Maintaining a healthy weight and body mass index (BMI), and tackling overweight and obesity issues in a timely and effective manner can have a beneficial impact on not only reducing the risk of several lifestyle and chronic diseases but also improving their medical management and outcome.
BMI (Body Mass Index)
BMI represents one’s proportional weight. Absolute weight on the weighing scale or just considering weight for age standards can be misleading as it does not take into account one’s height and therefore proportionality and distribution of body weight.
The figure below shows how to calculate BMI, and the definition of underweight, overweight and obese according to BMI calculation.
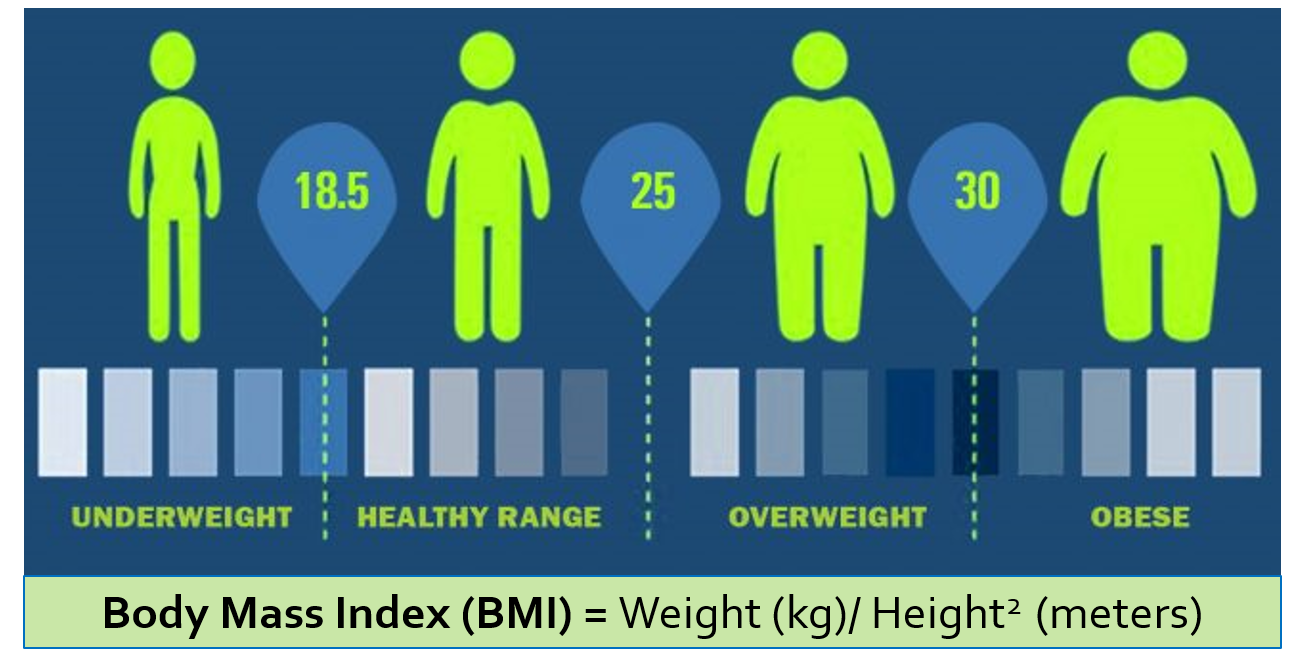


It is important to note that the BMI does not tell you whether the body weight is due to excess fat or muscle mass. So, though BMI may be a fair indicator for most adults of average height, it can be interpreted falsely in people who are very tall or athletic. People engaged in sports training and bodybuilding can have a high BMI attributed to increased muscle mass (protein) and not fat, therefore they do not carry any of the health risks or concerns that an overweight or obese person does.
BMI values in children are interpreted based on charts with the 5th and 85th being the for underweight and overweight cut-offs.
Being either underweight or obese increases the risk of mortality from many diseases.
Fat distribution – Subcutaneous and Visceral Fat
A very valuable indicator that complements the BMI value is assessing the fat distribution in the body. Fat deposits in our body can be subcutaneous (that is under the skin) or visceral (around internal organs). Subcutaneous fat is what one can pinch with the hand, and is not considered a high health risk. However visceral fat, seen mainly as what is also called abdominal/belly fat which is around the mid-region of the body (waist and stomach area) is of concern and associated with increased health risks.
