Quick read: 5 Important points for Acne prone skin
ACNE – HOW AND WHY DOES IT OCCUR?
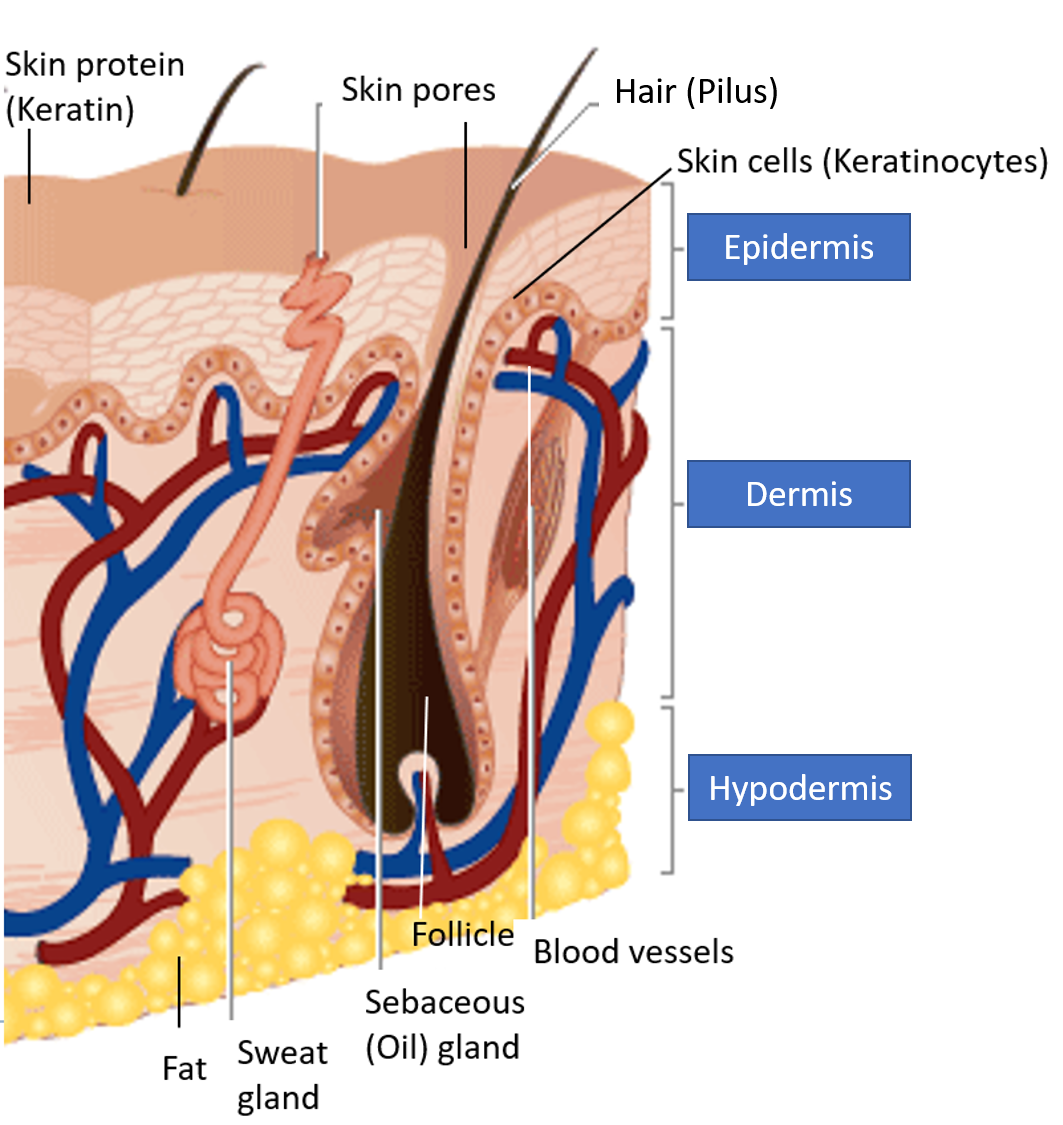
Skin Structure
The main skin cells which make up the outer layer of the skin (epidermis) are called keratinocytes as they synthesize the protein keratin which forms the outer protective coat of the skin. The epidermis also has cells called melanocytes which contain melanin pigment and give skin its characteristic color.
The skin contains hair follicles in the dermis (the middle layer of skin) from which hair (also called pilus, plural-pili) arise, and emerge out through pores on the skin surface. The hair follicles are nourished with oils and fats (called sebum) from the attached sebaceous glands. Therefore, each hair follicle and the attached sebaceous glands are together called a Pilo-Sebaceous Unit (PSU).


