day or two. This happens due to common causes like stress, tension, lack of sleep or late night hangovers, overstrain due to reading or computer work, increased heat, dehydration or being in the sun, or having a cold or fever. These headaches are generally transient with an attributable short-term reason, and usually do not require investigation or treatment (barring 1-2 doses of pain-relieving medicine occasionally).
Chronic Headaches
The term chronic headache refers to those which occur frequently (15 days or more in a month), for a significant period (6 months or more). Simply put, if one has a headache more days in a month than not, and this has been happening over a few months, it points to a chronic nature of headache which may call for a medical consult and treatment.
95% of chronic headaches are not due to any serious causes or brain disorders so that should be re-assuring. The commonest causes of chronic headaches which may be distressing but not serious are Tension headaches, Migraines, Cluster headaches, Eyestrain headaches, and Sinus headaches. Once these are ruled out, other rarer causes may be investigated.
COMMON TYPES AND CAUSES OF HEADACHE
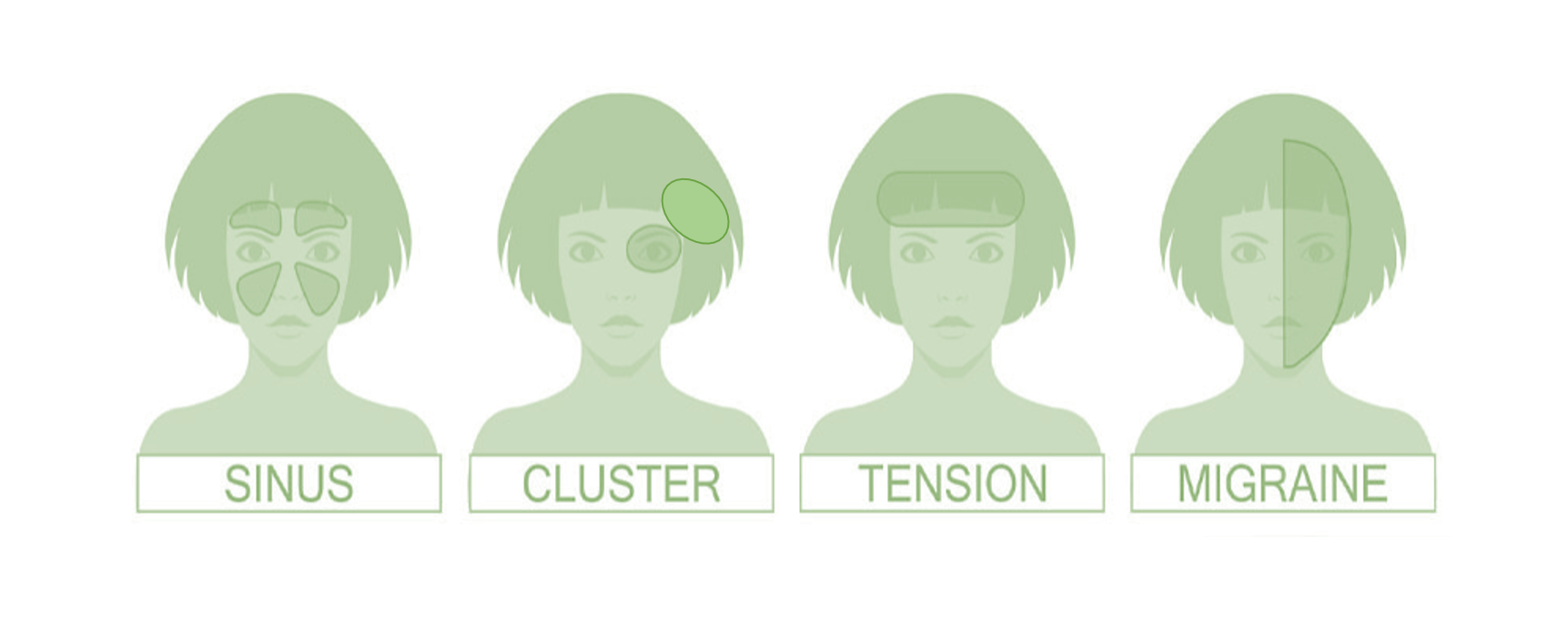
Tension headaches
These are the most common type of headaches (>80% cases). They are dull, constant, pressing, squeezing and ‘band-like’ in nature. They usually affect both sides across the forehead (bilateral), temples or back of the head, and even around the eyes. These headaches are of mild-moderate intensity, and can last a few hours or continuously for several days, and then often spontaneously go away.
Tension headaches usually start by late morning/afternoon and worsen by the end of the day. They are not worsened by physical or daily activities and do not wake a person from sleep. Usually, no other accompanying symptoms are there. Women are affected more and the age group is generally the 30s and 40s.
Migraine headaches
These are ‘throbbing’ (pulsing) in nature and can come on suddenly. These headaches often start at the onset of puberty itself and may reduce in frequency into late adulthood. They can affect one side of the head at a time or sometimes both sides together too.