Belly fat or abdominal is attributed to body fats (lipids: cholesterol and triglycerides), as well as to sedentary lifestyle and inappropriate diet, and is studied to stimulate the release of inflammatory mediators contributing to cardiovascular disease (CVD), fatty liver, and other chronic diseases.
A simple way to differentiate if the fat in your abdomen is subcutaneous or visceral is to lie down flat, and see if the abdomen flattens (subcutaneous fat) or not (visceral fat). The shape of the abdomen being like a ‘pear’ or ‘apple’ can also indicate subcutaneous or visceral fat respectively, but this assessment may be subjective and less reliable. Fat around the thigh, hips and buttocks which is common in most women, is not associated with increased health risk, unlike what was thought previously.



Waist Circumference
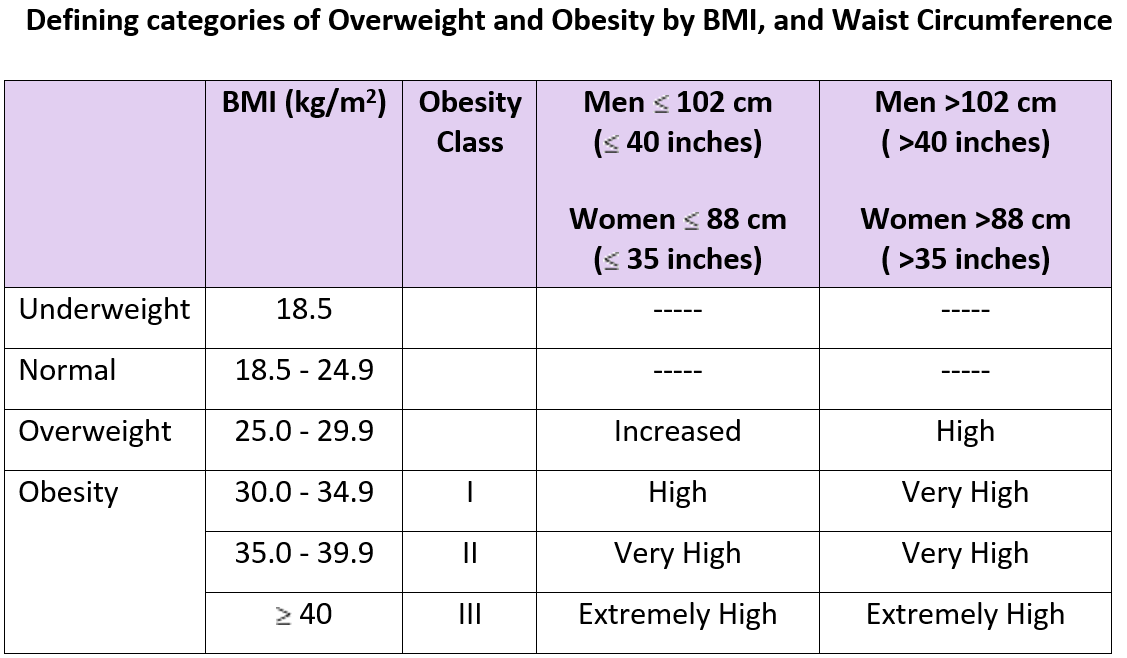
The waist circumference (WC) can also be a complimentary guide to BMI to assess obesity and health concerns. Increased obesity-related health risks are associated with a WC ≥ 94 cm in men and 80 cm in women. However substantially increased health risk with increased BMI is considered in a man with WC ≥102 cm, and women with WC ≥ 88 cm.
