WHAT IS ALLERGIC RHINITIS AND WHY DOES IT OCCUR?
Allergic Rhinitis (AR) is an allergic condition of the nose (nostrils). Often this can be associated with other allergic conditions like that of the eye (allergic conjunctivitis), lower respiratory tract (asthma), skin (atopic dermatitis/eczema) and sometimes various food allergies.
AR is characterized by a group of symptoms occurring due to exposure and response of the lining of the nose (nasal mucosa) to allergens. These could be seasonal environmental allergens like pollen, or indoor ones like house dust mite (HDM), and sometimes certain foods or insects (like cockroaches) and fungus (molds). AR is also sometimes called hay fever.
The cause is linked to a combination of genetic predisposition and environmental factors leading to altered balance and responses of the immune system. Some of these environmental causes implicated include a reduction in natural surroundings and habits, more use of processed items, and increased indoor/outdoor pollution. However, there is much individual variation, and lack of conclusive evidence. At an immune response level, AR is induced by an IgE antibody-mediated immune response to a specific allergen resulting in the release of histamine from mast cells, as well as activation of other immune cells and inflammatory mediators.
Allergic rhinitis is the most common respiratory disorder in most countries of the world and the 4th most common disease worldwide (WHO). It is estimated that more than 600 million people suffer from this condition, and it is the commonest allergy encountered in clinical practice. 30-40% of patients have coexisting asthma.
SYMPTOMS AND TYPES
The 4 cardinal symptoms of AR are:
- Sneezing
- Itching in the nose
- Running or watering nose (rhinorrhea)
- Stuffy nose (nasal congestion)
The symptoms of AR are very similar to those of the common cold. Therefore 2 or more of the cardinal symptoms should be present for more than 1 hour on most of the days to be diagnostic of AR.
Other co-existing signs-symptoms, or conditions can be-
- Watery, itchy and red eyes (allergic conjunctivitis)
- Dark circles under the eyes (allergic shiners)
- Headache and sinusitis
- Wheezing (with co-existent asthma)
- Ear fullness/pain (serous otitis media)
- Dry/irritating cough or scratchy feeling in the throat
- Itching on the roof of the mouth-palate
- Sleep difficulty and/or snoring
- Grinding/clenching teeth (bruxism)
- Difficulty in concentration, and fatigue
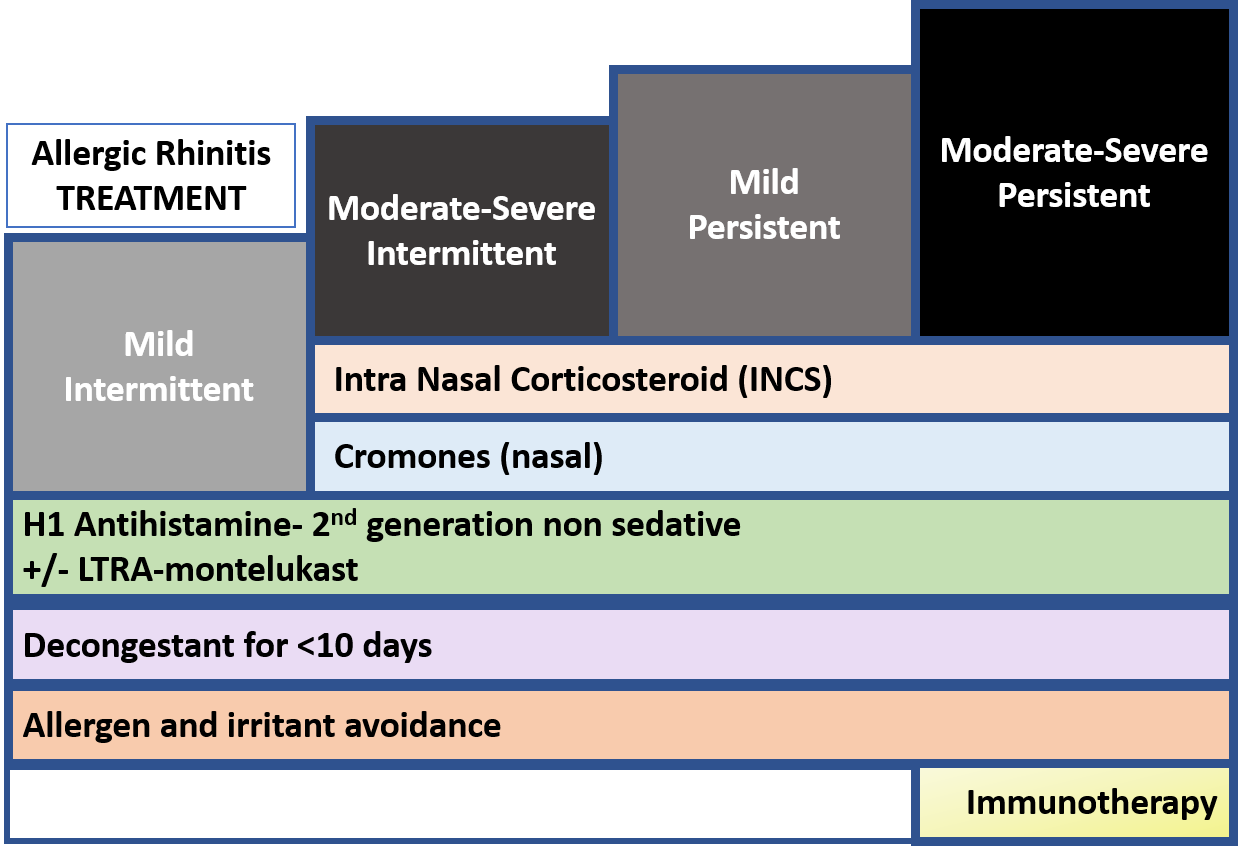
Earlier AR was classified as seasonal and perineal, however, the more recent classification of its types is Intermittent and Persistent (given by Allergic Rhinitis and Its Impact on Asthma – ARIA consensus). The severity is defined based on the impact on daily activities and sleep.