The migraine headache may be preceded by an aura in 25% of cases (like seeing flashes/lines of light, temporary loss of part or one half of vision for a few minutes, or tingling/altered sensations). The headache itself can last for 4 hours to 4 days and is often accompanied by increased sensitivity to light, sound, smell, and sensations, with nausea and vomiting and sometimes dizziness.
Typical triggers include sleep disturbance, hunger, certain food items, acute stress, sunlight, and loud noises. The person often gets relief by sleeping or being in a cool, dark place. Migraine is more common in women and may present as part of the premenstrual syndrome (PMS) or in those having hormonal imbalance at puberty or perimenopause, and if taking hormone pills. Family history may also be present in 50% of these people.
Cluster headaches
These are severe and stabbing or throbbing in nature, and are almost always one-sided. They are typically felt behind and around one eye, forehead, and side of the head, and can spread to the cheek and teeth. They frequently wake a person up from sleep. They often have accompanying tearing, running nose, or stuffy nose. Rarely on the affected side, the lid may droop, the eyeball may appear more inside and the face may be dry due to lack of sweating or be flushing red, as compared to the other side.
These headaches can last from 15 minutes to 2 hours and can happen daily for several weeks, followed by months/years of headache-free intervals. They are mostly seen in men in the 30-50 year age group. The cause is attributed to hypersensitivity of the trigeminal nerve that supplies the face and eyes.
Sinus headaches
They are usually felt on the forehead, cheeks, and upper teeth area. There is a feeling of fullness or a ‘heaviness’ which is aggravated by looking down, bending, or lying down. Changes or heaviness in voice or a nasal twang may be prominent. There is usually a history of nasal stuffiness, frequent colds or nasal allergy.


Eye strain headaches
Such headaches are usually due to extensive reading, computer/laptop or mobile use especially in inappropriate light conditions, wrong postures or in moving vehicles. Eye strain headaches are also due to uncorrected eye numbers and may be accompanied by a decrease in vision.
Far vision may be blurred with difficulty in reading small prints on signboards, room boards, or on TV, with a conscious or unconscious narrowing or squeezing of lids to improve visual clarity. Near vision loss with age typically after 40 years is perceived by the need to move the reading material further away from the face, for clarity.
These headaches are worse at the end of the day and are typically felt at the lower part of the forehead and brow.
Exertion Headaches
Exertion headache, (also called exercise headache), occurs during or after physical activity like aerobics, running, straining, coughing/sneezing, lifting weights, or intercourse. It is throbbing or pulsing in nature and usually affects both sides. It comes on quickly and lasts a few minutes to hours to up to two days. Exertion headaches can be very severe and also sometimes be associated with nausea, vomiting, visual changes, and light sensitivity, similar to migraine. The cause may be due to dilation of blood vessels caused by exertion.
Such people should avoid activity in extreme temperatures, or in high altitudes. One should stay well hydrated, and wear appropriate clothing. Do not over-exert or perform sudden high-intensity exercise. Warm-up and cool down properly. Do not exercise if tired or have not had adequate sleep. Varying type of exercises sometimes helps to identify the triggering activity.
MANAGING CHRONIC HEADACHE
For any chronic headache, it is wise to start with recording the pattern of the headache for 1-3 months by maintaining a headache diary for the following-
- frequency (number of days in a month)
- duration (hours)
- severity (scale of 1-10)
- character (frontal band-like, one-sided, whole head, etc.)
- onset (sudden or gradual)
- other associated symptoms
- impairment of normal daily activities (work/studies, hobbies/fun, etc)
- triggers or aggravating factors (stress, noise, lights, foods, exercise, lack of sleep, gadgets, sun/heat, cold, etc.)
- relieving factors (sleep, rest in a dark quiet room, distraction/fun, outdoor walk, exercise, music, etc.)
- need and relief with painkiller
This is to be followed by a basic medical consultation to discuss and understand and qualify the headache as being Tension, Cluster or Migraine headache, or attributed to other causes/types. ENT (Ear and Nose/Sinus), Eye Examination (including vision check, number correction, eye pressure, and retina examination), BP measurement, and basic blood tests like CBC, and blood sugar will help diagnose if eye strain, sinusitis, or high blood pressure, anemia and high blood sugar are present and responsible for the headache. Regularly wearing tight headgear or hair-styles which pull and tie the hair tightly can also contribute to chronic headaches.
The doctor may order imaging tests like CT scan, MRI, angiography or spinal tap (lumbar puncture) depending on clinical suspicion and the presence of atypical signs or red flag signs mentioned below.
Some drugs and food items have been linked with chronic headaches and these can also act as trigger factors for migraines. These if avoided can help in improving response to headache treatment. Such drugs include amphetamines, barbiturates, chronic use of painkillers (analgesic abuse), opioid drugs, cocaine, contraceptives and increased use of sleeping pills (sedative abuse). Food items linked to a chronic headache include MSG (monosodium glutamate), nitrates in preserved meats, alcohol abuse/binge drinking, chocolates, cheese and overuse of caffeine.