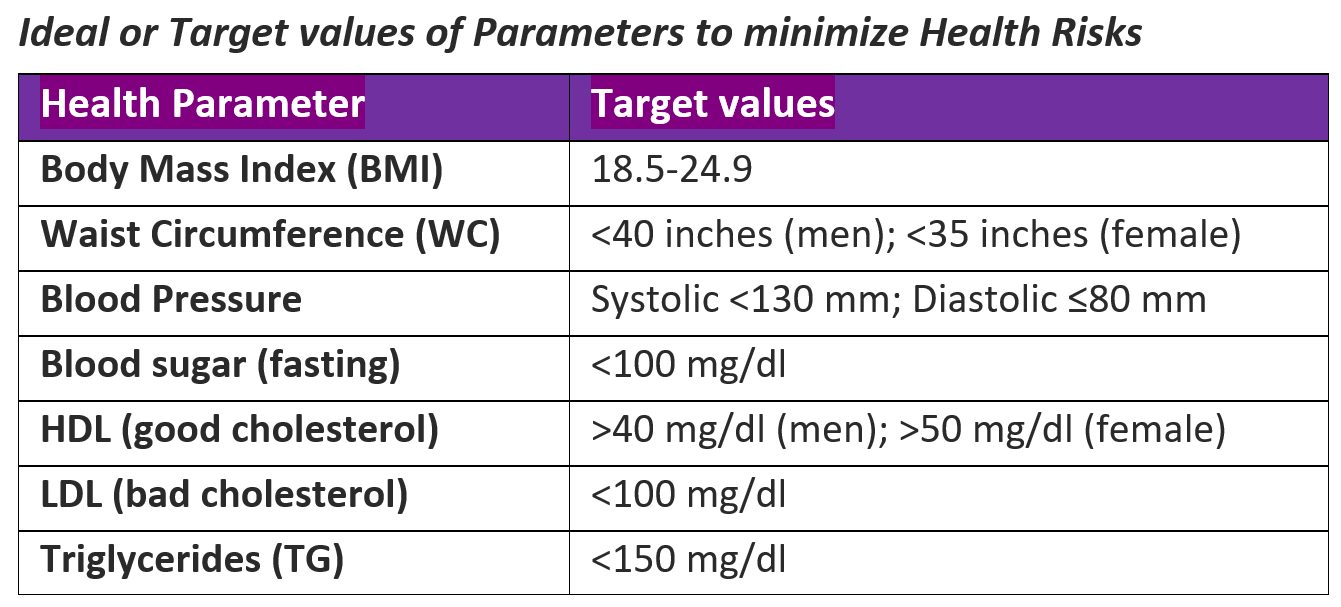
For adults who have a BMI in the range of 25-35kg/m2, the WC and the BMI along with visible fat distribution should be correlated with other health parameters like blood pressure (BP), blood lipids (LDL cholesterol and triglycerides) and diet/lifestyle to determine the overall health risks especially of hypertension, diabetes type II and CVD.


Health Impact of High BMI and Obesity
High BMI and Obesity can increase the risk of developing health problems given below:
- Hypertension (High BP)
- Diabetes Type II
- CVD (Cardiovascular disease – includes angina, heart attack and stroke) and Heart failure
- Fatty Liver Disease
- Gall bladder stones
- Kidney disease
- Osteoarthritis
- Osteoporosis
- Sleep Apnea
- Mood disorders
- Certain Cancers
- High BP and Increased blood sugar during pregnancy, the increasing complication rate


In addition, the presence of obesity can be a poor prognosis factor (increase the complication and mortality rate, or delay recovery) in certain conditions like Asthma, Chronic Obstructive Pulmonary Disease (COPD) and also COVID-19 (Coronavirus disease).
A 5% or more maintained weight reduction can improve a patient’s cardiovascular risk profile, lower the risk of diabetes, reduce the risk of bone problems (osteoarthritis and osteoporosis), and improve quality of life. However, larger weight loss (>10%) may be needed in patients with obesity and sleep apnea, or lung problems like chronic bronchitis and asthma.
Diet and Lifestyle Measures
Dietary guidance
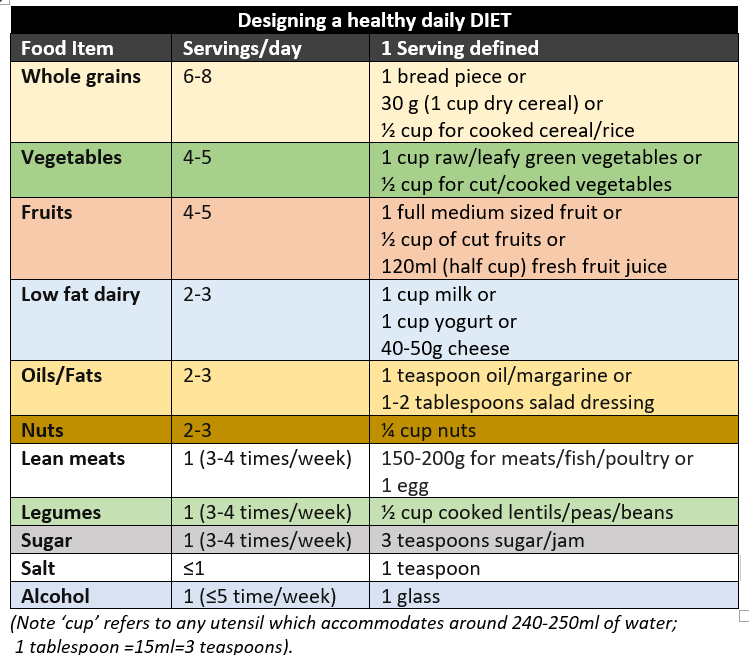
The two most important steps for reaching and maintaining target BMI and optimal health are an appropriately nutritious diet, and regular physical activity or exercise. The guide below can be used to design a healthy diet for oneself and the family. However, if obesity or cardiovascular risk factors are present, additional restrictions in both total amount of food intake and calories, as well as types of food items to select or avoid, may be given by the nutritionist or physician.