Developement of Acne
Increased multiplication and accumulation of the keratinocytes lining the hair follicles (called follicular hyper-keratinization), and increased production of sebum from the sebaceous glands (called hyper-seborrhea), can cause the pores of the follicles to get blocked. This leads to the development of acne (also called acne vulgaris).
The most common cause for this is a spurt in androgen hormones during puberty, which is why acne is typically known to be a teenage disease. However hormonal imbalances can occur later in life also. This is seen sometimes during certain days of the menstrual cycle, pregnancy, and conditions like Poly Cystic Ovarian Disease/Syndrome (PCOD/PCOS).
Other risks and contributing factors include certain skin-care product ingredients and cosmetics, stress, lifestyle and dietary factors. Acne occurs most commonly on the face (cheeks and forehead) but can also occur on the chest, upper back, and shoulder.
Stages and Manifestations of Acne
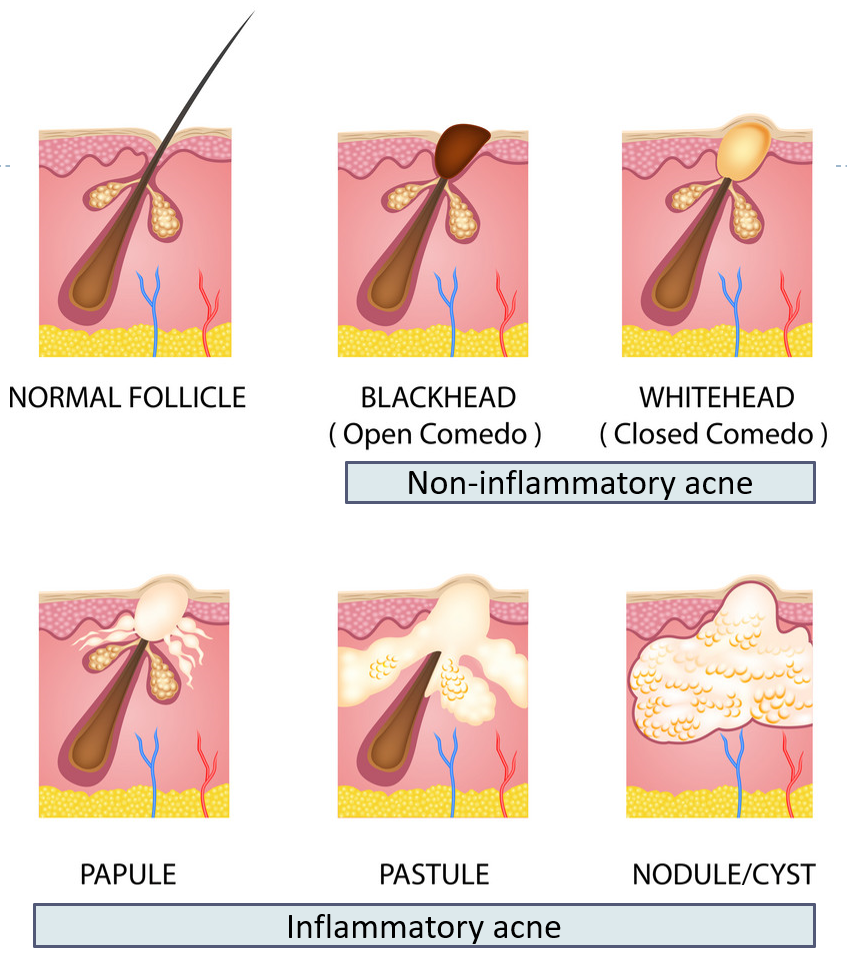
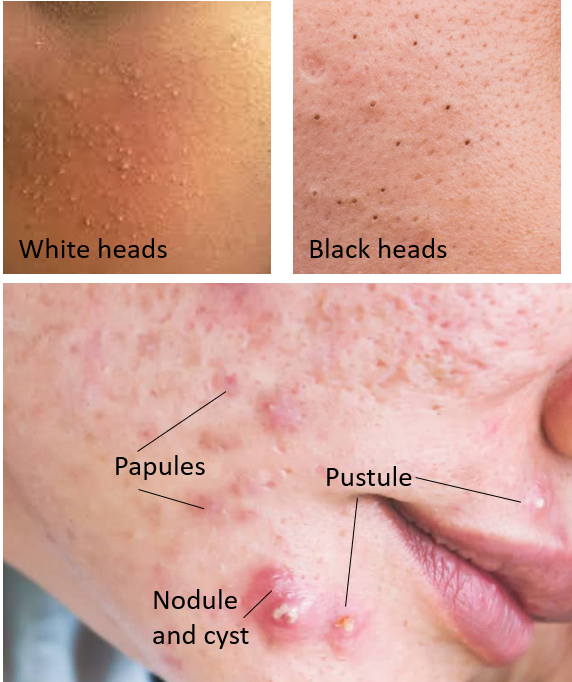
When the pore of the PSU gets blocked, it is called a comedo or comedone, and acne is said to be in the non-inflammatory stage. Comedones are the characteristic feature of acne vulgaris and can appear black (open comedo- blackhead) or white (closed comedo- whitehead: when it gets covered by the skin keratin). Within the hair follicle, reside bacteria called Propionibacterium acnes (also called Cutibacterium acnes) which are normally not active as they cannot multiply and thrive in the presence of oxygen (anaerobic bacteria).