Lifestyle modification often helps in many cases of Tension headaches. These include regulating and improving sleep, a healthy diet, adequate water intake, timely meals, and regular exercise. Postural and ergonomic corrections while using computers, laptops, mobile phones, reading and working, and including relaxation techniques and enjoyable hobbies into the daily routine are advised. These measures also have a favorable impact on migraines and cluster headaches and can help improve response to medicines. Stress management can also help relieve headaches.
Medicines prescribed include over-the-counter analgesics (pain killers) like aspirin, ibuprofen, diclofenac, naproxen, and paracetamol. The triptan group of drugs or rarely the older ergotamine drugs are used for treating migraine. Other medicines like propranolol, flunarizine, and topiramate are used to prevent migraines. Medicines like sodium valproate and gabapentin through antiepileptic drugs are also used to improve relief in some cases of migraine and tension headaches. Recently introduced, the oral drug lasmiditan and ubrogepant/rimegepant, and nasal spray zavegepant are medications used for the acute treatment of migraine with or without aura in adults. They are not useful for prevention.
Cluster headaches don’t usually respond to painkillers and are treated with triptans, or medicines like lithium, ergotamine (ergot) drugs, local anesthetics, octreotide, course of corticosteroids (prednisolone or methylprednisolone), or oxygen inhalation. Rarely surgery may be considered. Verapamil and lithium are drugs sometimes used to prevent cluster headaches.
Medicines to control nausea may also be added to the treatment.
Anxiety and depression, or psychological trauma can also manifest as chronic headaches. Depression typically leads to morning headaches upon waking up. Evaluation of mood disorders by a psychiatric referral can help in bringing out and treating these causes with appropriate counseling and medicines. Medicines relieving anxiety and depression are also sometimes prescribed for tension headaches.
All the mentioned medicines should be taken strictly under medical guidance, prescription, and monitoring.
Stress management can also help relieve headaches.
RED FLAG SIGNS AND RARER CAUSES OF HEADACHE
The following associated signs are alert signs of conditions in the brain causing the headache which should be promptly investigated:
- Sudden, severe, unbearable splitting headache with no prior history
- High fever (>101 F) or fever with neck stiffness
- Fit (convulsion) episode
- Bleeding from the nose
- Sudden vomiting without nausea
- Loss of consciousness or fainting
- Mental confusion or clouding and difficulty understanding speech
- Double vision or loss of a part, field, or segment of vision
- Pain worsening on changing position, coughing, sneezing, or straining
- Frequently losing balance, difficulty in walking or weakness/tingling sensations on one side of the body
- History of head injury or any area of head painful to touch
- Night sweats, unexplained weight loss
- Slurring of speech, difficulty in talking or hearing
Investigations may include further blood tests, a neurological consult, examining brain fluid (cerebrospinal fluid-CSF) by lumbar puncture, and brain scans (CT/MRI). These tests can help rule out causes like brain hemorrhage, tumors, and infections (meningitis, encephalitis or pus collections-abscesses), as well as diseases, malformations, clots or tears in the brain blood vessels.
FACIAL PAINS
Neuralgia
Neuralgia is a sharp, piercing type of pain that follows the path of an irritated or damaged nerve. The trigeminal nerve carries sensations to the brain from the face including the cheek, jaw, teeth, gums, lips, or sometimes the eye and forehead. The condition is therefore called trigeminal neuralgia.
Neuralgia can occur due to pressure on a nerve or a ganglion (cluster of nerves) by a swelling (pus, blood collection-hematoma, tumor mass or foreign body). It can also be caused by damage of the nerve caused by infections (like herpes, syphilis, TB), trauma, multiple sclerosis or other inflammatory nerve diseases.
The pain is severe, may come in flashes, and involve any part or many parts of the face, sometimes with headache and neck pain. The person affected has severe pain while talking, eating, swallowing, yawning and brushing.
The diagnosis is established by a neurological examination and MRI. Trigeminal neuralgia is treated with specific medications that include analgesics, muscle relaxants and anticonvulsants. Sometimes decompression procedures to relieve the pressure on the nerve, or destroying the affected nerve by radiation or radio-frequency maybe performed.
Temporo-Mandibular (TM) joint
The joint of the lower jaw with the skull about which the opening and closing movement of the jaw occurs is called the Temporo-Mandibular (TM) joint. This joint may become painful and inflamed and the most common cause for this is an ill-fitting denture or dental malocclusion.
Pain and tenderness (pain on touching), around the TM joint area, spreading to the ear, head or neck, and aggravated by chewing or yawning, should prompt this diagnosis. A dental check-up to remove the offending cause, followed by rest for the jaw and pain-controlling medicines, help recovery in a few days to weeks.
Further reading-
Not getting enough sleep can be detrimental to health: Tackling Insomnia
High Blood Pressure (BP) – Risks and Solutions for Hypertension
Depression and Anxiety – Causes, Signs and Holistic Treatment
Laptop and Computer use – solutions to reduce adverse health impact
For any query, additional information or to discuss any case, write to info@drvarsha.com, and be assured of a response soon.
Reference
American Migraine Foundation- Chronic daily headaches