People who are overweight and tending to obesity or those already in the obese category should follow a structured weight loss and physical exercise program under expert guidance.


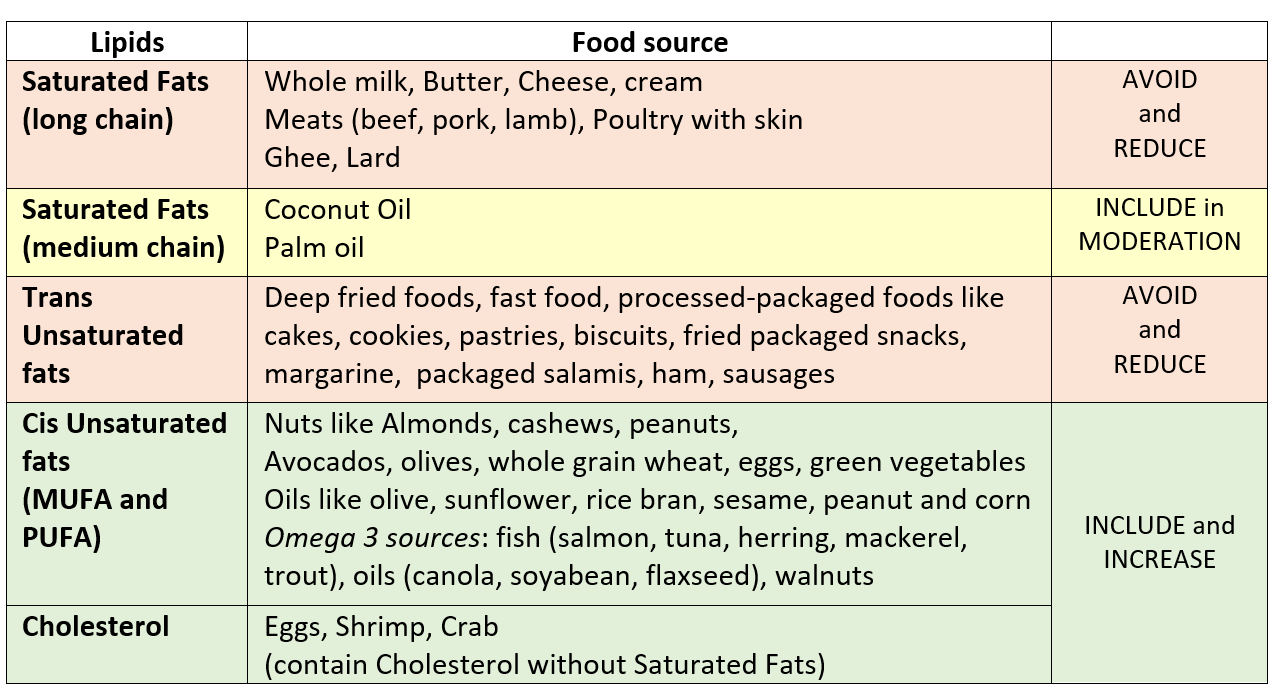
*Oils and Fats (Lipids) can be of various types as shown below. Therefore, it is important to take care and select the food items you eat based on what types of lipids are present in them.


Physical Activity
Daily half-hour to 45 minutes (90-150 minutes/week) of physical exercise is advocated to maintain BMI as well as general health, wellness and fitness. These exercises can include brisk walking, jogging, aerobics, yoga, swimming, cycling or playing a sport.
People with health conditions like cardiovascular disease, respiratory conditions like asthma and COPD, or bone-joint problems like arthritis and spondylitis, should consult their physician before starting on any new, or strenuous exercise regime. Sudden intense exercise or bouts can cause more damage than benefits, therefore a warm-up and cool-down period should be included, with duration and intensity of exercise scaled up gradually over a few days.