Once the pore is closed, these bacteria start actively multiplying and thrive on the increased oils and fats present. This causes infection and inflammation of the PSU. This is the inflammatory stage of acne. It manifests as pimples or zits which may be papules (red, raised in appearance), pustules (filled with pus), or enlarged nodules and cysts (filled with cheesy material or fluid).




TREATMENT AND HEALTH SOLUTIONS FOR MANAGING ACNE
Acne is of concern mainly for cosmetic reasons (especially in teenagers and young unmarried age groups). This is due to the pimples or the scars left behind as a result of inflammation, more notably with nodules and cysts. Acne can also have a psychological impact necessitating counseling and addressal of associated depression and anxiety.
Managing acne should be by a combination of lifestyle modification, appropriate medicines, and where required, skin procedures. People with acne or acne-prone skin should take care of their diet, physical activity, stress, and very importantly what skin-care products they use. It is also important to select the right face wash.
(Read Important points of care for acne-prone skin).
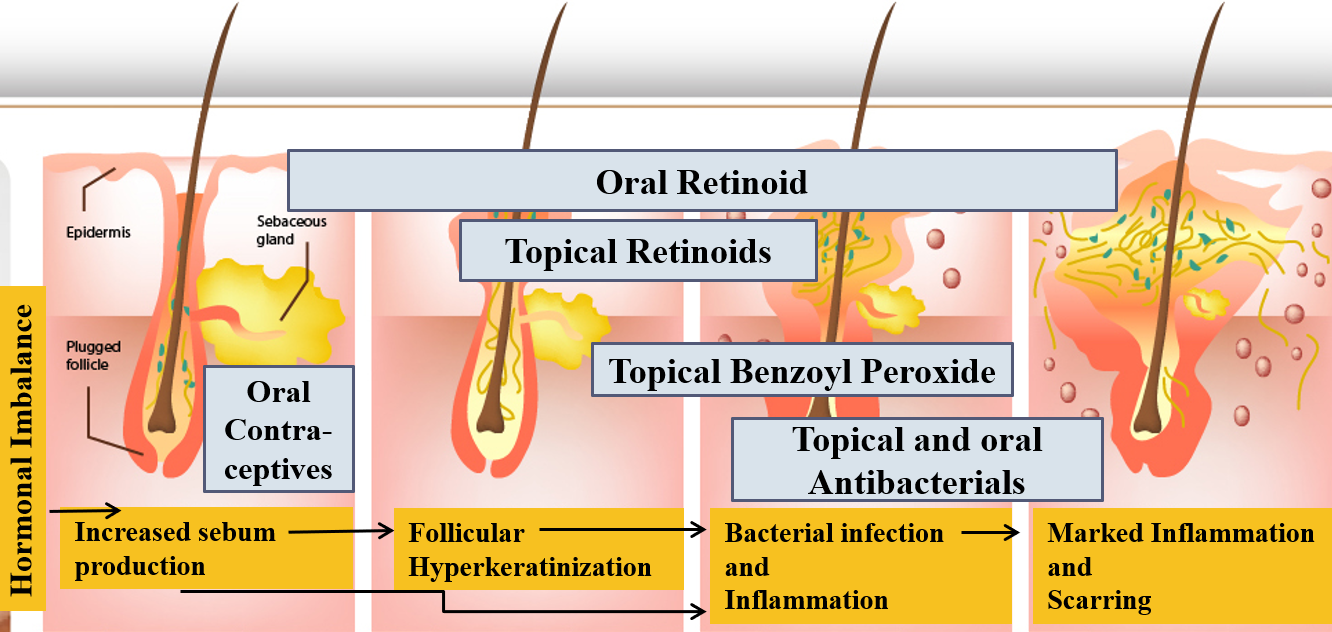
Medicines used for acne act through different mechanisms as shown. These may be topical (as creams and gels to apply on the affected skin) or oral tablets.