TREATMENT AND CONTROL
Allergen and Irritant avoidance: Allergic rhinitis is triggered by allergens (house dust mite, pollen/grass/ragweed, molds, insect, animal hair or some food items). However, symptoms can be exaggerated or flared up by irritant substances like cigarette smoke, wood smoke, industrial/automobile exhaust, VOC chemicals, perfumes, colognes, cosmetics, hair dyes or sprays, AC blasts, and even cold and damp air or places, which may not affect the general population as much. Therefore, for people with AR, it is essential to not only avoid the causative allergen but also such irritants. Maintaining an allergy diary to understand and avoid the responsible allergens and irritants is useful. Regular vacuuming and ventilating the house, and washing of sheets/linen can also be beneficial.
Antihistamines are agents that prevent the action of histamine once released, by blocking the target receptors (H1) through which it acts. These include first-generation sedative ones like chlorpheniramine, and second-generation less/non-sedating ones like cetirizine, levocetirizine, loratadine, desloratadine, fexofenadine, ebastine, bepotastine and bilastine. The second-generation antihistamines are one of the first-line medicines for managing AR and these are available as oral tablets, and nasal sprays/eye drops (azelastine, olopatadine).
Decongestants are medicines that constrict blood vessels and therefore relieve stuffiness and congestion. They are available as oral tablets (phenylephrine, pseudoephedrine) in combination with antihistamines or as nasal spray/drops (xylometazoline, oxymetazoline, naphazoline). They should be used only for the initial few days to relieve nasal stuffiness and enable sleep.
Corticosteroids act by stabilizing mast cells, reducing the release of histamine and also inhibiting the release of other inflammatory mediators. They are used in moderate-severe intermittent AR and persistent AR and are prescribed as nasal sprays often along with a course of oral antihistamines. Examples include budesonide, fluticasone, mometasone and ciclesonide nasal spray. Corticosteroid nasal sprays are the most effective in controlling all symptoms of AR and provide long-term relief. They are also available as combination nasal sprays with antihistamines.
Cromones are a group of medicines available as nasal sprays and eye drops (sodium cromoglycate and nedocromil), which also act by stabilizing mast cells and reducing histamine release.
LTRA (Leukotriene receptor antagonist) drug montelukast prevents the action of the allergy mediators cys-leukotrienes, and is a useful drug for AR, especially in patients who have co-existing asthma. This is also available as combination tablets with antihistamines.
Biological (Anti IgE monoclonal antibody) injectable drug omalizumab though approved for asthma, has been seen in studies to also have benefit in severe AR, especially if accompanied with asthma.
Allergen immunotherapy, also known as desensitization or hypo-sensitization, involves exposing a person to regular small doses of an allergen in an attempt to ‘acclimatize’ and reduce the immune system’s response against it. This is done after a process of allergy testing to identify the involved allergen/s. Allergy testing can be through the skin prick test (SPT) or blood test (radioallergosorbent test-RAST). Immunotherapy is given as injections (allergy shots) or by mouth as tablets/drops under the tongue (Sublingual Immunotherapy -SLIT).


Alternative therapies like homeopathy and acupuncture have been used with some success in allergies. Some research points towards restoring gut bacteria with probiotics as a possible benefit in AR. Irrigating the nasal passage with saline water on a regular basis is also recommended by some, but this has to be done in a guided and cautious way. Various herbal remedies like ginger, onion, garlic, turmeric, stinging nettle, elderberry, honey, lemongrass, parsley, Indian basil (Tulsi), butterbur and spirulina, are available as teas and supplements, and used by experience. However definitive clinical evidence is lacking and effects may take time and be variable. As people with AR are also predisposed to common (viral) cold and ear/sinus infections, they are sometimes prescribed vitamin C based supplements.
Also read:
Common Cold and Flu- Know the difference, effective care and 10 alert signs
For any query, additional information or to discuss any case, write to info@drvarsha.com, and be assured of a response soon.
References