Regular Medical Check-up
People who are overweight and tending to obesity, or those already in the obese category should have regular medical check-ups, especially after the age of 40 years.
A general physical examination, weight and blood pressure measurement, along with blood parameters like complete blood counts (CBC), blood sugar and lipids (cholesterol and triglycerides), kidney and liver function tests, and in some cases ECG and urine test, are usually the tests evaluated part of a regular/routine medical check.
An annual medical check-up is adequate if there are no associated cardiac conditions or risk factors. However, more frequent check-ups may be recommended if any health parameters are abnormal, if you are on medications, or have other risk factors for developing any of the conditions related to obesity as mentioned.
Medicines for Weight Loss
People who are overweight (>27 BMI) with comorbidities like hypertension, diabetes, etc., and tending to obesity, or those already in the obese category, can benefit from drugs for weight loss.
Weight loss medicines, such as semaglutide (Wegovy, and generics) and tirzepatite (Mounjaro), belonging to the class called GLP1– receptor agonists, are drugs that are considered among the most effective for long-term weight management. These drugs work by suppressing appetite, reducing cravings, slowing stomach emptying, and increasing satiety. These medicines should be used in conjunction with a healthy diet and exercise plan.
(Read in detail – weight loss GLP1-RA drugs)
Studies show 10-20% weight loss over a year with these drugs. The most common side effects are mild-moderate gastrointestinal (GI) effects (nausea, vomiting, diarrhea, constipation, dyspepsia, and abdominal pain). It is advised to monitor GI side effects and renal function, and especially avoid use in patients with severe gastroparesis (stomach not emptying properly), history of pancreatitis or gallbladder disease, risk factors for colo-rectal cancer, and reduced kidney function. Regular ophthalmic retina exam, and being vigilant of muscle loss (sarcopenia) and psychiatric effects, are also recommended.
Therefore, indiscriminate use by anyone wanting to lose weight should not happen. Individualized prescribing decisions after thorough evaluation of patient fitment by approved indication, risks, lifestyle and diet should always be the way to go with regular and meticulous monitoring for adverse effects.
Ready availability of these drugs without prescriptions or medical consultations in pharmacies and online platforms often marketed as miracle weight-loss solutions, should be strictly curbed and stopped. For those without diabetes, or not having high BMI and comorbidities, who still want to lose weight for personal or professional reasons, lifestyle modification with supervised healthy diets and physical exercise is always the most appropriate. Those who qualify for a GLP1-RA based on approved indications, priorities to address include:
• patient-centred initiation and weight loss/ health goals
• baseline screening, including usual dietary habits, emotional triggers, cravings, and all associated relevant medical conditions
• comprehensive exam including muscle strength, function, and body composition assessment
• lifestyle assessment including aerobic activity, strength training, sleep, mental stress, substance use, and social connections
During GLP-1 RA use, apart from strict monitoring and vigilance for adverse effects as mentioned, nutritional counselling, preventing nutrient deficiencies, preserving muscle and bone mass through resistance training with diet, and connecting to support groups and digital platforms are also important to improve compliance, as well as long-term weight maintenance post-cessation.
Recently, an over-the-counter GLP1-RA korglutide has been introduced as an oral health supplement for weight loss. However, there is no published data in a peer-reviewed medical journal, nor have full results, especially related to side effects (short or long-term), been disclosed. So currently, it would still be preferable to take a doctor’s opinion first.
Other weight loss drugs include bupropion-naltrexone combination oral medication that may be helpful for people who experience emotional eating.
Orlistat is an oral medication available in both prescription and over-the-counter forms that works by blocking the absorption of fat in the digestive system.
It is crucial to consult with a healthcare provider to determine the right medication for you, as they all have different mechanisms and potential side effects, some of which can be serious if not monitored properly.
Weight loss medications are most effective when used with a healthy diet and regular exercise routine.
Also read:
Cardiovascular Disease (CVD) – Understanding Atherosclerosis and Coronary Artery Disease
Incorporating the DASH diet to reduce BP, BMI and Cardiovascular risk
For any query, additional information or to discuss any case, write to info@drvarsha.com and be assured of a response soon.
References
Health Risks of being Overweight – NIH
Guidelines on Overweight and Obesity – NHLBI
Relationship between risk factor reduction and degree of weight loss – EHJ