Topical medications
Among topical medications, retinoids (like adapalene, tretinoin, tazarotene, trifarotene), antibiotics (clindamycin, nadifloxacin, azithromycin, erythromycin) and benzoyl peroxide (BPO) are the most commonly used either singly or in combinations. Usually, in the non-inflammatory comedogenic phase, retinoids are used alone. However, BPO is added in the inflammatory phase, while antibiotics are added especially if pustules are present. Combinations of retinoids with BPO, and antibiotics (clindamycin, nadifloxacin) with BPO or with retinoids, are available.
Many of these agents can cause significant skin dryness and irritation on exposure to sunlight. To overcome this, some agents like retinoids are prescribed for night-time use only and initially as ‘short contact therapy.’ ‘Micro or nano’ formulations are also available for better tolerance and action. Nano-therapeutics is now evolving globally as an effective approach.
Other topical medications for acne include niacinamide, zinc salts, azelaic acid, dapsone and herbal agents like aloe vera. Topical agents like glycolic acid and salicylic acid are commonly part of acne face washes and peels.


Oral medications
Oral medications for acne mainly include antibiotics (azithromycin, doxycycline, minocycline), oral retinoids (isotretinoin) and oral contraceptives. Among the oral antibiotics, only azithromycin can be used in pregnancy. Some of these antibiotics are available as low-dose extended-release (ER) formulations to improve action and reduce side effects.
Pulse therapy or intermittent therapy may also be used to reduce side effects. Isotretinoin can cause many side effects like severe dryness of skin/lips/eyes, drowsiness, back/joint pains and psychological effects. Isotretinoin also causes abnormalities in the fetus, therefore pregnancy should be ruled out before, and strict contraception is to be adhered to while taking Isotretinoin.
Oral contraceptives are used in women due to the suppressive effect of estrogen hormone on androgens and sebum production. All the acne medicines should be taken only under the doctor’s prescription, guidance and monitoring.
Procedures
Procedures like skin peels, laser therapy and skin polishing are also available and performed by experienced Dermatologists to treat acne resistant to medicines, and when there is associated scarring.
OTHER RELATED CONDITIONS
Acne vulgaris versus Acne rosacea
The term ‘acne’ commonly used as in the entire discussion above refers to ‘acne vulgaris’. Another condition called acne rosacea (or just rosacea) is seen more often in middle age women (especially with light fair skin). It manifests as redness of the cheeks and nose due to swelling and prominence of the small blood vessels in the area. It can also be associated with pimples just like in acne vulgaris. Some of the triggers include hot/spicy foods, alcohol, smoking, extreme temperatures, wind, emotional stress, intense physical activity and some drugs/cosmetics.
Rosacea is treated by avoiding known triggers, and with medicines to reduce redness (like brimonidine, oxymetazoline), anti-parasitic agents (like metronidazole, ivermectin), anti-acne drugs like isotretinoin and doxycycline, and antihistamines or aspirin for itching and flushing symptoms. Sometimes laser therapy may be tried.
Folliculitis, Furuncles (Boils) and Carbuncles
These are terms to describe the infection and inflammation of the hair follicles that can occur in anyone at any age. The causative bacterium is usually Staph aureus. Common predisposing factors are improper hygiene, tight clothes, heat with moisture, cuts/injuries, and sometimes an underlying immune deficiency or poor nutrition. Folliculitis is a hair follicle infection confined to the upper outer layer of the skin (epidermis). A furuncle implies deeper infection in the dermis. These appear as pus-filled bumps (boils) and so can be confused with pimples, but are painful on touching, which differentiates them from acne. Furuncles can sometimes join together to form a larger carbuncle.
These bacterial skin infections are treated by topical antibiotics (like mupirocin, fusidic acid, framycetin, neosporin) and sometimes oral antibiotics in case of larger deeper infections.
Also read:
Skin Infections – Types, Predisposing Factors and Health Measures
For any query, additional information or to discuss any case, write to info@drvarsha.com and be assured of a response soon.